Treating Acne in Indian Skin

The Essential Info
As we see in all ethnicities, acne is common in Indian people.
Like any non-Caucasian ethnicity, Indian people also experience frustrating amounts of hyperpigmentation (dark/red spots left behind after an acne lesion heals).
Treatment for acne is usually the same regardless of skin color, but people with darker skin should ask more questions if they decide to try laser therapy, chemical peels, or photodynamic therapy, which are all treatments that can cause changes in pigmentation.

The Science
- Overview
- Clinical Trials and Studies
- What Is Different about Indian Skin?
- How to Treat Acne in Indian Skin
- The Bottom Line
Overview

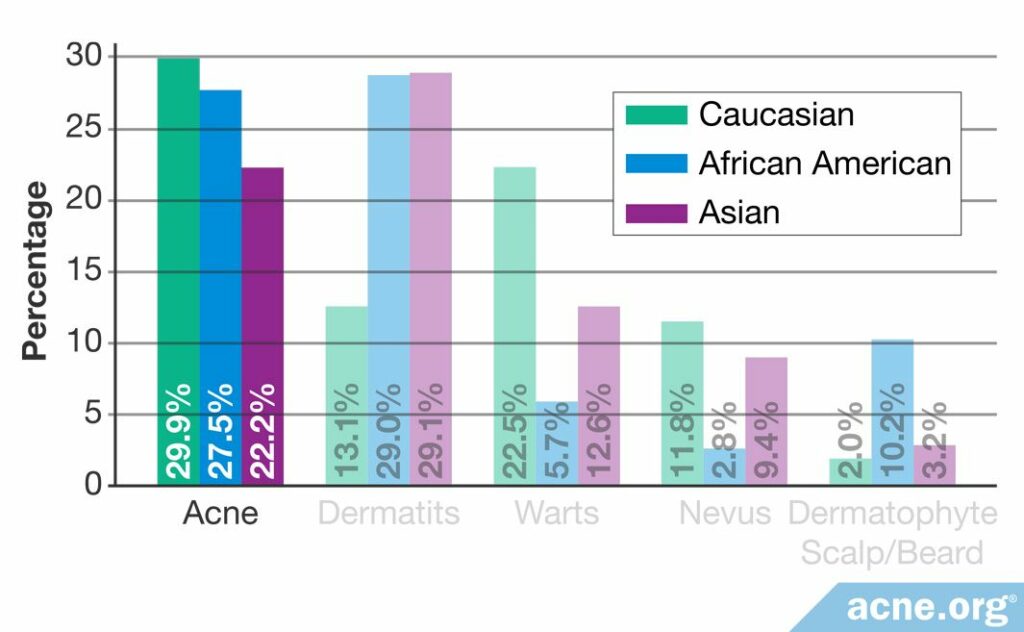
In India, similarly to other places in the world, acne is the most common skin disease and affects a large percentage of people. The Indian Acne Alliance notes that “acne is believed to be as common in India as it is in European Union (EU) and USA.”1 However, researchers have performed few studies specifically on people of Indian origin. There is some evidence that Asian children and adolescents may suffer from acne somewhat less than those of other ethnicities. And broadly speaking, “Asian” includes India, which is considered a South Asian country. However, in the studies on Asian children, the exact location of the children is not specified.2
Clinical Trials and Studies
When we look specifically at the studies that present evidence on people with Indian skin in particular, we see:
- Indian adult women experiencing the least amount of adult acne compared to women of other ethnic backgrounds.
- Indian people of all ages and genders experiencing a high rate of acne scarring.
- Indian people of all ages and genders experiencing a low rate of hyperpigmentation.
However, the data is just coming in and as future studies look at various ethnicities, these findings could change.
Expand to read details of studies

The one study we have comparing people of Indian descent with people of other races was performed in the United States and not in India.This study looks at Indian women, and was published in 2011 in the Journal of the European Academy of Dermatology and Venereology.
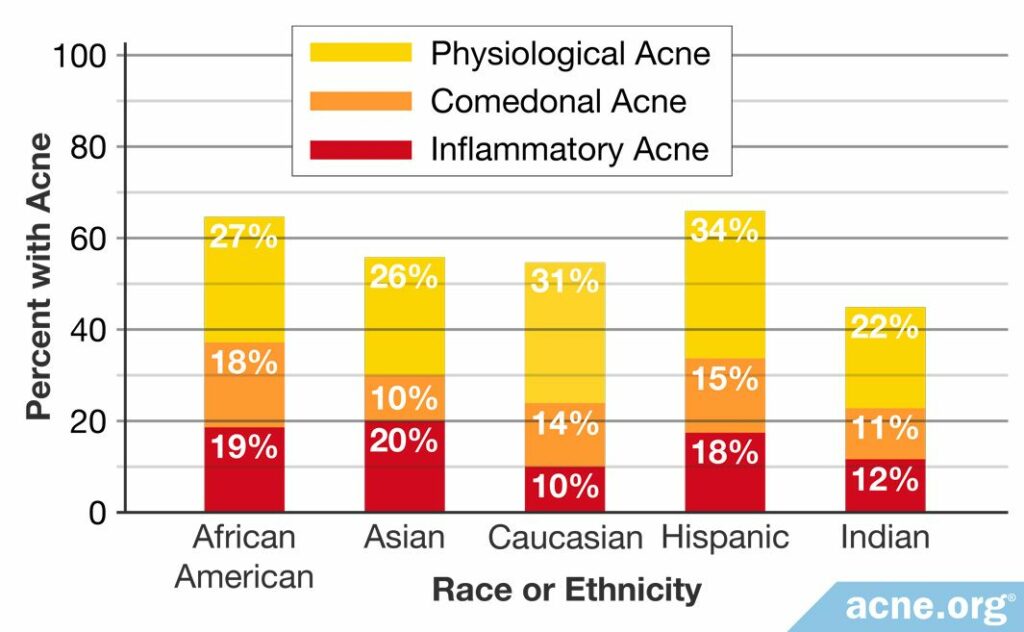
Researchers examined 2895 women of various ethnicities in the United States. Overall incidence of acne in Indian women was lower than in any other ethnicity, including in African American, Asian (East Asian in particular), Caucasian, and Hispanic women. When the researchers separated out types of acne, they saw that Indian women had the least amount of physiologic acne, a milder form of acne common in adult females. Indian women also showed a low incidence of both comedonal acne, which includes whiteheads and blackheads, as well as inflammatory acne, which includes red, sore pimples or “zits,” in addition to severe lesions like nodules and cysts.3

Another recent study was published in the Indian Journal of Dermatology, Venereology and Leprology in 2017.
Researchers examined patients of all ages who showed up at an Indian hospital and determined which were acne patients and what their characteristics were. They then compared their results with the results of previous studies of other ethnicities. The reliability of the study results are limited, however, in that the study design does not directly compare various populations. It instead simply compares results of a study on only 309 Indian patients with those of previous studies performed by other researchers in other areas. Even though we cannot count on the data, we will examine it nonetheless since we have such little data on Indian people and acne. Results showed that only 1.06% of the total patients in India were acne patients. This was far lower than the prevalence shown in previous studies in other populations. Why this was the case is not known. It could be that Indian people display a somewhat lower incidence of acne, or more likely, that Indian people do not seek treatment for acne as much as people in other countries. When it came to acne scarring, they found that Indian acne patients tended to suffer from acne scarring at a high rate compared to those of other populations. Only Senegalese (West African) women had slightly more scarring. Regarding postinflammatory hyperpigmentation (the dark/red marks left behind after acne lesions heal), Indian acne patients had less than people of other ethnicities examined in other studies. This lower amount of hyperpigmentation is contrary to what doctors in the real world, who say they see a high amount of hyperpigmentation in Indian patients, claim.
As stated, data is still coming in and current findings could change over time. The table below summarizes the comparative studies and their findings that we have so far.2


One more study was published in the Journal of Cosmetic Dermatology in 2021. This study looked at adults in India to determine how common acne was among them. Out of 24,056 study participants, 180 people, or less than 1%, had acne. Adult acne was much more common in Indian women than in Indian men, with 81.7% of the acne sufferers being women. The average age of adults with acne was 30.1 years. Acne lesions were mostly inflammatory, and the vast majority of acne lesions were located on the cheeks. In addition, over half of Indian adults with acne in this study developed acne scars.4

What Is Different about Indian Skin?

More similarities than differences: Regardless of whether studies show us differences between people with skin of color, in the real world, there are far more similarities than there are differences. For instance, data shows that people with Indian skin experience less hyperpigmentation compared to other ethnicities, but doctors will tell you that people with Indian skin experience hyperpigmentation right on par with other people of “Asian” origin.12
Sensitive skin: As outlined in a 2016 article in the Journal of Cutaneous and Aesthetic Surgery, Asian skin in general is considered to be more sensitive and prone to irritation than the skin of other ethnicities.13 However, the authors mentioned that they saw this most strongly in East Asian skin. Whether Indian people, who are considered South Asian, are also more prone to sensitive skin is still up for debate.
One recent study concluded the opposite, namely, that sensitive skin may be less common in India than in other countries. Still, the researchers found that about one-third of the Indian population possesses sensitive skin. The scientists also found that Indian people with sensitive skin were 2-4 times more likely to suffer from acne compared to those without sensitive skin.14
Expand to read details of study

The study was published in the journal Frontiers in Medicine in 2019. The researchers performed a nationwide survey of 3,012 people in India who were at least 15 years old. They found that 27.9% of men and 36.7% of women in India report having sensitive or very sensitive skin. The researchers wrote, “[A]lthough less frequently reported than in other countries, sensitive skin is a frequent condition in India, affecting about one third of the population.”14
Indian cultural skincare practices: Indian people sometimes use traditional practices such as using vegetable oils, coconut oil, almond oil, olive oil, and rye oil as moisturizers, which are comedogenic (tend to clog pores). These oils as such may aggravate acne or cause new acne lesions to appear.15
How to Treat Acne in Indian Skin

Acne develops in the same way regardless of skin color and is treated in the same way in people of every ethnicity. Acne can be effectively treated with topical medications, particularly with a properly applied benzoyl peroxide regimen. Doctors sometimes prescribe the oral medication Accutane®(isotretinoin) to people with severe, widespread, scarring acne as well. Dermatologists in India founded a group called the Indian Acne Alliance and in 2009 developed guidelines for management of acne.1 They recommend the use of benzoyl peroxide as a safe and effective therapy and “an excellent choice in the treatment of mild and moderate acne.”1 In these guidelines they also established, “Indians are more sensitive and less tolerant of topical retinoids than other ethnic groups.”
Retinoid medications include tretinoin, adapalene, and tazarotene. Adapalene is the least irritating retinoid and causes the fewest side effects in all people, including Indian people, and the guidelines further assured that it is possible to overcome intolerance to retinoids in the vast majority of Indian people.16
As for the treatment of postinflammatory hyperpigmentation, as with any other ethnicity, bleaching agents and/or exfoliating agents are recommended.12
The Bottom Line
Prevention is key. Get yourself completely cleared up so that you are actively preventing future acne lesions, hyperpigmentation, and scarring. Then, if you so desire, you may employ one of the various methods of treating hyperpigmentation.
References
- Kubba, R. et al. Acne in India: Guidelines for management – IAA consensus document. Indian J Dermatol Venereol Leprol 75, 1 – 2 (2009). https://pubmed.ncbi.nlm.nih.gov/19282578/
- Adityan, B. & Thappa, D. M. Profile of acne vulgaris-A hospital-based study from South India. Indian J Dermatol Venereol Leprol 75, 272 – 278 (2017). https://pubmed.ncbi.nlm.nih.gov/19439880/
- Perkins, A. C., Cheng, C. E., Hillebrand, G. G., Miyamoto, K. & Kimball, A. B. Comparison of the epidemiology of acne vulgaris among Caucasian, Asian, Continental Indian and African American women. J Eur Acad Dermatol Venereol 25, 1054 – 1060 (2011). https://pubmed.ncbi.nlm.nih.gov/21108671/
- Shah, N., Shukla, R., Chaudhari, P., Patil, S., Patil, A., Nadkarni, N. & Goldust, M. Prevalence of acne vulgaris and its clinico-epidemiological pattern in adult patients: Results of a prospective, observational study. J Cosmet Dermatol 20, 3672-3678 (2021). https://pubmed.ncbi.nlm.nih.gov/33655630/
- Tan, H. H., Tan, A. W., Barkham, T., Yan, X. Y. & Zhu, M. Community-based study of acne vulgaris in adolescents in Singapore. Br J Dermatol 157, 547 – 551 (2007). https://pubmed.ncbi.nlm.nih.gov/17655737/
- Al-Ameer, A. M. & Al-Akloby, O. M. Demographic features and seasonal variations in patients with acne vulgaris in Saudi Arabia: a hospital-based study. Int J Dermatol 41, 870 – 871 (2002). https://pubmed.ncbi.nlm.nih.gov/12492972/
- Stathakis, V., Kilkenny, M. & Marks, R. Descriptive epidemiology of acne vulgaris in the community. Australas J Dermatol 38, 115 – 123 (1997). https://pubmed.ncbi.nlm.nih.gov/9293656/
- Kane, A., Niang, S. O., Diagne, A. C., Ly, F. & Ndiaye, B. Epidemiologic, clinical, and therapeutic features of acne in Dakar, Senegal. Int J Dermatol 46, 36 – 38 (2007). https://pubmed.ncbi.nlm.nih.gov/17919205/
- Kilkenny, M., Merlin, K. & Plunkett, A. M. The prevalence of common skin conditions in Australian school students: 3. acne vulgaris. Br J Dermatol 139, 840 – 845 (1998). https://pubmed.ncbi.nlm.nih.gov/9892951/
- Taylor, S. C., Cook-Bolden, F., Rahman, Z. & Strachan, D. Acne vulgaris in skin of color. J Am Acad Dermatol 46, 98 – 106 (2002). https://pubmed.ncbi.nlm.nih.gov/11807471/
- Yeung, C. K., Teo, L. H., Xiang, L. H. & Chan, H. H. A community-based epidemiological study of acne vulgaris in Hong Kong adolescents. Acta Derm Venereol 82, 104 – 107 (2002). https://www.researchgate.net/publication/11253329_Yeung_CK_Teo_LH_Xiang_LH_Chan_HHA_community-based_epidemiological_study_of_acne_vulgaris_in_Hong_Kong_adolescents_Acta_Derm_Venereol_82104-107
- Kubba, R. et al. Post-inflammatory hyperpigmentation in acne. Indian J Dermatol Venereol Leprol 75, 54 (2009). http://www.ijdvl.com/article.asp?issn=0378-6323;year=2009;volume=75;issue=7;spage=54;epage=54;aulast=Kubba
- Goh, C. et al. Meeting the challenges of acne treatment in Asian Patients: A review of the role of dermocosmetics as adjunctive therapy. J Cutan Aesthet Surg 9, 85 – 92 (2016). https://pubmed.ncbi.nlm.nih.gov/27398008/
- Brenaut, E., Misery, L. & Taieb, C. Sensitive skin in the Indian population: An epidemiological approach. Front Med (Lausanne) 6, 29 (2019). https://pubmed.ncbi.nlm.nih.gov/30842946/
- Kubba, R. et al. Factors precipitating or aggravating acne. Indian J Dermatol Venereol Leprol 75, 10 – 12 (2009). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6052742/
- Kubba, R. et al. Topical retinoids. Indian J Dermatol Venereol Leprol 75, 28 – 30 (2009). http://www.ijdvl.com/article.asp?issn=0378-6323;year=2009;volume=75;issue=7;spage=28;epage=30;aulast=Kubba
 Acne.org Products
Acne.org Products