Accutane (Isotretinoin) Is a Systemic Medication That Affects All Parts of the Body

The Essential Info
Isotretinoin, often known by its original brand name, Accutane®, despite being an effective acne treatment, comes with many side effects, some of which can be severe and/or long-term. If your doctor recommends isotretinoin, it is important to review your medical history with your doctor. Unless you are experiencing widespread, severe acne that is scarring, it is best to exhaust all other avenues of treatment before trying isotretinoin.
Skin and Mucous Membranes: Severely dry skin/lips and nosebleeds are expected, and anecdotal evidence points toward the possibility that dry lips in particular may be permanent.
Eyes, Psychiatric, Joints, Blood, Gut, Etc.: Because isotretinoin is an oral medication, it affects the entire body, and some patients may experience side effects elsewhere in the body, such as eye/vision problems, psychiatric symptoms, joint pain, blood imbalances, intestinal disorders, and many others. Some of these side effects may be lifelong.
BIRTH DEFECTS: Most important, and most disastrous, is the likelihood of severe birth defects and miscarriage. Isotretinoin is the #1 most birth-defect causing medication on the market. Women must absolutely avoid pregnancy since isotretinoin greatly increases the chance of birth defects.
My Experience: I took isotretinoin in college because I struggled with severe acne, particularly on my body. It completely cleared up my acne in the short term, but immediately after finishing my course, my acne returned, albeit at a lower level. I experienced severely dry, cracked, bleeding lips, nose bleeds, eyes that were so sensitive I could not watch movies, and severe joint pain. That was over 25 years ago, and I still have to use lip balm several times a day and my joints may not have ever fully recovered. Isotretinoin can be a godsend for some people with severe, widespread, and scarring acne, but it should be entered into extremely carefully, and only after considering the repercussions you may have to deal with forever.

The Science
- Most Common: Side Effects of the Skin, Mucous Membranes, and Eyes
- Less Common, but Still Expected: Side Effects of the Skull/Head, Musculoskeletal System, Liver, Blood/Hormones, and Intestines
- Controversial: Psychiatric Side Effects
- What to Keep an Eye on While Taking Isotretinoin
- Drug Interactions
- Who Should Not Take Isotretinoin

Isotretinoin, often known by its original brand name, Accutane®, is an oral medication that doctors sometimes prescribe to patients with severe acne. It is normally taken for 15-20 weeks and results in long-term remission of acne symptoms in up to 2/3 of people who take it.
While results are impressive, the side effects of isotretinoin are numerous and diverse.

An article published in The Cochrane Database of Systematic Reviews in 2018 combed through all the available evidence on the side effects of isotretinoin. The review authors found 14 randomized controlled trials, which are the most rigorous type of study on patients, with a grand total of 906 participants. None of the 14 studies reported any side effects of isotretinoin that were fatal, life-threatening, permanently disabling, or requiring hospitalization. However, 13 out of 14 studies reported a variety of other, less grave side effects, such as skin dryness and hair loss.1
The review authors also noted that the longest follow-up with patients in any of the studies was a year after they stopped taking isotretinoin. Therefore, it is possible that these studies may have missed some long-term side effects.1

Recently, the same researchers updated their literature search to include studies on isotretinoin published up until March 2020. Their new search confirmed that side effects from isotretinoin use were common but not life-threatening. Almost all patients experienced dry skin, lips, or eyes. Less common side effects included various muscle and joint symptoms, such as arthritis, tendinitis, and backache, as well as changes in lab test results like cholesterol levels. The researchers published their findings in the journal Expert Review of Clinical Pharmacology in 2020.2
Let’s have a look at the side effects more closely.
Most Common: Side Effects of the Skin, Mucous Membranes, and Eyes
The most common side effects of isotretinoin involve the skin, mucous membranes, and eyes, and affect almost every person who takes isotretinoin.
Skin and mucous membranes
Side effects of the skin and mucous membranes (membranes that line body cavities and secrete mucus) are common in patients treated with isotretinoin. The most common symptoms are dry lips, dry skin, inflammation of the lips, dry nostrils, and dry mouth.3
Expand to read details of studies

In an analysis published in 2001 in the Journal of the American Academy of Dermatology, McLane observed that over 90% of patients who experienced adverse side effects of the skin reported dry skin, localized exfoliation, rash, and dermatitis (a type of skin irritation).4

In a review published in 2013 in the Expert Opinion on Drug Safety, Tripathi et al. reported that:
- 100% of patients experienced lip dryness
- 95% of patients experienced cheilitis (inflammation of the lips)
- 50% of patients experienced dryness of the nostrils
- 40% of patients experienced dryness of the oral mucosa (mucous membrane lining the inside of the mouth)5

In 2020, a group of researchers looked specifically at 15 studies that had tested low doses of isotretinoin on patients. The researchers published their conclusions in the journal Dermatologic Therapy. They found that for low-dose isotretinoin, the most common side effect was cheilitis, meaning red, dry, and itchy lips.6
Eyes
Side effects related to eye irritation may be short term or long term and include intolerance to contact lenses, increased S. aureus bacteria infections, and light sensitivity.4 Rare side effects include night vision disorders and corneal opacity (scarring or clouding of the cornea, the eye’s outermost layer).3
Expand to read details of studies

In the Journal of the American Academy of Dermatology, McLane noted that dryness and irritation of the eyes occurs in 28% of patients taking isotretinoin.4

In a study published in the Archives of Dermatology, Neudorfer found that:
- 28% of patients experienced eye dryness and irritation
- 13.8% of patients experienced persistent adverse effects of the eyes after the end of treatment5
Neudorfer’s findings also indicated that isotretinoin increased the risk of conjunctivitis (pink eye) by 1.7 times. Additionally, isotretinoin use was associated with an increased risk for developing hordeolum (painful bumps around the eyelid), chalazion (inflammatory lump near tear gland), and blepharitis (inflammation of the eyelid).7
Less Common, but Still Expected: Side Effects of the Skull/Head, Musculoskeletal System, Liver, Blood/Hormones, and Intestines
Other side effects of isotretinoin include headaches, musculoskeletal disorders like joint pain, liver problems, and potentially intestinal conditions.3
Expand to read details of studies

A study published in the journal BMC Musculoskeletal Disorders in 2020 found that isotretinoin caused side effects in muscles and joints in a large number of patients. Among 94 patients taking isotretinoin:
- 70.2% experienced lower back pain
- 53.2% experienced myalgia (muscle pain)
- 47.9% experienced joint pain
- 4.3% experienced tendon injuries8

In a review published in Clinical Dermatology in 2010, Rigopoulos et al. notes that headaches are rare but might be due to intracranial hypertension, which is high pressure of the fluid surrounding the brain and spinal cord. About one third of isotretinoin patients can expect joint aches. Rigopoulos et al. also reported that hepatitis is a less common side effect. Inflammatory bowel disease is a rare side effect.3

Pituitary hormones control many processes in the body such as sleep cycles, metabolism, and sex hormone production. In a study published in Dermatology in 2015, Karadag et al. reported that isotretinoin decreased pituitary hormones in a dose-dependent way; in other words, the higher the dose, the lower the hormone levels.9

Isotretinoin treatment also affects blood cell counts, triglyceride (fat/lipid) levels, and cholesterol levels, summarized in the table below. However, it is worth noting that in a meta-analysis published in JAMA Dermatology in 2015, Lee et al. found that the proportion of patients with these abnormalities was low.10
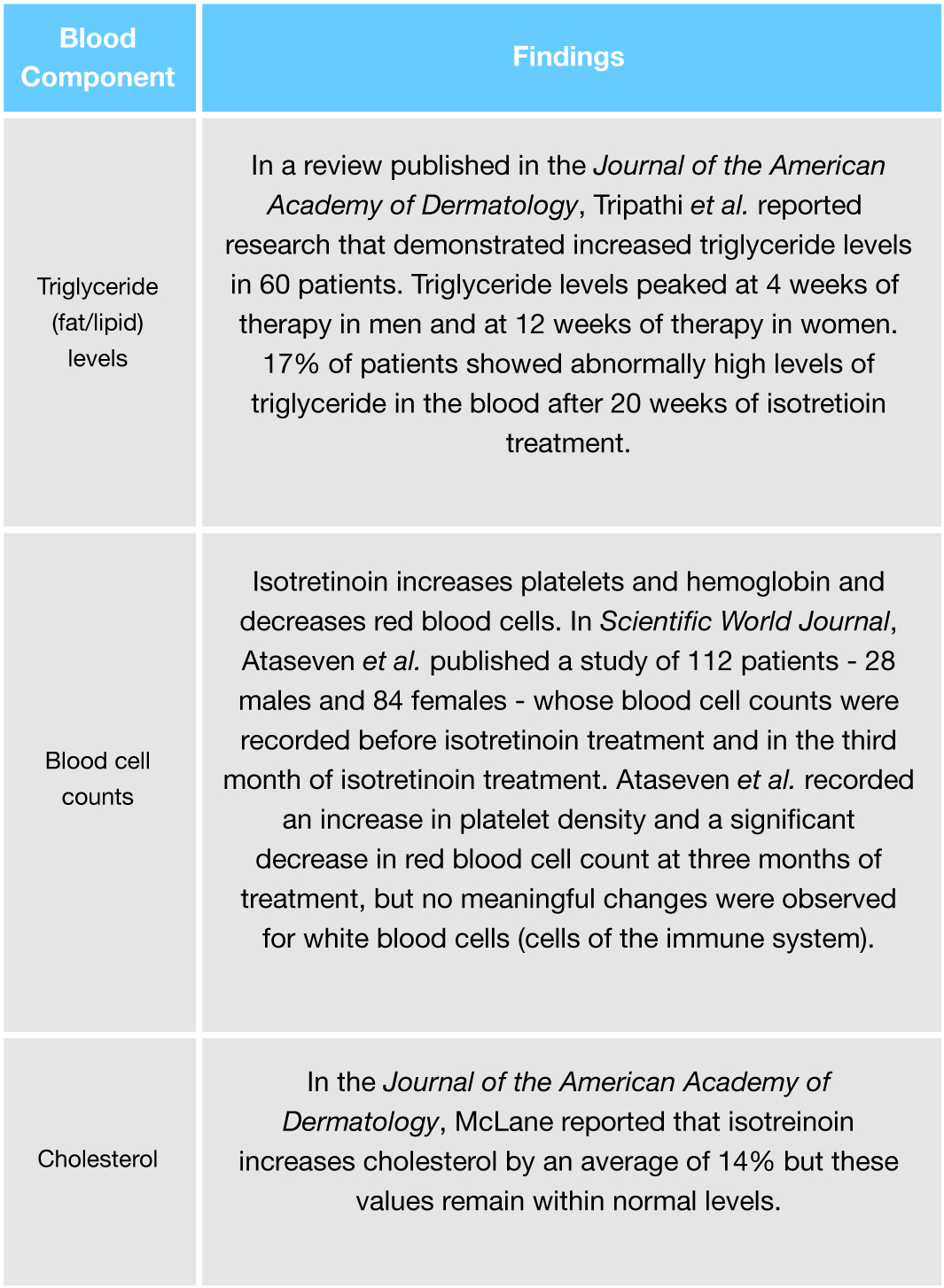
Controversial: Psychiatric Side Effects
Some psychiatrists have reported a connection between isotretinoin and psychiatric conditions such as depression, suicidal ideation, and suicide.3 However, scientists have found no conclusive proof that isotretinoin causes these conditions, so this issue remains controversial.
Dermatologists argue that acne itself causes depression, pointing out that isotretinoin can have a positive effect on mood because it clears up acne and improves self-image.12,13
Expand to read details of studies

In the journal Clinical Dermatology, Rigopoulos et al. reported that, “A retrospective cohort study reviewed the supposed risk of depression, psychotic symptoms, attempted suicide, and suicide with isotretinoin therapy. No evidence was provided to support that use of isotretinoin was correlated with an increased risk of depression, suicidal behavior, or other psychiatric disorders. Another study found no association with suicidal behavior and treatment with isotretinoin.”3

In a review published in Archives of Dermatology, Goldsmith et al. points out that “Epidemiological studies to date have not shown an association between isotretinoin and depression or suicide because acne itself may be a risk factor for depression.”12
However, psychiatrists suggest a causal relationship between isotretinoin and depression. Psychiatrists argue that dermatologists are unable to identify these conditions correctly. While the evidence that isotretinoin causes adverse psychiatric orders is not definitive, dermatologists are advised to check their patients’ medical histories and check their patients’ mental well being at each visit.3,13
Concerning: Long-term Side Effects
The long-term effects of isotretinoin therapy are not well studied. In fact, we have only one study which looks at long-term side effects.

This study published in the British Journal of Dermatology assessed long-term side effects in 720 patients treated with isotretinoin. The follow-up period of this study ranged from 2 to 12 years. The study found that 52 patients (7.2%) reported persistent side effects during the follow-up period, predominantly joint aches and dry skin. Goulden et al. reported no correlation between side effects and age, sex, cumulative dose, or number of treatments.14
Anecdotal evidence suggests that many people who take isotretinoin tend to use lip balm for decades after taking isotretinoin. Isotretinoin reduces skin oil production long term. What role this plays long term in the health of the skin and in skin aging remains to be studied.
What to Keep an Eye on While Taking Isotretinoin
Doctors should check patients for changes in blood parameters, such as blood cell and triglyceride counts, as well as changes in mood and vision while taking isotretinoin.5,12 Some researchers argue that monthly monitoring of blood parameters is not necessary, suggesting that doctors may check blood parameters every two months to reduce costs.13
Some skin, mucous membrane, and eye side effects are manageable with complementary therapies such as skin lotions, sunscreen, petroleum jelly, and similar products.
Some eye problems can be decreased by avoiding contact lenses and by eye washing. Visions problems, with the most notable being a rapid decrease in night vision, may require discontinuing isotretinoin therapy.4
Drug Interactions
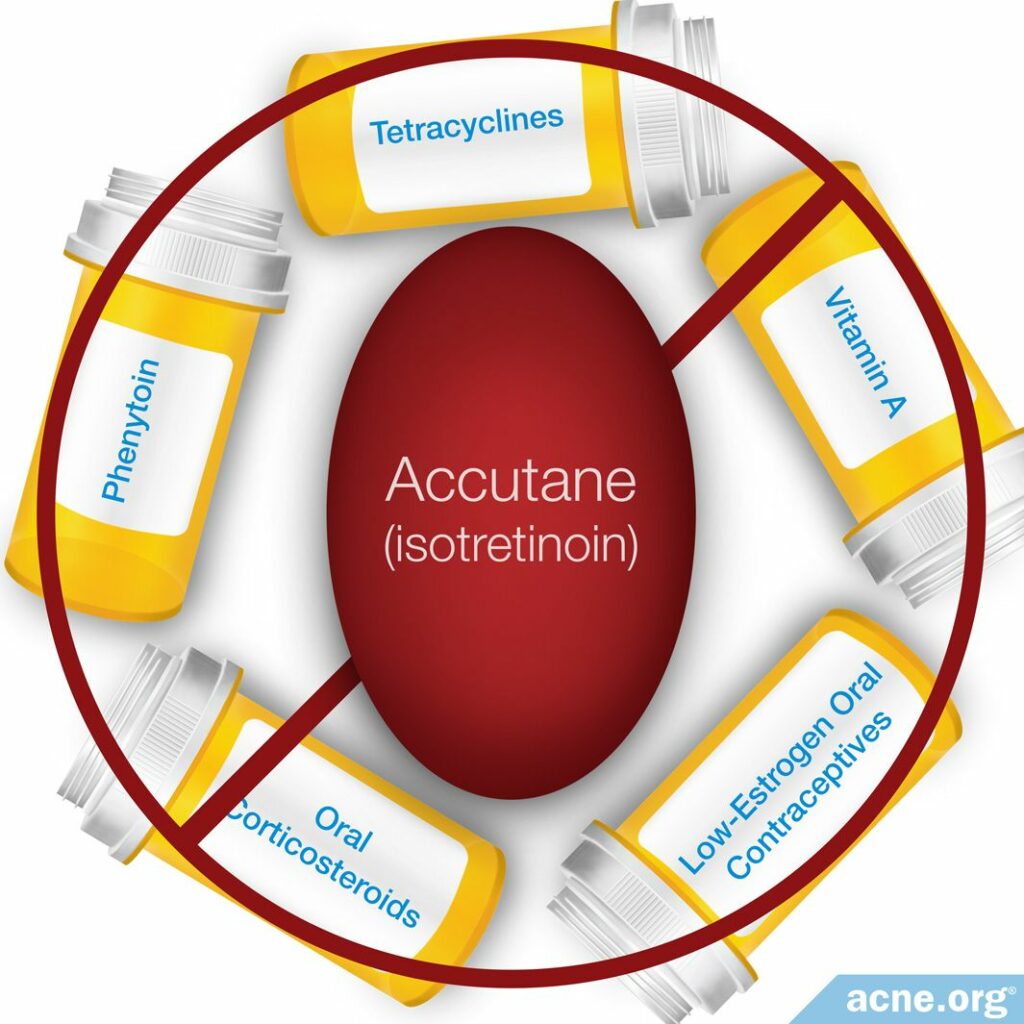
Isotretinoin can interact with some drugs, and patients taking phenytoin, tetracyclines, vitamin A, low-estrogen oral contraceptives, and oral corticosteroids should not take isotretinoin.3
Who Should Not Take Isotretinoin

Women who are or who may become pregnant: Women cannot take isotretinoin during pregnancy or when there is any possibility whatsoever that they may become pregnant because it greatly increases the risk of birth defects.3 Isotretinoin is the most teratogenic (causes birth defects) medication on the market.
Birth defects include malformations of the brain, skull, face, and heart, as well as miscarriage and death.4
Therefore, the FDA and EU have created programs to prevent pregnancy in patients taking isotretinoin. These programs require using two effective birth control methods from one month before isotretinoin treatment to five weeks after treatment, preferably including oral contraceptives.4,12,15 These programs also test for pregnancy before, during, and after treatment.3 In the United States, iPLEDGE is the pregnancy risk management program for isotretinoin administration. Prescribers and patients can access the iPLEDGE registry at www.ipledgeprogram.com.
People with liver problems, kidney problems, diabetes, high blood lipids, or alcoholism also should not take isotretinoin.3
References
- Costa, C. S., Bagatin, E., Martimbianco, A. L. C. et al. Oral isotretinoin for acne. Cochrane Database Syst. Rev. 11, CD009435 (2018). https://www.ncbi.nlm.nih.gov/pubmed/30484286
- Bagatin, E. & Costa, C.S. The use of isotretinoin for acne – an update on optimal dosing, surveillance, and adverse effects. Expert Review of Clinical Pharmacology 13, 885-897 (2020). https://pubmed.ncbi.nlm.nih.gov/32744074/
- Rigopoulos, D., Larios, G., & Katsambas, A. D. The role of isotretinoin in acne therapy: why not as first-line therapy? facts and controversies. Clinical Dermatology 28, 24-30 (2010). https://www.ncbi.nlm.nih.gov/pubmed/20082946/
- McLane, J. Analysis of common side effects of isotretinoin. Journal of the American Academy of Dermatology 45,188-194 (2001). https://www.em-consulte.com/en/article/559248
- Tripathi, S. V., et al. Side effects of common acne treatments. Expert Opinion on Drug Safety 12, 39-51 (2013). https://www.ncbi.nlm.nih.gov/pubmed/23163336
- Sadeghzadeh-Bazargan, A. et al. Systematic review of low-dose isotretinoin for treatment of acne vulgaris: Focus on indication, dosage, regimen, efficacy, safety, satisfaction, and follow up, based on clinical studies. Dermatologic Therapy 34, 1-39 (2021). https://pubmed.ncbi.nlm.nih.gov/33085149/
- Neudorfer, M., et al. Ocular adverse effects of systemic treatment with isotretinoin. Archives of Dermatology 148, 803-808 (2012). https://jamanetwork.com/journals/jamadermatology/fullarticle/1148708
- Karaosmanoğlu, N. & Mülkoğlu, C. Analysis of musculoskeletal side effects of oral Isotretinoin treatment: a cross-sectional study. BMC Musculoskeletal Disorders 21, 1-10 (2020). https://pubmed.ncbi.nlm.nih.gov/32977793/
- Karadag, A. S., et al. The effect of different doses of isotretinoin on pituitary hormones. Dermatology 230, 354-359 (2015). https://www.researchgate.net/publication/272835622_The_Effect_of_Different_Doses_of_Isotretinoin_on_Pituitary_Hormones
- Lee, Y. H., et al. Laboratory monitoring during isotretinoin therapy for acne. JAMA Dermatology 17033, 1 (2015). https://jamanetwork.com/journals/jamadermatology/fullarticle/2471551
- Ataseven, A. and Ugur Bilgin, A. Effects of isotretinoin on the platelet counts and the mean platelet volume in patients with acne vulgaris. Scientific World Journal 2014, 156464 (2014). https://www.hindawi.com/journals/tswj/2014/156464/
- Goldsmith, L.A., et al. American Academy of Dermatology Consensus Conference on the safe and optimal use of isotretinoin: summary and recommendations. Journal of the American Academy of Dermatology 50, 900-6 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15153892
- Ludot, M., Mouchabac, S., & Ferreri, F. Inter-relationships between isotretinoin treatment and psychiatric disorders: depression, bipolar disorder, anxiety, psychosis and suicide risks. World Journal of psychiatry 5, 222-227 (2015). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4473493/
- Goulden, V., Layton, A. M., & Cunliffe, W. J. Long-term safety of isotretinoin as a treatment for acne vulgaris. British Journal of Dermatology 131, 360-3 (1994). https://www.ncbi.nlm.nih.gov/pubmed/7918010
- Zouboulis, C. C. and Bettoli, V. Management of severe acne. British Journal of Dermatology 172, 27-36 (2015). https://www.ncbi.nlm.nih.gov/pubmed/25597508
 Acne.org Products
Acne.org Products