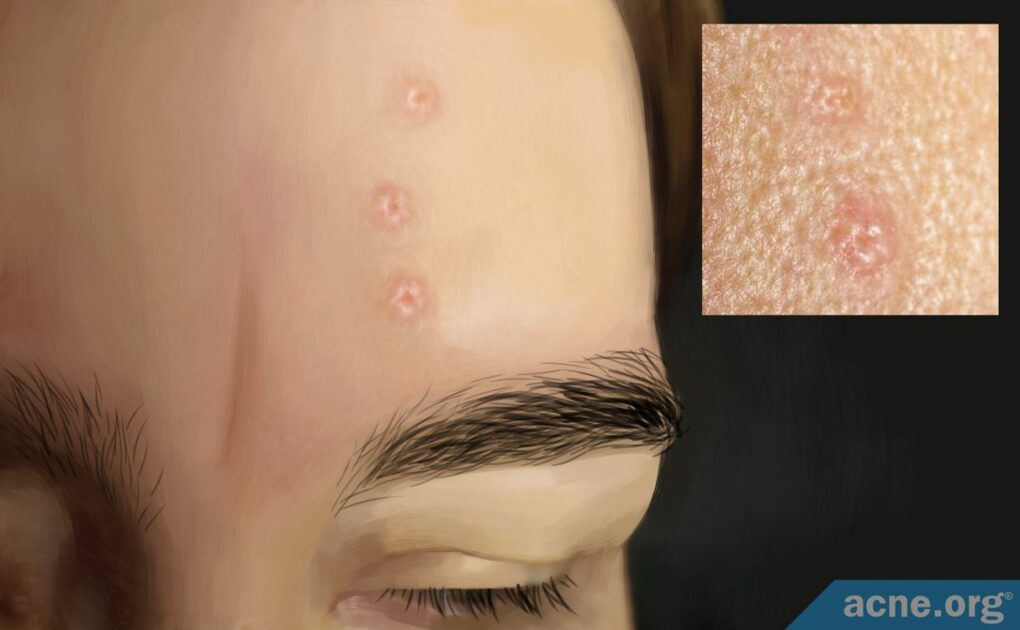
Sebaceous Hyperplasia Is a Harmless Skin Condition That Looks like Raised Bumps on the Face with Dimples in the Middle and Mainly Affects Older Adults. It Has No Connection to Acne.

The Essential Info
Sebaceous hyperplasia is a minor skin condition that occurs mostly in people over 40 when the glands that produce skin oil overgrow, resulting in bumps on the face with a small dimple in the middle of each bump.
The bumps in sebaceous hyperplasia are harmless but will not go away without treatment. There are many treatment options, such as:
- Laser therapy
- Cryotherapy (extreme cold)
- Surgical removal
Sebaceous hyperplasia is completely different from acne because:
- Sebaceous hyperplasia typically occurs in older adults, while acne usually occurs in teens and young adults.
- People with sebaceous hyperplasia tend to produce too little skin oil, while people with acne produce too much skin oil.
- Sebaceous hyperplasia is a minor nuisance that only affects the appearance of the face, while acne is a more serious condition that comes with soreness, itching, and discomfort.
Important: If you’re not sure the bumps you see are sebaceous hyperplasia, see a doctor to rule out other conditions that can look similar, like some types of skin cancer.
My Experience: Yup. I’m old 🙂 I have one sebaceous hyperplasia on my right cheek. At different times I have had it lasered, frozen, and burned (cauterized). Each of these things works in the short term, but it never goes away completely and always comes back, so I go in about once a year or once every other year and just do it again. I’ve seen different dermatologists, and each of them is confident that he/she knows a better way to get rid of it, but at least in my case, it’s persistent. It’s annoying but there’s not much else I can do about it other than keep getting treatments every so often to keep it at bay.

The Science
- How Can You Tell You Have Sebaceous Hyperplasia?
- Who Is at Risk
- Causes of Sebaceous Hyperplasia
- Treatments
- Sebaceous Hyperplasia Vs. Acne
Sebaceous hyperplasia is an overgrowth (hyperplasia) of the glands that produce skin oil (sebaceous glands). It shows up on the skin with one, or a few, bumps on the cheeks and/or forehead, with a dimple in the middle of each bump.
The bumps are caused by sebaceous glands that have grown to as much as 10 times their normal size. The overgrown glands are harmless but will not go away unless you see a doctor for treatment.1
How Can You Tell You Have Sebaceous Hyperplasia?
You may suffer from sebaceous hyperplasia if:
- Your skin has round, superficial bumps that measure 2 – 5 mm across and have a dimple in the center.
- The bumps are located alone or in groups on the forehead, nose, and/or cheeks, or, less commonly, on the back and/or chest.1,2
- The bumps stay in the same place and do not go away on their own.
- The bumps do not itch or hurt.
Who Is at Risk for Sebaceous Hyperplasia?
You are more likely to develop sebaceous hyperplasia if you:
- Are over 40 years old
- Have oily or combination skin
- Are immunosuppressed (have lowered immunity) due to an illness like AIDS or a medication you are taking, like cyclosporine
- Have direct relatives with sebaceous hyperplasia (it can be genetic)
- Suffer from a genetic skin disorder like Muir-Torre syndrome or pachydermoperiostosis1
Scientists estimate that about 1% of healthy people over the age of 50 have sebaceous hyperplasia. Among people who are over 50 and have other risk factors, such as taking immunosuppressive drugs, the percentage may be as high as 16%.3
Causes of Sebaceous Hyperplasia
Doctors are unsure what exactly causes the skin oil glands to overgrow in sebaceous hyperplasia. However, they suspect that these factors may contribute:
- A drop in male hormones (androgens): Androgens–male hormones that are also present in females–regulate how sebaceous glands grow and how much skin oil they produce. During adolescence, androgen levels tend to peak, and so does skin oil production, which is why acne is especially common during this time. For men, androgen levels begin to decline around age 40, while for women, they tend to drop after menopause. With less androgens in the body, the cells in the skin oil glands (sebocytes) no longer receive the signals they need to develop normally. These sebocytes get stuck in an undeveloped stage inside the skin oil glands. It is thought that perhaps the skin oil glands become enlarged as a result.4,5
- Sun damage: Exposure to sunlight without protection leaves the skin open to damage from the sun’s UV rays. When UV rays strike sebocytes, these cells can start overgrowing, leading to the enlargement of the skin oil glands. Therefore, one way to reduce your chances of developing sebaceous hyperplasia is to put on sunscreen when going outside for extended periods.5
- Taking cyclosporine: Cyclosporine is an immunosuppressant medication that doctors prescribe for rheumatoid arthritis, psoriasis, Crohn’s disease, or for people who have received organ transplants. Up to 30% of people treated with this drug develop sebaceous hyperplasia. Cyclosporine is a fat-loving (lipophilic) medication, so it tends to build up where there is oil, such as in the skin oil glands. Once there, cyclosporine stimulates undeveloped sebocytes to overgrow, resulting in the enlargement of skin oil glands.6
Treatments for Sebaceous Hyperplasia
Sebaceous hyperplasia is a persistent skin condition, which means it will not go away on its own without treatment. First, it is important to see a dermatologist to make sure you really have sebaceous hyperplasia and not another condition that may look similar, like some forms of skin cancer.
There are many treatment options for sebaceous hyperplasia, and most need to be performed by a doctor. Some topical over-the-counter treatments like salicylic acid can help to reduce the appearance of the bumps, but to fully remove them, more in-depth treatment is usually necessary.
First-line treatments for sebaceous hyperplasia include:
- Laser therapy: The pinpoint laser beam breaks down the sebaceous gland, which then crusts over. After the scarring process completes, the sebaceous gland will be smaller. As a side effect, the treated glands may appear reddish-purple for several weeks after treatment.
- Cryotherapy: Liquid nitrogen is placed on top of the sebaceous gland to cause a freeze burn. After the scarring process completes, the sebaceous gland will be smaller. Cryotherapy is effective for 71.4% of males and 61.8% of females, but can cause side effects like a scar or skin lightening.
- Bichloroacetic or trichloroacetic (TCA) acid: The acid is applied to the bump to damage the sebaceous gland. After the scarring process completes, the sebaceous gland will be smaller. Side effects can include prolonged stinging, indented scars, and skin lightening.
- Surgical removal: The bump is removed by burning (cauterization) or cutting out with a scalpel (excision). This option is a last resort because it can cause scarring.1,5,7-9
Second-line treatments for sebaceous hyperplasia include:
- Photodynamic therapy with aminolevulinic acid (ALA) or methyl aminolevulinate (MAL): This light-based treatment targets the sebocytes to stop them from overgrowing. Several sessions are usually necessary to see results.
- Oral medication: A so-called 5-lipoxygenase inhibitor like Zileuton (Zyflo CR®) can directly decrease sebum production. A last resort option is oral isotretinoin (Accutane®), which can also reduce the size and activity of sebaceous glands. With both of these medications, sebaceous hyperplasia may return once you stop taking the drugs.1,5,7,8,10
How well any of these treatments work will depend on several factors, such as the number and severity of the sebaceous hyperplasia lesions, your skin type, and your age.11 Your doctor will help you choose a suitable option for your particular case and budget.
Sebaceous Hyperplasia Vs. Acne
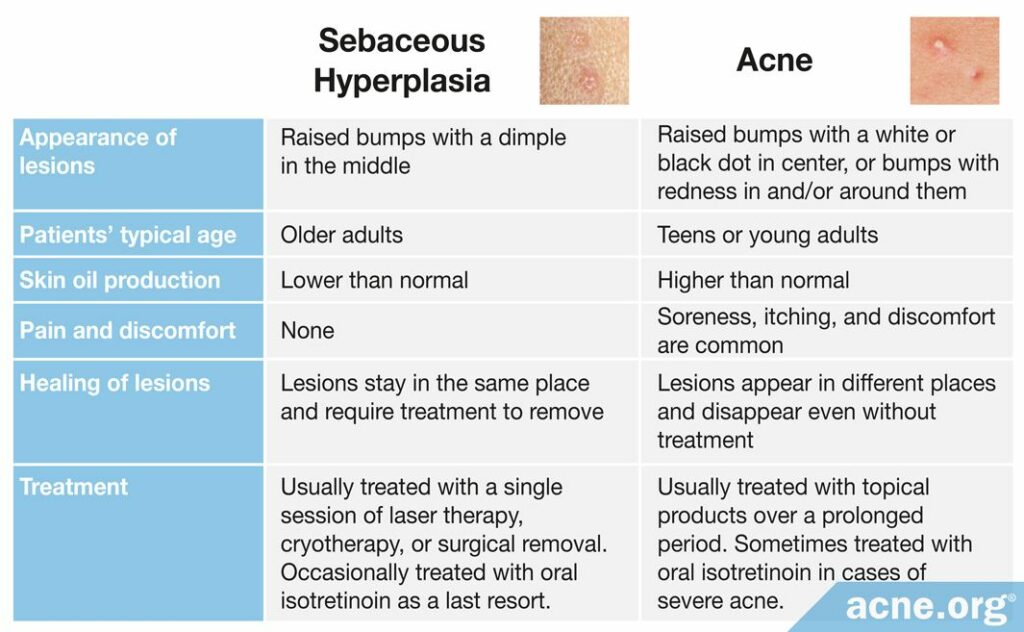
Both sebaceous hyperplasia and acne occur in the sebaceous glands on the face and upper body, but the two conditions are completely unrelated.12 They look different, occur at different ages and for different reasons, and require different treatments. The table below summarizes these differences.
The Bottom Line
Sebaceous hyperplasia is a harmless skin condition that bears a slight outward resemblance to acne, but has different causes and treatments. If you suspect you may have sebaceous hyperplasia, see a dermatologist to rule out other skin diseases that look similar. If you are diagnosed with sebaceous hyperplasia, your doctor can probably zap it with a laser, freeze it, cauterize it, or put some acid on it and help reduce it.
References
- Aghassi, D., González, E., Anderson, R. R., Rajadhyaksha, M. & González, S. Elucidating the pulsed-dye laser treatment of sebaceous hyperplasia in vivo with real-time confocal scanning laser microscopy. J. Am. Acad. Dermatol. 43, 49 – 53 (2000). https://www.ncbi.nlm.nih.gov/pubmed/10863223
- Sato, T. & Tanaka, M. Linear sebaceous hyperplasia on the chest: Case presentations. Dermatology Pract. Concept. 4, 93 – 95 (2014). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3919849/
- Hou, X., Wei, Z., Zouboulis, C. C. & Ju, Q. Aging in the sebaceous gland. Front. Cell. Dev. Biol. 10, 909694 (2022). https://pubmed.ncbi.nlm.nih.gov/36060807/
- Pochi, P. E., Strauss, J. S. & Downing, D. T. Age-related changes in sebaceous gland activity. J. Invest. Dermatol. 73, 108 – 111 (1979). https://www.sciencedirect.com/science/article/pii/S0022202X15455538
- Tagliolatto, S., Enokihara, M. & Alchorne, M. M. a. Sebaceous hyperplasia : a pilot study to correlate this skin disease with circulating androgen levels. An. Bras. Dermatologiais Bras. 86, 917 – 923 (2011). https://www.ncbi.nlm.nih.gov/pubmed/22147031
- Wilken, R. et al. Cyclosporine-induced sebaceous hyperplasia in a hematopoetic stem cell transplant patient: Delayed onset of a common adverse event. Dermatol. Online J. 22, 0 – 5 (2016). https://www.ncbi.nlm.nih.gov/pubmed/26990469
- Atas, H. & Gönül, M. Evaluation of the efficacy of cryosurgery in patients with sebaceous hyperplasia of the face. J. Cutan. Med. Surg. 21, 202 – 206 (2017). https://www.ncbi.nlm.nih.gov/pubmed/28300439
- Tagliolatto, S., Santos Neto, O. de O., Alchorne, M. M. de A. & Enokihara, M. Y. Sebaceous hyperplasia: Systemic treatment with isotretinoin. An. Bras. Dermatol. 90, 211 – 215 (2015). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4371670/
- Rosian, R., Goslen, J. B. & Brodell, R. T. The treatment of benign sebaceous hyperplasia with the topical application of bichloracetic acid. J. Dermatol. Surg. Oncol. 17, 876 – 879 (1991). https://www.ncbi.nlm.nih.gov/pubmed/1757649
- Wang, S., Chang, Y., Chi, C., Wang, S. & Tsai, T. Using pulsed dye laser to treat sebaceous hyperplasia: comparison of short and long pulse-duration pulsed dye laser. Dermatologica Sinica 35, 119-123 (2017). https://www.sciencedirect.com/science/article/pii/S1027811716300805
- Hussein, L. & Perrett, C. M. Treatment of sebaceous gland hyperplasia: a review of the literature. J. Dermatolog. Treat. 32, 866-877 (2021). https://pubmed.ncbi.nlm.nih.gov/32011918/
- Zouboulis, C. C. & Boschnakow, A. Chronological ageing and photoageing of the human sebaceous gland. Clin. Exp. Dermatol. 26, 600‐607 (2001). https://pubmed.ncbi.nlm.nih.gov/11696064/
 Acne.org Products
Acne.org Products