In Both Males and Females, Estrogens Improve Acne by Decreasing the Production of Skin Oil

The Essential Info
Both males and females produce female hormones called estrogens. Estrogens counteract the effects of male hormones in the body, thereby decreasing the production of skin oil and reducing acne.
To put it simply, male hormones tend to make acne worse, and female hormones tend to improve acne.
Birth control pills containing estrogens can be used to treat acne in females and produce on average a 60% reduction in acne after 6 months, but come with side effects.

The Science
- Role of Estrogens in the Body
- Types of Estrogens
- Estrogens Improve Acne
- The Science: How Estrogens Decrease Acne
- Estrogen Therapy for Females with Polycystic Ovarian Syndrome (PCOS)
- The Bottom Line
Estrogens are female sex hormones. Although they are female hormones, they are also produced in males in smaller amounts. There is actually no single hormone called “estrogen.” Instead, estrogens are a class of closely related hormones with similar names.
Role of Estrogens in the Body
In females, estrogens are responsible for:
- The development and activity of the female sex organs
- The development of secondary sex characteristics like the growth of breasts and widening of the hips
- Regulating menstrual cycles
In both males and females, estrogens:
- Increase bone density
- Help with blood clotting
- Increase fat stores
Expand to learn about where estrogens are produced in the body
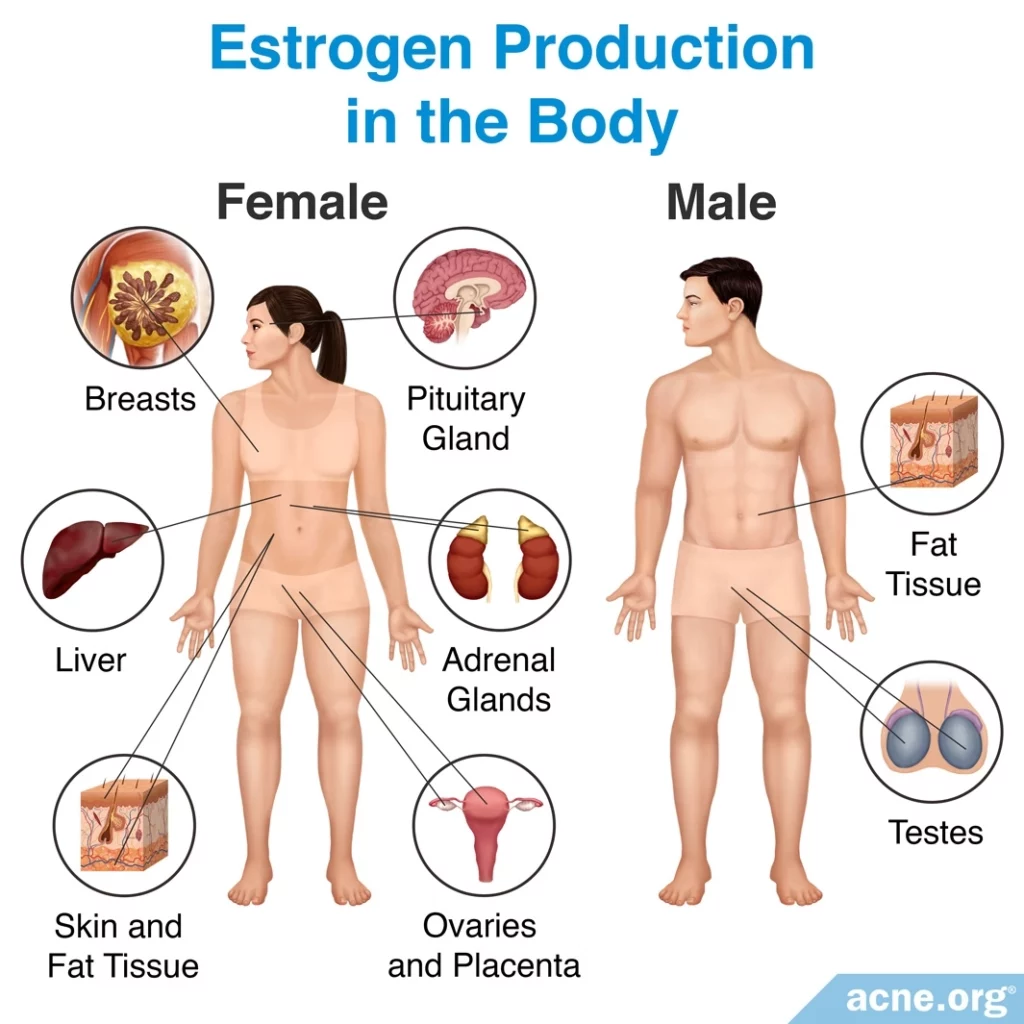
Where in the Body Are Estrogens Produced?
In females, estrogens are produced in the:
- Ovaries
- Placenta during pregnancy*
- Adrenal glands
- Liver
- Breasts
- Skin
- Fat tissue
*Most of a woman’s estrogens are produced in the ovaries – or in the placenta when she is pregnant – with much smaller amounts being produced by the other five organs.
In males, estrogens are produced in the:
- Testes
- Fat tissue
The production of estrogens is controlled by the pituitary gland, which is located at the base of the brain. The pituitary gland is the master hormonal gland of the human body, which means that it acts like a central computer – controlling other organs in the body. The pituitary gland does this by producing hormones that then stimulate the production of other hormones by different organs.1
To stimulate the production of estrogens, the pituitary gland sends out two hormonal signals: follicle-stimulating hormone (FSH) and luteinizing hormone (LH). FSH and LH work as follows:
- In females, FSH and LH stimulate the ovaries to produce large amounts of estrogens** and small amounts of androgens (male hormones like testosterone)
- In males, FSH and LH stimulate the testes to produce large amounts of androgens and small amounts of estrogens**1
**Estrogens are actually produced from androgens, which means while females ultimately hold small amounts of androgens, the ovaries make a large amount of androgens at first and then convert most of it into estrogens.2
Types of Estrogens
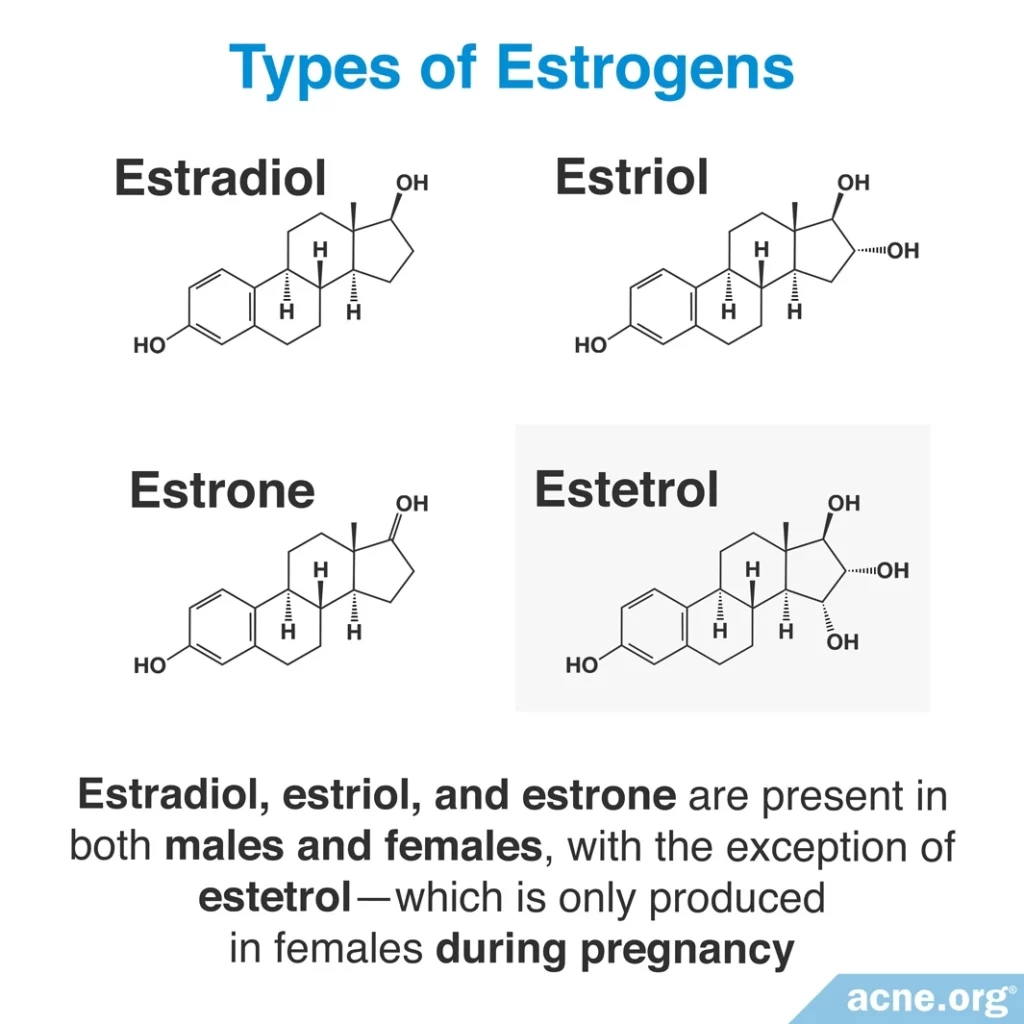
The four main estrogens include:
- Estradiol (the primary estrogen)
- Estriol
- Estrone
- Estetrol (produced only in women during pregnancy)
These estrogens are present in both males and females, with the exception of estetrol.
Scientists do not fully understand how the body controls the balance between androgens and estrogens. However, this balance is critical for overall health as well as specifically for skin health.3
Estrogens Improve Acne
Researchers and doctors have long recognized that estrogens appear to improve acne. For example, in females, acne tends to occur when the levels of estrogens in the blood are low.

An overview article on the role of hormones in acne, published in 2011 in the journal Clinical Biochemistry, noted that in many cases, females with acne possess low estrogen levels:
- Acne in females often occurs at puberty, when menstrual cycles are just beginning to be established and estrogen levels are low
- Acne in females may worsen just before the beginning of a menstrual cycle, when estrogen levels drop
- Females with acne tend to have less estrogen in their blood than females without acne4
Two recent studies provide more evidence that people with acne—both males and females—tend to have low levels of estrogens, specifically estradiol. The first study looked at 89 females with acne and found that 73% of them had low levels of estradiol in the blood.5 The second study looked at 693 males and females with acne and found that 37.2% of them, or just over a third, had levels of estradiol below the normal range.6
Estrogenic Medications (Birth Control Pills) Tend to Decrease Acne
Since high estrogen levels tend to decrease acne, medications that contain estrogen can be used as an acne treatment. Estrogen therapy usually comes in the form of oral contraceptives (birth control pills), which reduce acne on average by 60% after 6 months.
For males, estrogen therapy is not an option because of unwanted side effects, such as gynecomastia (enlarged breasts) and sexual dysfunction.
Today, most oral contraceptives are combined oral contraceptives (COCs), meaning that they combine two components:
- A synthetic version of estrogen
- A synthetic version of progesterone, which is another type of female hormone

One large study published in 2012 combined and analyzed the results of many earlier studies with a total of over 12,000 participants. The researchers concluded that the findings of all the studies agree that oral contraceptives can reduce acne and that all the combined oral contraceptives were effective in reducing acne, regardless of the particular synthetic estrogen each contained.7
Expand to read details of study

A large study was published in 2012 in the Cochrane Database of Systematic Reviews. The authors performed a meta-analysis, which means that they combined the results from many different clinical studies and analyzed them in order to draw some general conclusions. For this meta-analysis, the scientists examined 31 separate studies on oral contraceptives and acne, with a total of 12,579 participants. The researchers found that in the studies which compared a combined oral contraceptive to a placebo (in this case, an identical-looking pill without any hormones), the oral contraceptive significantly reduced acne. They wrote, “All [studies] showed [combined oral contraceptives] reduced acne lesion counts, severity grades and self-assessed acne compared to placebo.”7
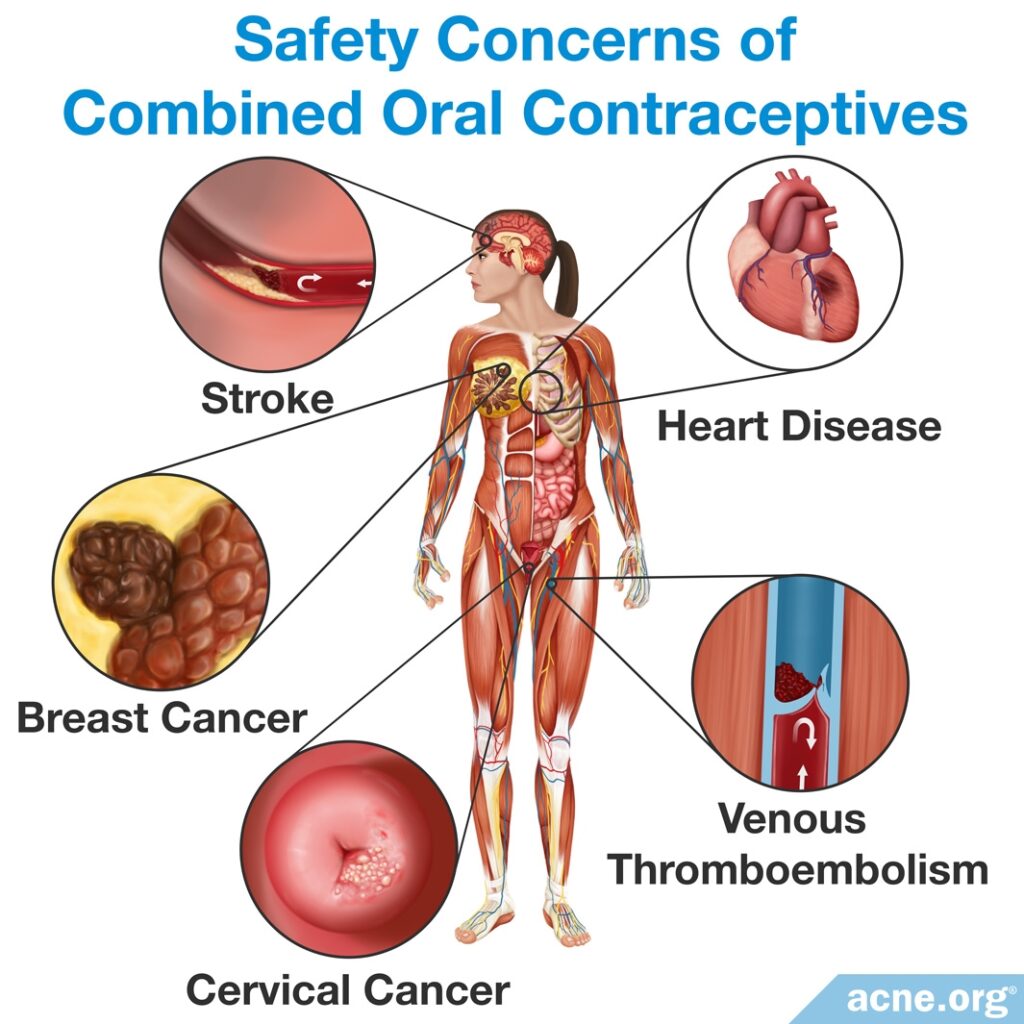
Side effects: However, it is important to keep in mind that oral contraceptives cause moderate to potentially serious side effects, such as increased risk of blood clots, stroke, and heart attack, especially in women over 30 years old who smoke. Some people may also be at increased risk of developing venous thromboembolism (a blood clot in a vein). It is a good idea to speak with your doctor about any family history of blood clots before beginning hormonal therapy for acne. Because of the potential side effects, oral contraceptives are usually only prescribed for acne when other treatments, like benzoyl peroxide and/or retinoids, fail.
How long before they work: Acne begins to improve after about 3 months of taking combined oral contraceptives, while the biggest improvement occurs after 6 months of taking the pills.8
The Science: How Estrogens Decrease Acne

Estrogens improve acne in both males and females by counteracting the effects of androgens, which tend to worsen acne.9
To understand how estrogens relieve acne, we first need to understand the effects of androgens on acne. Androgens, such as testosterone, signal skin oil-producing glands, called sebaceous glands, to produce more skin oil, called sebum. Androgens from the blood do this by binding to the cells of the sebaceous glands, called sebocytes. Inside these cells, the androgens then head for the nucleus, which is the so-called “control center” of each cell. The nucleus contains the cell’s genetic material, which is the biological instructions telling the cell what to do and how to grow. When androgens penetrate the nucleus of a sebocyte, they “turn on” specific genes that “tell” the cell to start synthesizing more sebum. In other words, increased androgen levels in the blood results in more androgens interacting with sebaceous glands, causing an increase in sebum.10
On the other hand, estrogens have the opposite effect, meaning that they decrease sebum production in both males and females.
Scientists speculate that estrogens achieve a decrease in sebum by one of three mechanisms.
- Estrogens may stop the production of androgens in the body via a so-called “negative feedback loop.” As we have seen, in both males and females, the sex organs begin producing both androgens and estrogens when the pituitary gland sends a signal to the sex organs. The pituitary gland constantly monitors the amount of sex hormone in the blood to see if there is already an abundance of estrogen or androgen in the body. If it senses much estrogen in the blood, it stops sending a signal to the sex organs, which stop producing androgens that the body can convert into more estrogens. In other words, having a lot of estrogen in your blood can temporarily stop your body from making more androgens. Less androgen production entails less sebum production, which potentially means less acne.
- Estrogens may decrease the amount of so-called “free” testosterone in the blood. Free testosterone is testosterone which floats around in the blood by itself and can bind to sebaceous glands to stimulate sebum production. Most testosterone in the body is not free but is bound to proteins. Estrogens may cause the liver to synthesize more of these proteins, so that more testosterone is bound and less is free.
- Estrogens may also indirectly help with acne by entering the cells of the sebaceous glands and “turning on” genes that tell the cells to produce less, not more, sebum.11
Besides reducing the amount of sebum, estrogens also reduce inflammation – in other words, they reduce the redness, swelling, and soreness that come with acne breakouts.4 Thus, estrogen not only helps to prevent the first step in acne development, but helps to relieve the symptoms of acne as well.
Because of the multiple ways estrogens can work against acne, combined oral contraceptives that contain estrogen can be a good choice for long-term treatment in some women with acne. For best results, doctors should prescribe estrogen therapy together with topical treatments that attack acne on other fronts. Such topical treatments can include benzoyl peroxide, topical retinoids (tretinoin, adapalene, tazarotene, trifarotene), and/or azelaic acid.12
Estrogen Therapy for Females with Polycystic Ovarian Syndrome (PCOS)
Some females have an excess of androgens due to a hormonal condition called polycystic ovary syndrome (PCOS), characterized by acne, excessive hair growth, and menstrual irregularities. For females who suffer from acne due to PCOS, research shows that estrogen therapy can be a good treatment option.13-17 If you are a female who experiences these symptoms, be sure to see a doctor for a proper diagnosis.
The Bottom Line
Estrogens can improve acne by reducing the production of sebum and relieving the symptoms of breakouts. Oral contraceptives containing estrogen have been shown to be effective in treating acne in females, but they come with potentially serious risks. Estrogen therapy for acne is not available for males because of undesirable side effects.
References
- Silverthorn, D. Human Physiology: An Integrated Approach (Pearson, 2010).
- Thiboutot, D. Regulation of Human Sebaceous Glands. J. Invest. Dermatol. 123, 1 – 12 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15191536
- Estradiol. https://en.wikipedia.org/wiki/Estradiol
- Arora, M. K., Yadav, A. & Saini, V. Role of hormones in acne vulgaris. Clin. Biochem. 44, 1035 – 1040 (2011). https://www.ncbi.nlm.nih.gov/pubmed/21763298
- Gayen, R., Podder, I., Chakraborty, I. & Chowdhury, S. N. Sex hormones, metabolic status, and obesity in female patients with acne vulgaris along with clinical correlation: An observational cross-sectional study. Indian J. Dermatol. 66, 60-66 (2021). https://pubmed.ncbi.nlm.nih.gov/33911295/
- Zhang, R., Zhou, L., Lv, M., Yue, N., Fei, W., Wang, L., Liu, Z. & Zhang, J. The relevant of sex hormone levels and acne grades in patients with acne vulgaris: A cross-sectional study in Beijing. Clin. Cosmet. Investig. Dermatol. 15, 2211-2219 (2022). https://pubmed.ncbi.nlm.nih.gov/36281268/
- Arowojolu, A. O., Gallo, M. F., Lopez, L. M. & Grimes, D. A. Combined oral contraceptive pills for treatment of acne. Cochrane Database Syst. Rev. 7 – 9 (2012). https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD004425.pub6/full
- Trivedi, M. K., Shinkai, K. & Murase, J. E. A Review of hormone-based therapies to treat adult acne vulgaris in women. Int. J. Womens Dermatol. 3, 44 – 52 (2017). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5419026/
- Toyoda, M. & Morohashi, M. Pathogenesis of acne. Med. Electron. Microsc. 34, 29 – 40 (2001). https://www.ncbi.nlm.nih.gov/pubmed/11479771
- Degitz, K., Placzek, M., Borelli, C. & Plewig, G. Pathophysiology of acne. J. Dtsch Dermatol. Ges. 5, 316 – 323 (2007). https://www.ncbi.nlm.nih.gov/pubmed/17376098
- Tan, A. U., Schlosser, B. J. & Paller, A. S. A review of diagnosis and treatment of acne in adult female patients. Int. J. Womens Dermatol. 4, 56 – 71 (2017). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5986265/
- Thiboutot, D. Acne: Hormonal Concepts and Therapy. Clin. Dermatol. 22, 419 – 428 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15556729
- Thiboutot, D. & Chen, W. C. Update and Future of Hormonal Therapy in Acne. Dermatology 206, 57 – 67. (2003). https://www.ncbi.nlm.nih.gov/pubmed/12566806
- Couzinet, B., Le Strat, N., Brailly, S. & Schaison, G. Comparative effects of cyproterone acetate or a long-lasting gonadotrophin-releasing hormone agonist in polycystic ovarian disease. J. Clin. Endocrinol. Metab. 63, 1031 – 1035 (1986). https://www.ncbi.nlm.nih.gov/pubmed/2943752
- Conway, G. et al. The polycystic ovary syndrome: a position statement from the European Society of Endocrinology. Eur. J. Endocrinol. 171, P1 – 19 (2014). https://www.ncbi.nlm.nih.gov/pubmed/24849517
- McCartney, C. R. & Marshall, J. C. Polycystic ovary syndrome. N. Engl. J. Med. 375, 54 – 64 (2016). https://www.ncbi.nlm.nih.gov/pubmed/27705264
- Spritzer, P. M. & Motta, A. B. Adolescence and polycystic ovary syndrome: current concepts on diagnosis and treatment. Int. J. Clin. Pract. 69, 1236 – 1246 (2015). https://www.ncbi.nlm.nih.gov/pubmed/26289303
 Acne.org Products
Acne.org Products