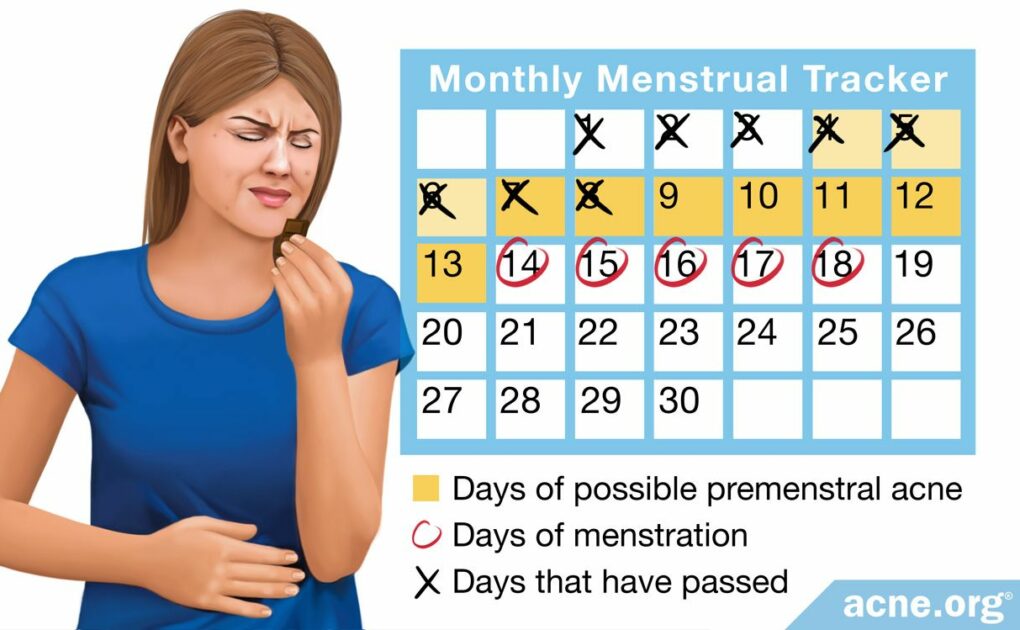
Acne Sometimes Flares Approximately 7-10 Days Prior to Menstruation

The Essential Info
Hormone levels fluctuate during the menstrual cycle and can result in acne flares, particularly 7-10 days or so before the onset of menstruation.
Premenstrual acne is very common, with studies showing that among women who suffer from acne, 36-78% experience premenstrual acne flares.
Pimples from premenstrual flares tend to be inflammatory, which means they are red and sore.
The most common treatments include:
- Topical Treatment – Proper topical treatment can normally keep premenstrual flares at bay.
- Birth Control Pills – Combined oral contraceptives (COCs), commonly referred to as birth control pills, regulate hormones and can get to the “root cause” of premenstrual acne in women. However, COCs come with side effects, and should only be entered into carefully, alongside a trusted physician.

The Science
The menstrual cycle influences acne. Many women experience an acne flare approximately 7-10 days before their period, and then see improvement in their acne once menstruation starts. These cyclical acne flares result from the fluctuation of hormones during the menstrual cycle.
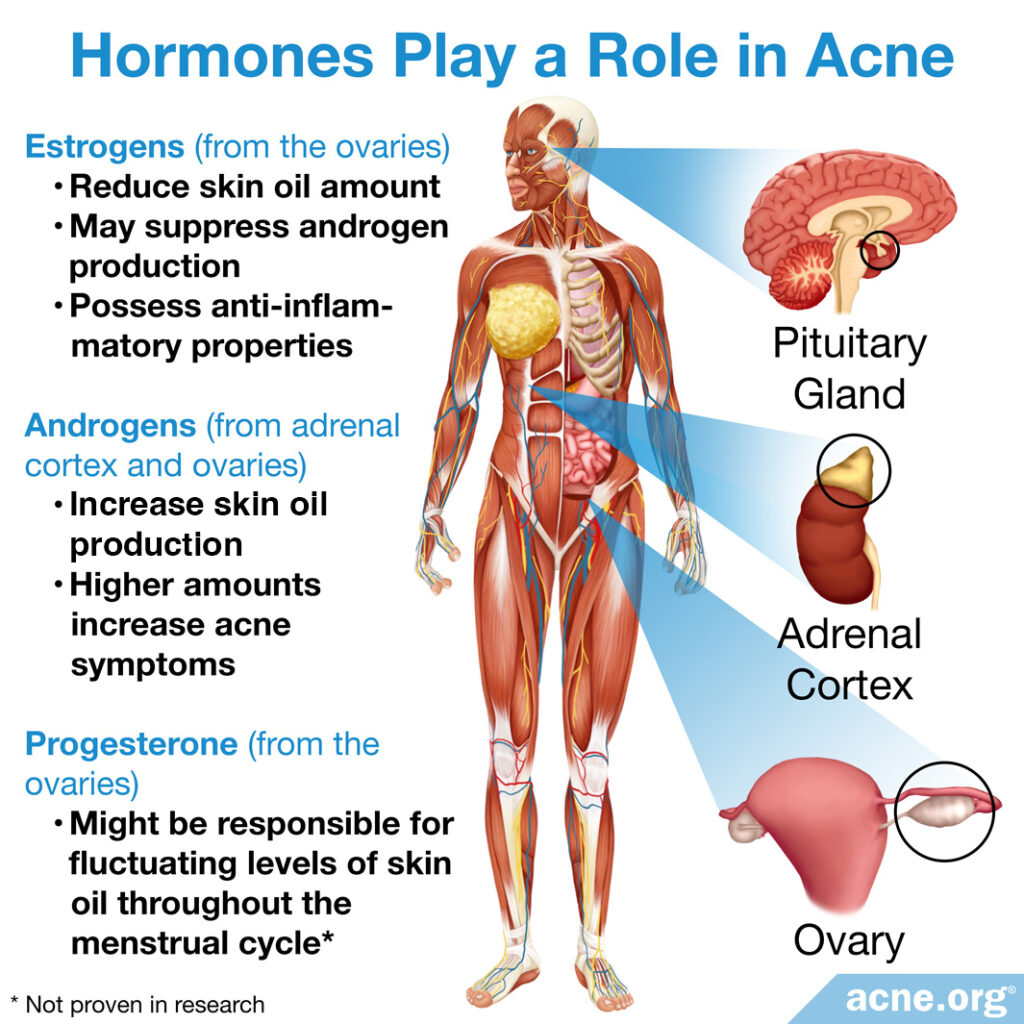
First let’s look at the hormones that fluctuate over a woman’s monthly cycle. Each of these hormones plays a different role in acne:
- Estrogens: As a whole, estrogens reduce acne. They can do so in the following ways:
- They lower the amount of skin oil that the body produces. Less skin oil usually means less acne.
- They lower the production of androgens (male hormones present in both males and females), which also typically results in less acne.
- Estrogens possess anti-inflammatory properties. Since acne is an inflammatory disease, this means estrogens can reduce acne in this way as well.
- Androgens: As a whole, androgens increase acne. They do so in the following way:
- Higher levels of androgens increase skin oil production, which usually leads to more acne.
- Progesterone: Scientists are still not certain how progesterone might affect acne. It might be responsible for fluctuating levels of skin oil throughout the menstrual cycle. However, this has not been proven in the research.1,2
The Science: Why Does Acne Spike in the Premenstrual Window?
The primary reason why acne may occur in the premenstrual window is due to fluctuating hormones.
A 2011 systematic review published in Clinical Biochemistry looked at many studies in order to examine the role that hormones play in acne. The authors of the review found that acne was correlated with low levels of estrogen and high levels of progesterone in the blood. They speculated that low estrogen levels might indirectly lead to increased skin oil (sebum) production and increased inflammation, and thus to acne.2
Expand to read details of review

When acne was present, blood levels of estrogen were low, and blood levels of progesterone were high. The review did not specifically look at menstrual cycles, however, they do tell us about the relationship between changing hormones and acne. The authors noted that:
- Since estrogens reduce skin oil production and probably reduce androgen levels, low estrogen levels in the blood most likely contributed to acne.
- Since estrogens may provide an anti-inflammatory effect, and acne is primarily an inflammatory disease, lower levels of estrogen might contribute to acne inflammation.
- It is unclear what effects, if any, progesterone had on acne.2
Emerging research suggests that rising progesterone levels in the days leading up to menstruation may play their own part in premenstrual acne. Confusingly, progesterone seems to have somewhat contradictory effects on skin oil production:
- Progesterone may increase skin oil production: An increase in progesterone may lead to a rise in testosterone levels in the body. We know that more testosterone means more skin oil production and, in turn, more acne.
- Progesterone might decrease skin oil production: There is also evidence that progesterone might slightly reduce the ability of testosterone to trigger skin oil production.3
So which is it then? At the moment, scientists speculate that the first effect of progesterone may cancel out the second, resulting in a net increase in skin oil production. Therefore, this might explain why rising progesterone levels in the days leading up to menstruation contribute to acne flares.3 However, this is a field of ongoing research, so stay tuned.
Another reason why acne occurs in the premenstrual window may be due to skin pores contracting at this time, which in turn allows them to become more easily clogged, trapping skin oil (sebum) inside, and leading to acne.
A small study conducted in 1973 found that skin pores in women with acne were smallest during the premenstrual period, coinciding with an increase in acne at this time.4
Expand to read details of study

A small 1973 study in The Lancet measured the diameter of skin pores in 23 women who had mild-to-moderate acne and found that pore openings were smallest between the 15th and 20th days of the menstrual cycle. Smaller pores allow for skin oil to get stuck in the skin oil gland and clog the pores. Clogged pores can lead to acne. The authors also interviewed the women and found that their acne was worst on the 22nd day of the menstrual cycle, just a few days after pore openings got smaller. The authors concluded, “Obstruction of the [pore] is almost certainly one of the earliest changes needed for the development of an individual acne lesion.”4
The Evidence: Women Experience More Acne During the Premenstrual Window
What is clear is that acne does in fact flare in the premenstrual window, and this is backed up by multiple studies. These studies agree that among women who suffer from acne, 36-78% experience premenstrual acne flares.5-9
Another recent study looked more closely at premenstrual acne and found that acne flare-ups during this period tend to mean an increase in papules–red and inflamed acne lesions.10
Expand to read details of studies

A 2001 study in the Journal of the European Academy of Dermatology and Venereology had 3394 French women complete a questionnaire about their acne. This study found that 78% of the women reported having premenstrual acne flares.5

Another 2001 study in the Journal of the American Academy of Dermatology interviewed 400 American women who had acne. This study found that 44% of the women experienced premenstrual acne flares.6

A 2004 study published in Archives of Dermatology counted acne lesions during two menstrual cycles in adult women. This study found that in 63% of the women, inflammatory acne lesions increased by 25% during the premenstrual phase. The authors concluded, “[W]e believe that our observational data complement and confirm the results obtained by questionnaire that a significant number of adult women have a premenstrual flare of acne.”7

A 2009 study of 503 female high school students published in the Journal of Investigative Dermatology found that acne was more severe during the premenstrual period. They concluded, “The premenstrual phase in female high school pupils…[was] positively associated with the severity of…acne.”8

A 2014 study published in The Journal of Clinical and Aesthetic Dermatology surveyed 105 women between the ages of 18 and 49. The study included African-American, Latina, and Asian women. The researchers found that 65% of the women experienced worsening of their acne at a specific time during their menstrual cycle. More specifically, 36%, or slightly more than a third of the women, reported an increase in acne in the week before menstruation, while the rest reported that their acne worsened at various other points during their menstrual cycle. For example, 11% of the women experienced an increase in acne during menstruation itself.9

In a 2017 study published in the European Journal of Dermatology, researchers examined 32 women who suffered from premenstrual acne. They found that premenstrual acne flare-ups consisted of a significant increase in the number of papules and a smaller increase in the number of whiteheads. The researchers wrote, “Therefore, based on the results of our study, we propose a definition of premenstrual acne flare-up as an increase in the number of papules by at least 25% during the week prior to the menstrual period.”10

Finally, a study published in 2020 in the International Journal of Adolescent Medicine and Health reported that among 3065 young women between 18 and 25 years old, almost half had experienced acne at least once in the previous half-year. Among those women who had recently had acne, over half had experienced a flare-up around their period. In particular, 58.5% had had a flare-up one week before menstruation and 35% had had a flare-up during menstruation.11
So What Can Be Done About It?
Proper topical treatment of acne is normally strong enough to keep acne at bay during the premenstrual window, and comes with very few, manageable side effects. One study found that 57% of women with acne flare-ups around their period would be very likely to use a safe and effective topical treatment.9
Sometimes, doctors will prescribe birth control pills, also called combined oral contraceptives (COCs), when acne flares are especially severe, or when an oral contraceptive is desired or necessary for other reasons.
Combined oral contraceptives contain a combination of synthetic estrogen and synthetic progesterone. Research has shown that all COCs are effective in treating acne, so when it comes to premenstrual acne, there is no one proven birth control pill that is better than another.8,12
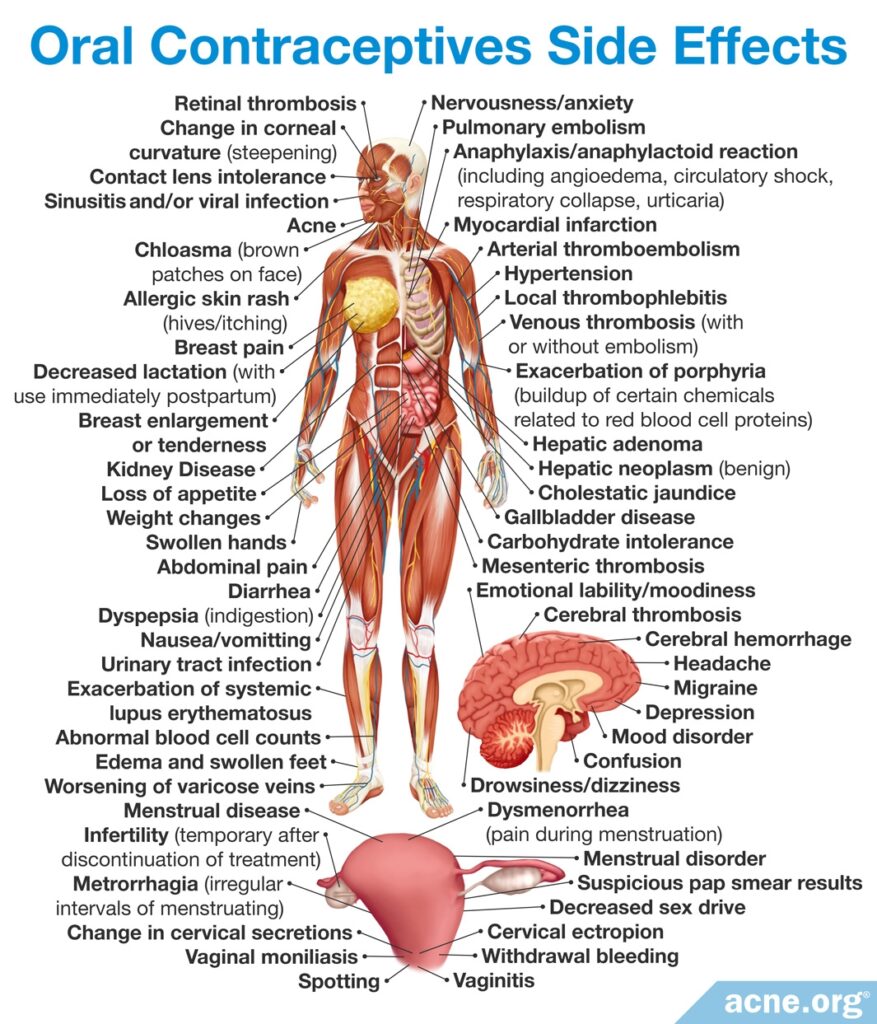
Oral contraceptives, while effective for reducing acne (on average by about 66%), come with a plethora of side effects, so be sure to have a serious conversation with your doctor before you embark upon this kind of hormonal therapy.
References
- Raghunath, R. S., Venables, Z. C. & Millington, G. W. The menstrual cycle and the skin. Clin. Exp. Dermatol. 40, 111 – 115 (2015). https://www.ncbi.nlm.nih.gov/pubmed/25683236
- Arora, M. K., Yadav, A. & Saini, V. Role of hormones in acne vulgaris. Clin. Biochem. 44, 1035 – 1040 (2011). https://www.ncbi.nlm.nih.gov/pubmed/21763298
- Zhang, R., Zhou, L., Lv, M., Yue, N., Fei, W., Wang, L., Liu, Z. & Zhang, J. The relevant of sex hormone levels and acne grades in patients with acne vulgaris: A cross-sectional study in Beijing. Clin. Cosmet. Investig. Dermatol. 15, 2211-2219 (2022). https://pubmed.ncbi.nlm.nih.gov/36281268/
- Williams, M. & Cunliffe, W. J. Explanation for premenstrual acne. The Lancet 2, 1055 – 1057 (1973). https://www.ncbi.nlm.nih.gov/pubmed/4127313
- Poli, F., Dreno, B. & Verschoore, M. An epidemiological study if acne in female adults: results of a survey conducted in France. J. Eur. Acad. Dermatol. Venereol. 15, 541 – 545 (2001). https://www.ncbi.nlm.nih.gov/pubmed/11843213
- Stoll, S. et al. The effect of the menstrual cycle on acne. J. Am. Acad. Dermatol. 45, 957 – 960 (2001). https://www.ncbi.nlm.nih.gov/pubmed/11712049
- Lucky, A. W. Quantitative documentation of a premenstrual flare of facial acne in adult women. Arch. Dermatol. 140, 423 – 424 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15096370
- Ghodsi, S. Z., Orawa, H. & Zouboulis, C. C. Prevalence, severity, and severity risk factors of acne in high school pupils: a community-based study. J. Invest. Dermatol. 129, 2136 – 2141 (2009). https://www.ncbi.nlm.nih.gov/pubmed/19282841
- Geller, L., Rosen, J., Frankel, A. & Goldenberg, G. Perimenstrual flare of adult acne. J. Clin. Aesthet. Dermatol. 7, 30 – 34 (2014). https://pubmed.ncbi.nlm.nih.gov/25161758/
- Saint-Jean, M., Khammari, A., Seite, S., Moyal, D. & Dreno, B. Characteristics of premenstrual acne flare-up and benefits of a dermocosmetic treatment: a double-blind randomised trial. Eur. J. Dermatol. 27, 144 – 149 (2017). https://pubmed.ncbi.nlm.nih.gov/28251894/
- Arafa, A., Mostafa, A. & Khamis, Y. The association of acne and menstrual symptoms among young women (18-25 years) in Egypt: a population-based cross-sectional study. Int. J. Adolesc. Med. Health. 11, 463-468 (2020). https://pubmed.ncbi.nlm.nih.gov/32549185/
- Schindler, A. E. Non-contraceptive benefits of oral hormonal contraceptives. Int. J. Endocrinol. Metab. 11, 41 – 47 (2013). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3693657/
 Acne.org Products
Acne.org Products