An Overview of Acne Development

The Essential Info
What It Is: If you’ve ever had a pimple, you’ve had acne. Symptoms can range widely, from an occasional pimple to severe, widespread acne that can scar.
Who It Affects: Acne affects almost every adolescent at some point, and also about 30% of adult women and 20% of adult men.
Where It Occurs: It occurs most commonly on the face, but over 1/2 of people who have facial acne also have acne on the body as well.
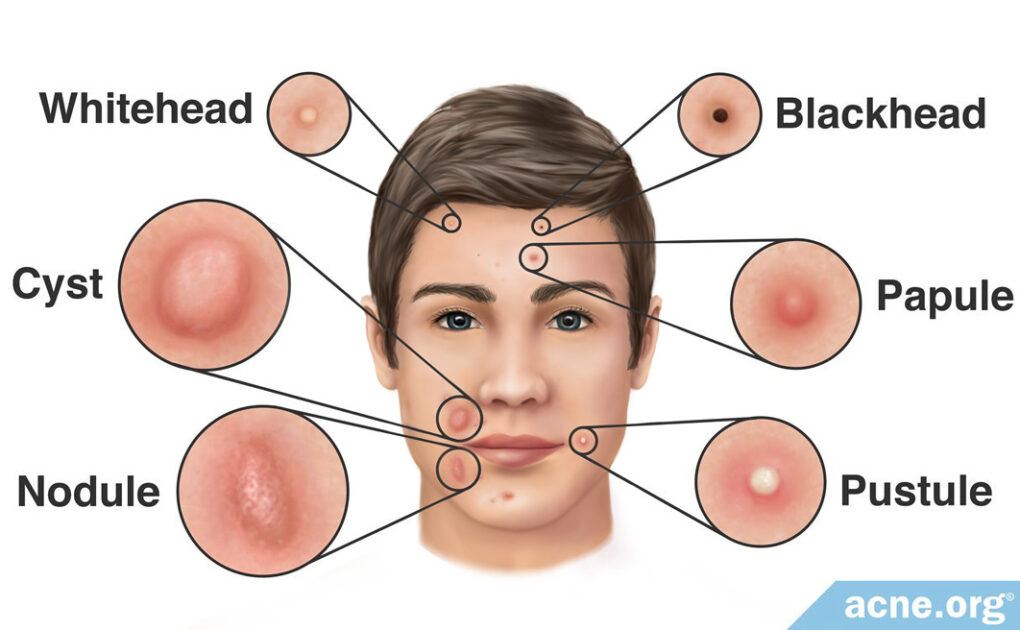
How It Develops: Acne lesions begin when inflammation, an increase in skin oil production, and an overgrowth of skin cells cause a skin pore to become clogged. The clogged pore traps skin oil inside the pore, where acne bacteria then feeds on the trapped skin oil and multiplies. Lesions fall into two categories:
- Non-inflammatory acne (not red or sore):
Whiteheads – small white dots on the skin
Blackheads – small black/brown dots on the skin
- Inflammatory acne (red and sore):
Papules – raised red pimples with no white or yellow center
Pustules – raised red pimples with a white or yellow center
Nodules – large (over 5mm wide), severe, painful, fibrous lesions not filled with pus
Cysts – large (over 5mm wide), severe, painful lesions filled with liquid or pus
This article is a basic explanation of what acne is and how it develops. For the full scientific scoop, including all current theories of exactly how it develops, see the What Is Acne – An In-Depth Look page.

The Science
Acne is a chronic inflammatory skin disease that starts after the onset of puberty when hormones increase. These hormones initiate to the production of skin oil, which is necessary for acne to form.
Acne can occur on any part of the body that has pores, which are tiny hair follicles. All parts of the body except the palms of the hands and soles of the feet have pores. However, we see acne mostly on the face and upper body (back, chest, back of the neck, shoulders) because these areas contain many pores, and the pores in these areas produce the most skin oil.
Acne lesions start when inflammation, increased skin oil production, and an overgrowth of skin cells causes pores to become clogged. This traps skin oil inside the pore where acne bacteria thrive and reproduce.
Inflammation plays a major and central role in acne development and is present from the very start of a clogged pore all the way until an acne lesion is completely healed. While all acne is inflammatory in nature, it is helpful to use the terms “non-inflammatory” to refer to acne that is not red and sore and “inflammatory” to refer to acne that is red and sore.
Non-inflammatory Acne
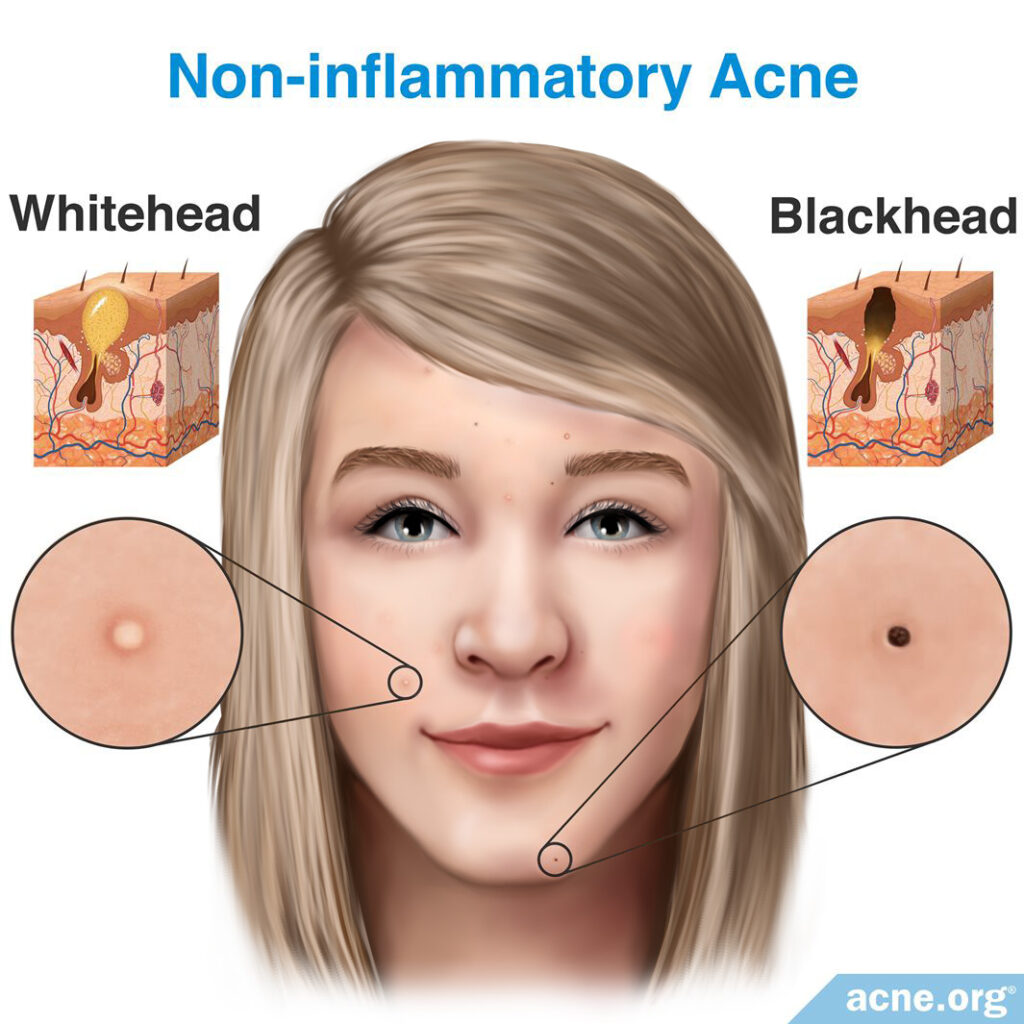
The very first phase of a clogged pore is called a microcomedone, which cannot be seen with the naked eye. Microcomedones form when an overproduction of skin cells narrows the opening of the pore and leads to a clog. Skin oil that normally drains to the surface gets trapped inside, and acne bacteria, which thrives in skin oil, reproduces rapidly.
The trapped skin oil and bacteria build up until they become visible to the naked eye, and the lesion is then called a comedone. There are two types of comedone:
- Whiteheads
- Blackheads
Whiteheads
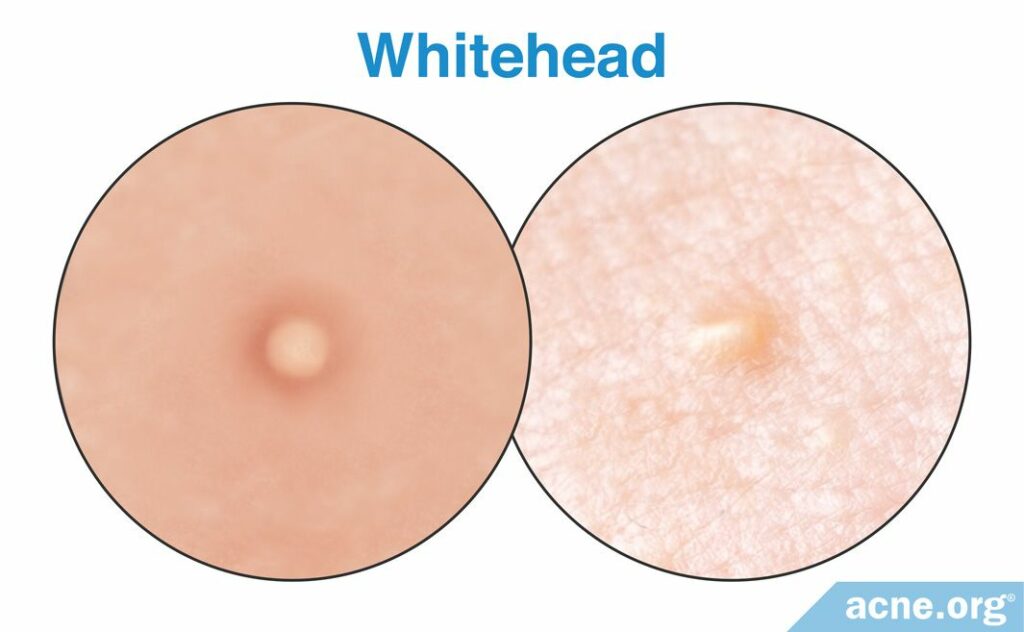
Whiteheads are lesions that appear as white spots on the surface of the skin. They also are called “closed comedones” because skin cells completely block the pore’s opening.
Blackheads
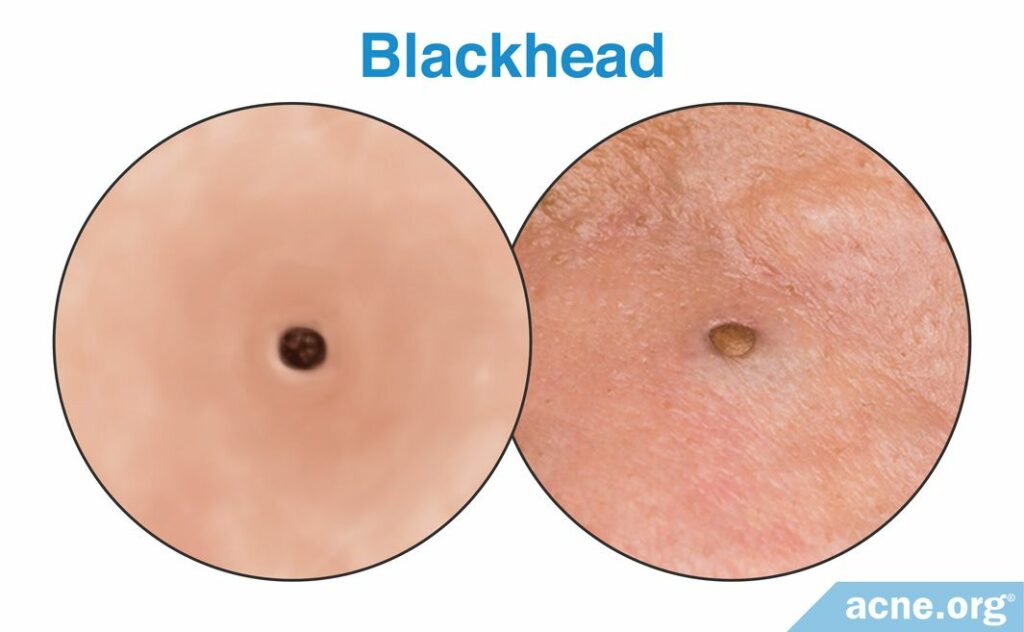
Blackheads are lesions that appear as brown or black spots on the skin’s surface. They are called “open comedones” because skin cells only partially block the opening of the pore. Because the pore is only partially clogged, skin oil and dead skin cells can seep out of the pore. When these contents reach the surface, the oxygen in the surrounding air chemically reacts with the skin pigment, called melanin, in the dead skin cells, and this gives a blackhead its characteristic black or brown color.
Whiteheads and blackheads can heal, or they can continue to grow and become inflammatory acne.
Inflammatory Acne
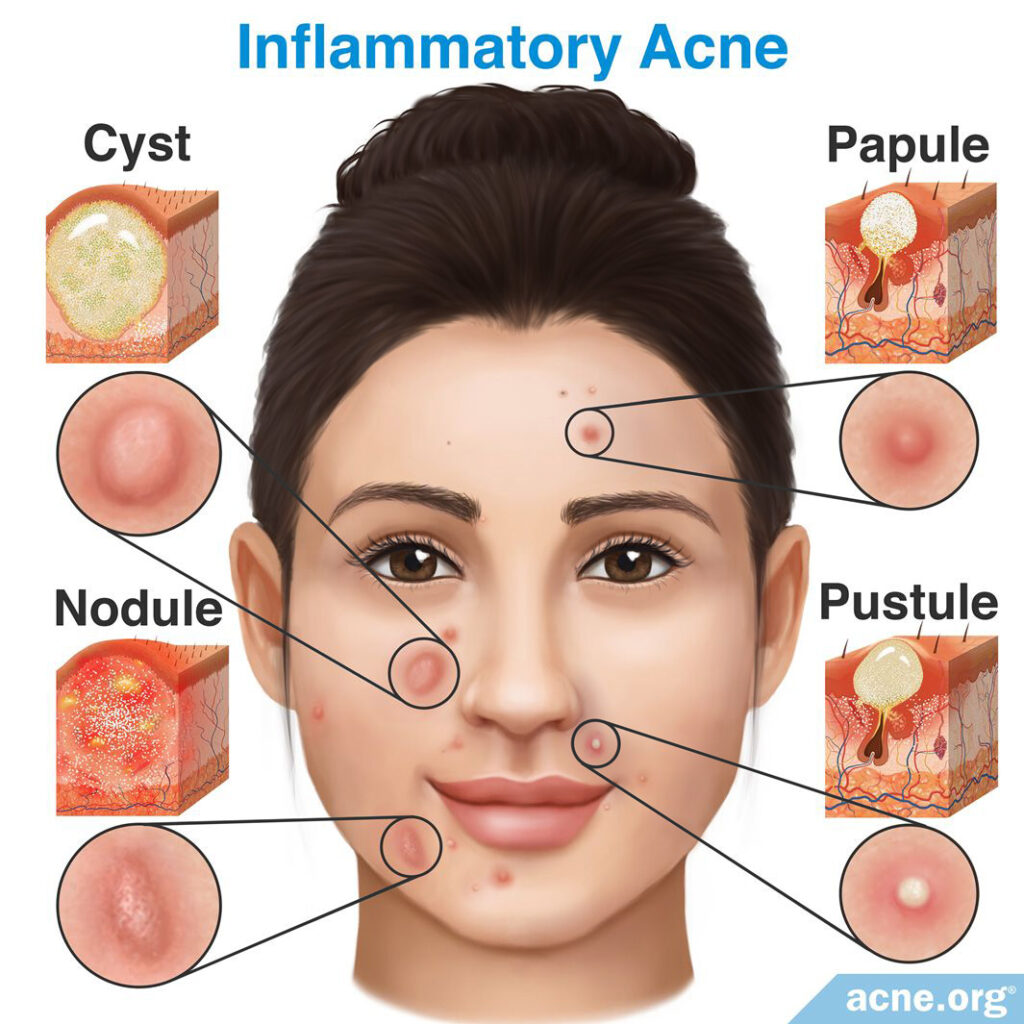
Inflammatory acne develops when so much pressure builds up inside a clogged pore that is breaks the wall of the pore, allowing the pore’s contents to leak into the surrounding skin.
The body’s immune system sees these contents as “foreign invaders” and activates inflammatory cells, most notably white blood cells, to fight the infection. The influx of inflammatory cells causes the acne lesion to become red and sore.
There are four types of inflammatory acne lesions:
- Papules
- Pustules
- Nodules (severe)
- Cysts (severe)
Papules
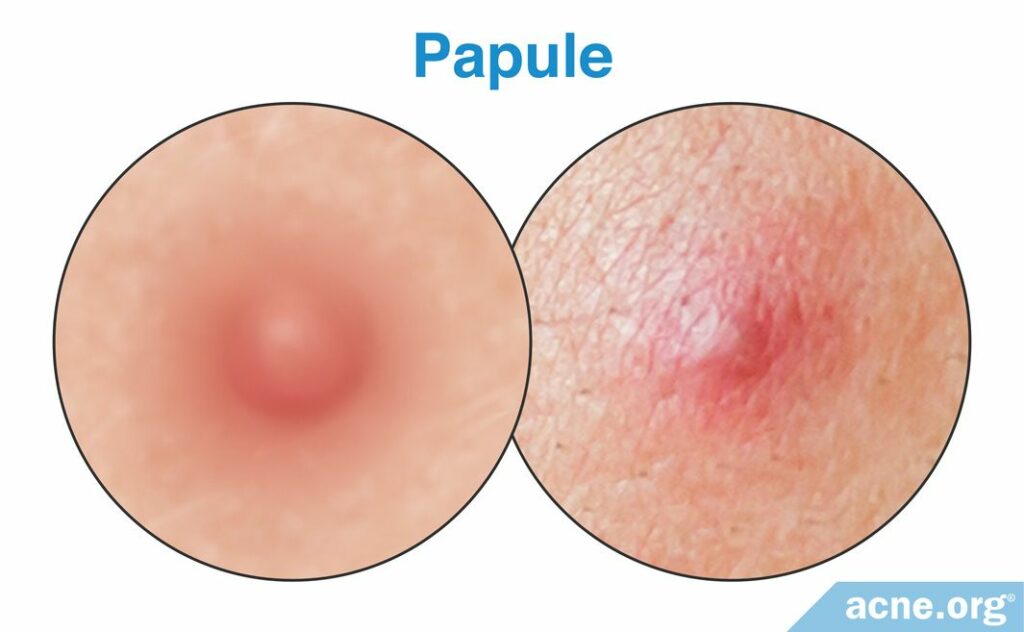
Papules are red lesions that contains no white or yellow center. They are the first lesion to develop after the wall of the clogged pore breaks.
Pustules
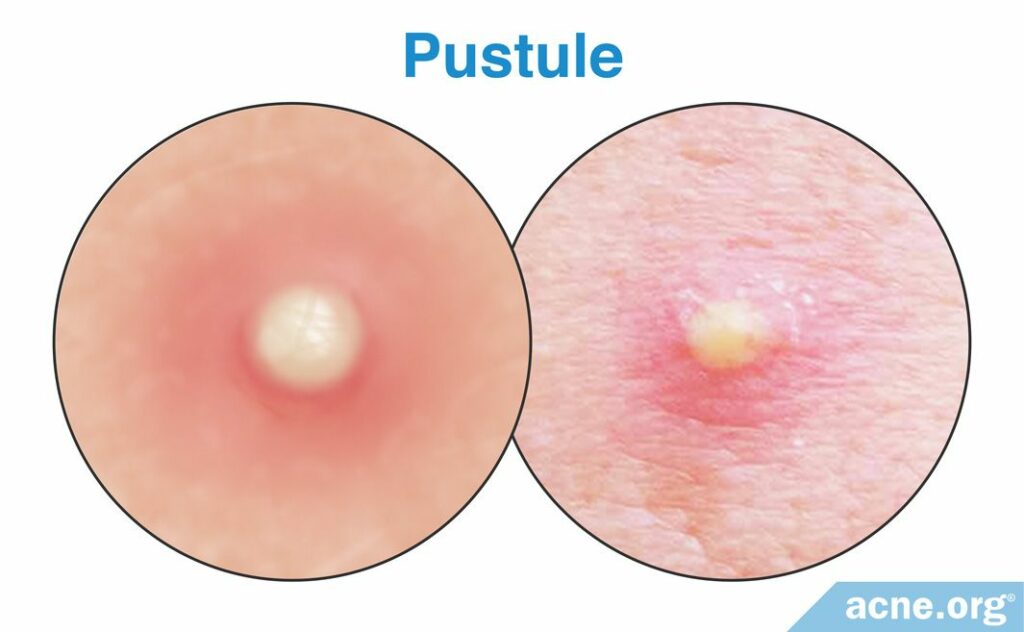
Pustules develop as a papule matures. They are red lesions with a white or yellow center, which is the result of the accumulation of white blood cells, called pus, inside the pore. Pustules are what many people refer to as “pimples” and “zits.”
Nodules (severe)
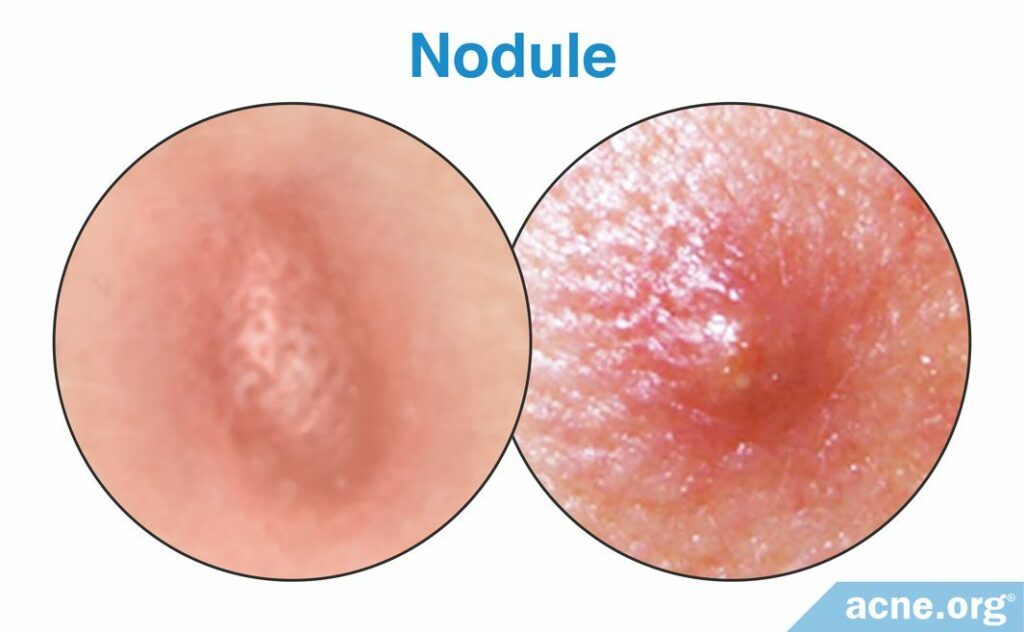
Nodules are by far the most common severe acne lesion. They are large (over 5mm in diameter) fibrous lesions that contains no white or yellow center, and are red, swollen, and usually painful. Nodules result when a clogged pore completely breaks down deep in the skin. This “explosion” results in a severe inflammatory response which frequently causes severe tissue damage that often leads to scarring.
Cysts (severe)
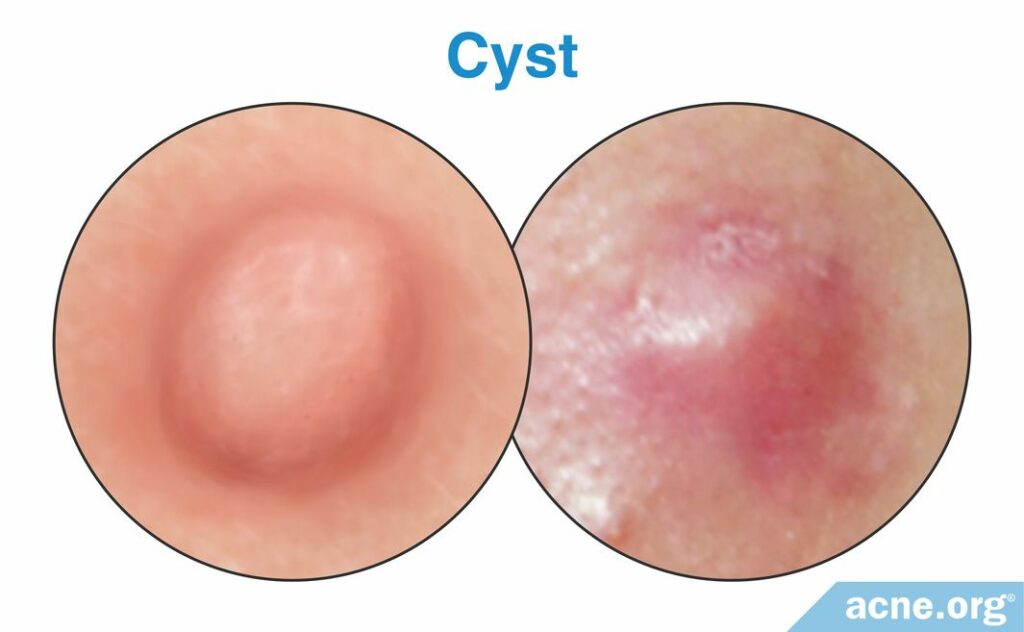
Cysts are less common severe acne lesions. They are also over 5mm in diameter, red, swollen, develop deep in the skin, and are often painful. However, unlike a nodule, cysts are not fibrous. Instead, they are filled with liquid or pus.
Eventually, the immune system heals an acne lesion by reducing inflammation and attempting to repair damage to the skin that the acne lesion may have caused. However, if the immune system creates excessive inflammation in an acne lesion, or if it does not heal the acne lesion quickly, scarring may occur.1-6
What Is Acne – An In-Depth Look <– Click for a deeper dive into the science of acne development.
References
- Tanghetti, E. The role of inflammation in the pathology of acne. J Clin Aesthet Dermatol 6, 27 – 35 (2013). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3780801/
- Degitz, K., Placzek, M., Borelli, C. & Plewig, G. Pathophysiology of acne. JDDG 5, 316 – 323 (2007). https://pubmed.ncbi.nlm.nih.gov/17376098
- Toyoda, M. & Morohashi, M. Pathogenesis of acne. Med Electron Microsc 34, 29 – 40 (2001). https://pubmed.ncbi.nlm.nih.gov/11479771
- Cunliffe, W. et al. Comedone formation: Etiology, clinical presentation, and treatment. Clin Dermatol 22, 367 – 374 (2004). https://pubmed.ncbi.nlm.nih.gov/15556720
- Brogden, R. & Goa, K. Adapalene. Drugs 53, 511 – 519 (1997). https://pubmed.ncbi.nlm.nih.gov/9074847
- Do, T. et al. Computer-assisted alignment and tracking of acne lesions indicate that most inflammatory lesions. arise from comedones and de novo. J Am Acad Dermatol 58, 603 – 608 (2008). https://pubmed.ncbi.nlm.nih.gov/18249468
 Acne.org Products
Acne.org Products