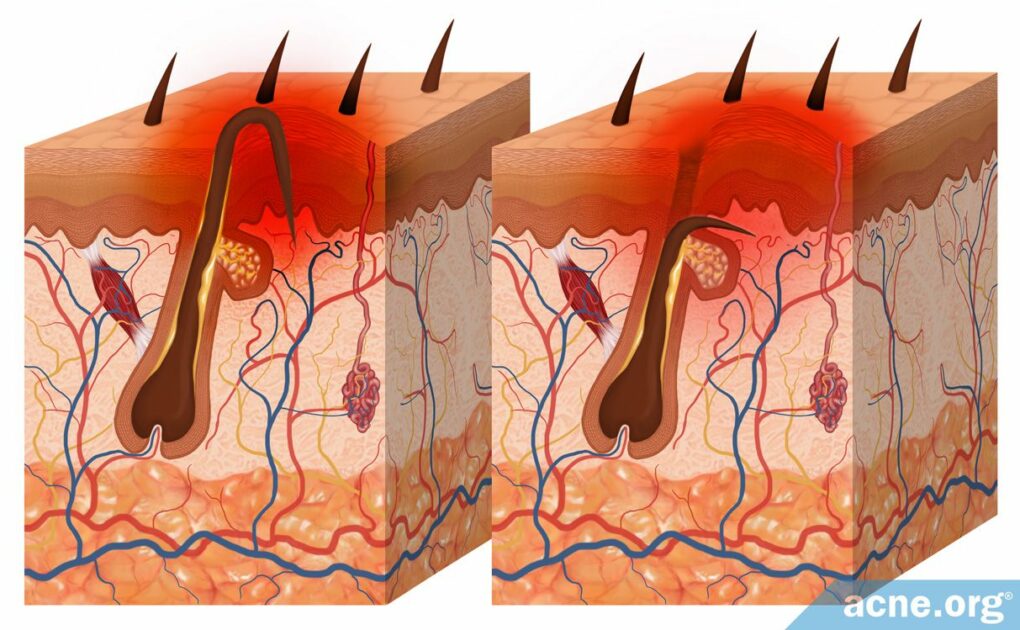
Ingrown Hairs Occur When Shaved or Removed Hairs Get Trapped Inside the Skin, Causing Acne-like Lesions

The Essential Info
Ingrown hairs, also often referred to as razor bumps, are a common skin condition caused by hair removal in both males and females, but are a particular problem on the neck in men.
They occur when shaved or removed hairs get trapped inside the skin, causing lesions that look like acne but are not actually acne.
Ingrown hairs are more common in people with curly hair, especially black men, and can be prevented by stopping or changing hair removal practices. They can also be treated topically.
My Take: I have never had a big problem with ingrown hairs, but have had a few friends who really suffered with them. A few things seem to work best:
- Not shaving at all and growing a beard.
- Using a beard trimmer instead of a razor to shave down to a “stubble” but not all the way to the skin.
- Shaving the way I recommend, with a 2-blade razor.
- Using The Regimen along with glycolic acid. Even though The Regimen is designed for acne, it has completely taken away razor bumps in several people who I know well.

The Science
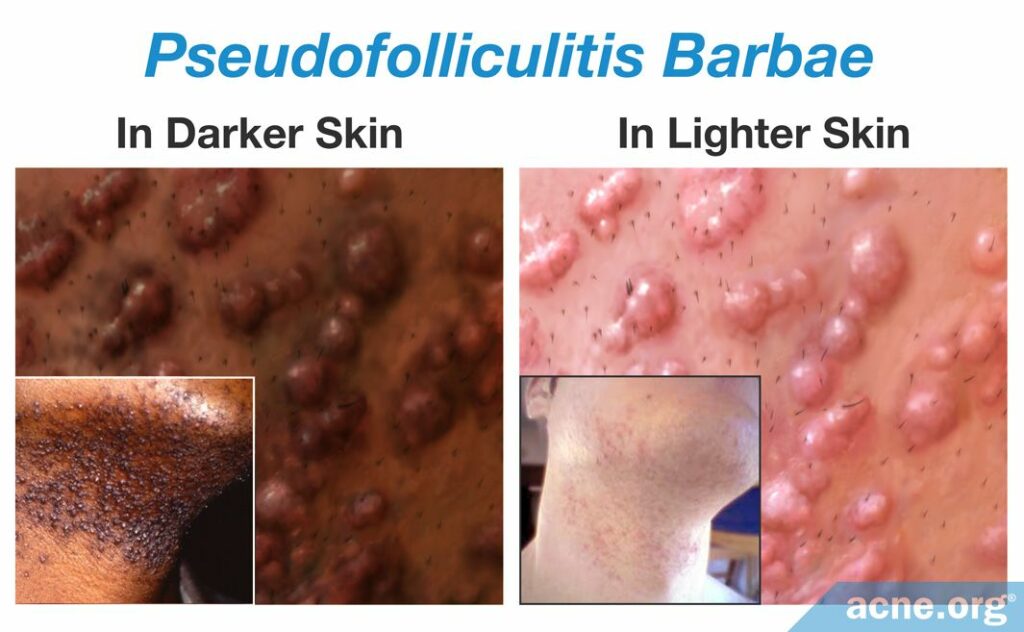
The medical term for “ingrown hairs” is pseudofolliculitis barbae.
Hair removal practices that can cause it include:
- Shaving
- Waxing
- Plucking
- Threading
Ingrown hairs result in firm, acne-like lesions that can be itchy or sore. Depending on the skin color of the person who gets them, they can be skin-colored, red, or dark. Sometimes, the lesions can fill with liquid that resembles pus. Although these breakouts appear similar to acne, they are a completely different phenomenon.
When they are caused by shaving, they are often called “razor bumps” or “shave bumps.”
Who Is Most Likely to Develop Ingrown Hairs?
Although anyone can develop an ingrown hair from time to time, they are most common in people whose hair curls tightly. Since people of African descent typically have curly hair, they are more prone to developing ingrown hairs than people of European descent. Because of this, black men who shave facial hair are much more likely to develop them than white men who shave facial hair. As Drs. Beth and Adam Goldstein, both professors of medicine at the University of North Carolina, wrote on a website for doctors called UpToDate, “Between 45 and 83 percent of black men and 3 percent of white men who shave facial hair develop [a problem with ingrown hairs].”1
Interestingly, genetics may be at play as well: one study found that a specific genetic mutation may make some people more prone to developing ingrown hairs. Incidentally, black people are three times more likely to have this mutation compared to people of Caucasian background.2,3
Regardless of ethnicity, most people will develop an ingrown hair from time to time–including women who remove hair. Ingrown hairs most often appear on the cheeks and front of the neck. However, they can develop on any area of the body where a person removes hair, such as the legs, armpits, or pubic region.
How Do Ingrown Hairs Develop?
When a hair is shaved off or removed by plucking or waxing, it soon begins to regrow. Sometimes the hair becomes trapped in the skin, causing the body to see its own hair as an “intruder.” The body reacts with an inflammatory response, which is the body’s reaction to any “foreign object.” This defensive reaction causes the typical signs of inflammation, such as redness, swelling, heat, and soreness. You can see this reaction when you harm the skin with a wooden splinter and do not remove it immediately: after a while, the skin displays characteristics of inflammation.
When allowed to grow naturally, a hair normally emerges through a pore in the skin. However, when a shaved, plucked, or waxed hair grows, things can go off course. This can occur in one of two ways:
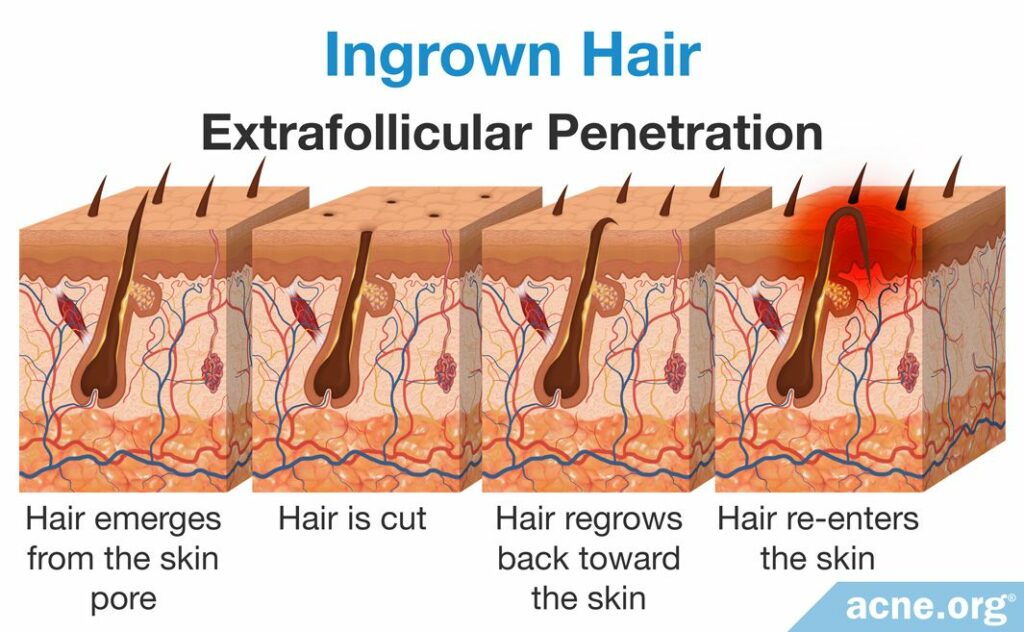
- Extrafollicular penetration: In extrafollicular penetration, the hair emerges from the skin pore, but then curls back on itself and re-enters the skin near the follicle. In other words, a loop of hair is formed above the skin. This is especially likely to occur when the hair is curly, short, and has a sharp end due to shaving. As the hair continues to grow, it eventually finds its way out of the skin again, but this can take several weeks.
- Transfollicular penetration: In transfollicular penetration, instead of emerging from the skin pore, the hair pierces the wall of the hair follicle and grows into the surrounding skin. That is to say, there is no loop rising above the skin surface. Rather, the hair remains inside the skin, but instead of growing directly through the pore and out of the skin, it becomes trapped. The hair may continue to grow several millimeters through the dermis, the middle layer of skin, before finding its way out. This typically takes 3-6 weeks. Just like in extrafollicular penetration, transfollicular penetration is more likely to occur if the hair is curly and has a sharp end.
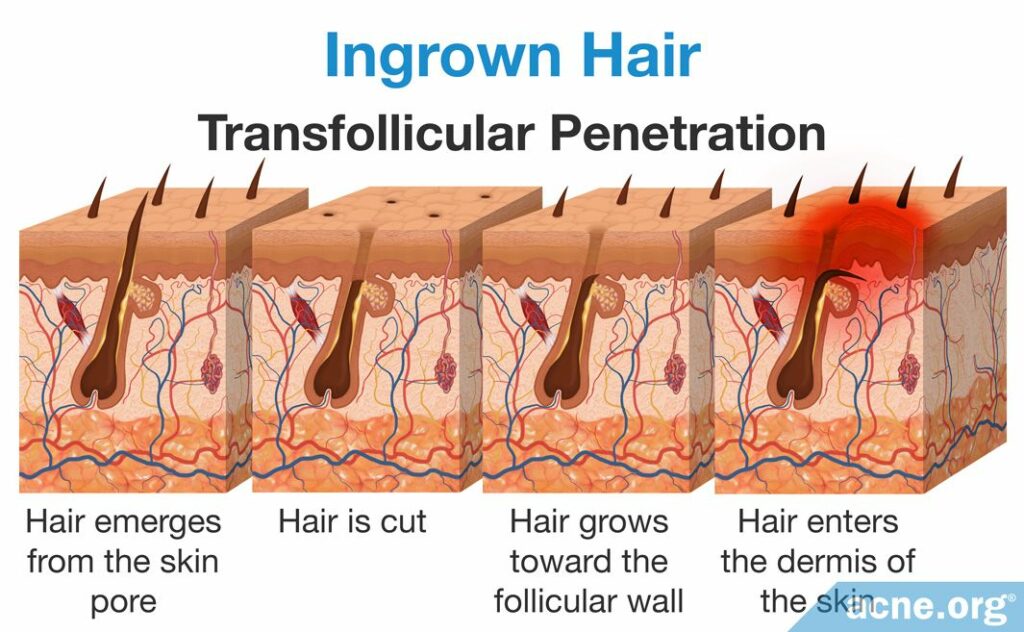
Transfollicular penetration can result from stretching the skin when shaving. When a person stretches an area of skin, passes over it with a razor, and then lets go of the skin, the cut hairs shrink back into their follicles. This results in short, sharp-ended hairs just under the skin surface, and these hairs are especially likely to take the wrong path when they start to regrow.
Multi-blade razors contribute to transfollicular penetration in a similar manner. When a person shaves with a multi-blade razor, the first razor edge pulls the hairs upward and the next razor edge cuts the hairs. After shaving, the hairs shrink back into their follicles. This results in short hairs with sharp ends just beneath the skin surface. Such hairs are likely to grow into the surrounding skin, instead of through the pore.
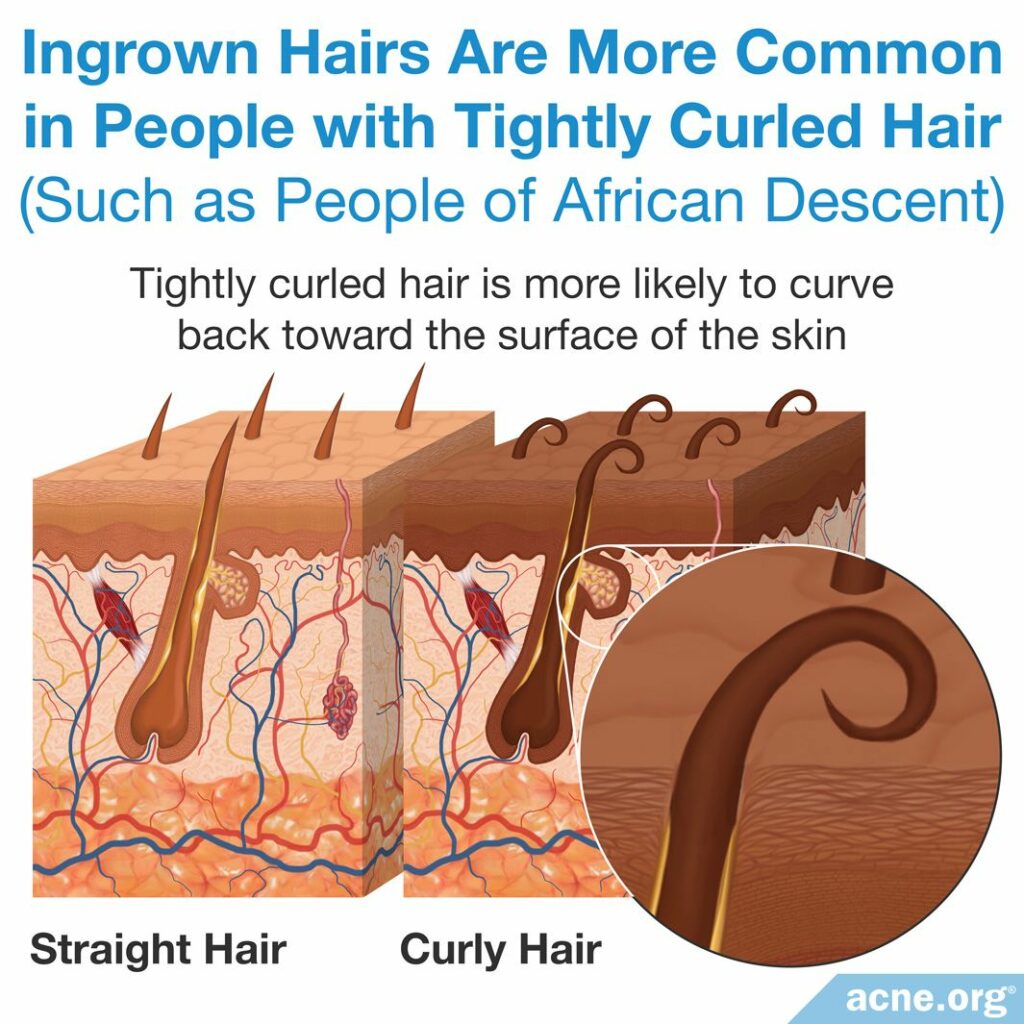
People with tightly curled hair, such as people of African descent, are particularly likely to develop ingrown hairs for two reasons.
- Tightly curled hair is more likely to curve back toward the surface of the skin.
- Hair follicles in people with tightly curled hair are usually angled obliquely to the skin surface, meaning that instead of the hair emerging at a 90-degree angle to the skin surface, the hair comes out at a slant. This angle makes it more likely that a close shave will create hairs with sharp, rather than blunt, edges.1
Once a regrowing hair pierces the skin by either extrafollicular or transfollicular penetration, the spot where the hair is trapped becomes inflamed, and a dense, flesh-colored or red or hyperpigmented (darker than the surrounding skin) papule appears. Soon, a pustule (a fluid-filled lesion) may form at the site of the ingrown hair. In contrast to acne pustules, which are filled with pus and bacteria, pustules due to ingrown hairs are often sterile, meaning they are not filled with pus or bacteria. Instead, these pustules contain liquid that comes from the blood vessels near the ingrown hair, which leak liquid into the area. The blood vessels around the hair also swell, causing the skin to become red and warm to the touch. However, scratching or picking at ingrown hairs can cause an open wound–even if that open wound is merely a tiny crack in the skin–which can let bacteria into the skin and lead to infection. If this occurs, pustules containing bacteria and pus may develop, just like in acne.1,4
Hyperpigmentation after an ingrown hair heals
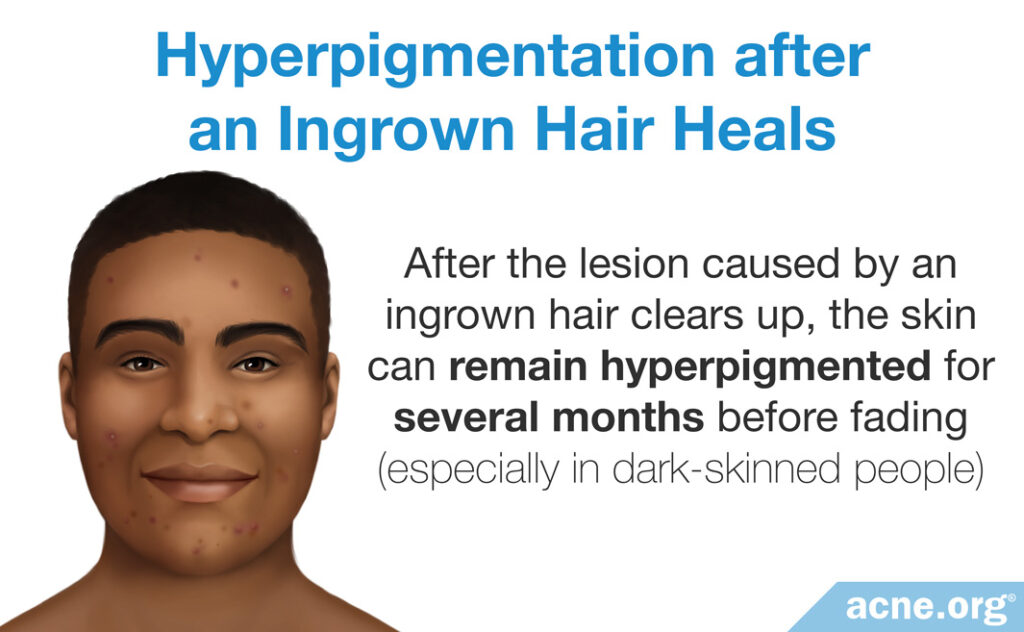
After the lesion caused by an ingrown hair clears up, the skin can remain hyperpigmented for several months before fading. This is especially likely to occur in dark-skinned people.
Prevention and Treatment
Management of ingrown hairs should be focused on prevention, rather than treatment. Additionally, some topical medications are available to treat ingrown hairs.
There are three possible approaches to preventing ingrown hairs.
- Stopping hair removal
- Proper shaving
- Long-term hair reduction
Stopping hair removal

Discontinuing shaving, waxing, plucking, and/or threading, and allowing the hair to remain at a length that makes penetration of the is the most effective preventative measure against ingrown hairs. For men, grooming the beard with scissors or an electric clipper can be an alternative to shaving. It is recommended not to cut the hair shorter than 0.5cm (5mm), at least until ingrown hairs clear up. Depending on the person and the severity of the condition, ingrown hairs and any associated hyperpigmentation can take from one to six months to resolve.
Proper Shaving

Sometimes, discontinuing hair removal is undesirable or even impossible, such as for men in the U.S. Army and Marine Corps, who are not permitted to grow beards.
If you continue to shave, you may want to adjust your shaving routine by following these tips:
- Soften the hair before shaving by shaving at the end of a shower, using a highly lubricating shaving cream, and/or applying a shave oil under shaving cream. Do not practice dry shaving!
- Use only a one- or two-blade, low-irritation razor and avoid the multi-blade razors.
- Shave exclusively in the direction of hair growth, which is normally downward on the face and the top half of the neck and upward on the bottom half of the neck.
- Avoid stretching the skin during shaving.
- If you do have an ingrown hair, be careful when you shave over it. Shave gently, using only the necessary amount of pressure possible with the razor.
Other Short-term Hair Removal Options
Instead of changing the way you shave, consider replacing razor blades with electric clippers that leave the hair at least 5 mm long so that the hair does not curl back and pierce the skin.
Another option is using chemical hair removal powders and creams. Unfortunately, these products tend to have an unpleasant smell and can also cause skin irritation, which is a no-no for acne-prone skin, as irritation can bring on a breakout.5
Some companies are now working on developing manual razors with a foil guard that prevents shaving the hair too close to the skin. Early research suggests such products may help reduce the likelihood of ingrown hairs.5
Long-term hair reduction
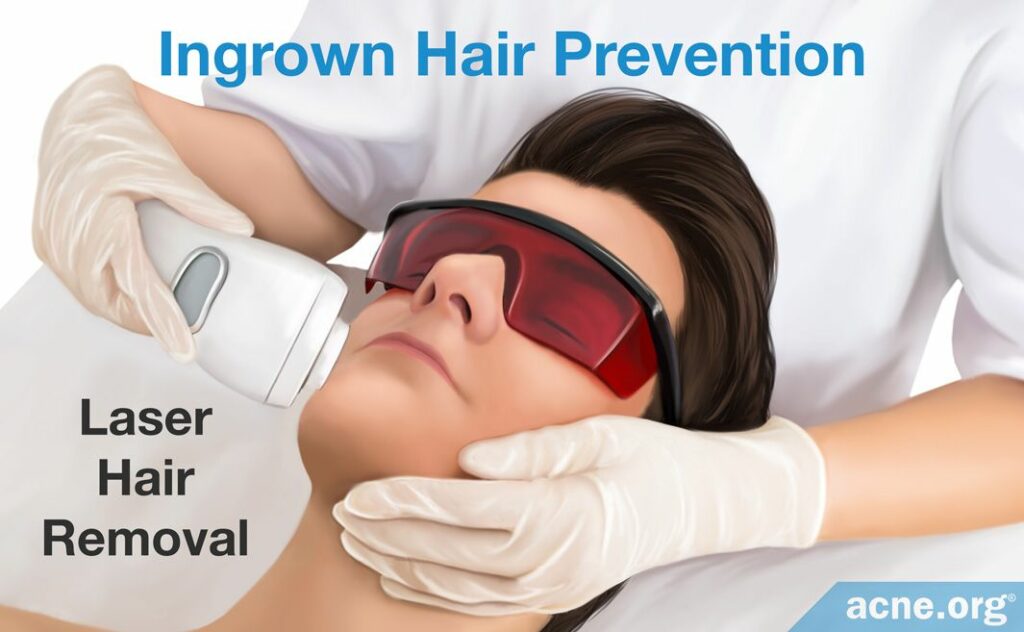
The problem of recurring ingrown hairs can be solved by long-term hair reduction, which destroys the hair follicles. Of course, the downside is that a person can no longer grow hair in that area–for example, a man who undergoes long-term reduction of facial hair will no longer be able to grow a beard.
Long-term hair reduction can be accomplished by laser hair removal. It usually requires several sessions in order to achieve a major reduction in hair growth, because each treatment only destroys a small fraction of hair follicles.5 In addition, maintenance treatments might be necessary once a year or so to prevent gradual regrowth of the hair.6
The lasers work by targeting the dark pigment called melanin, which can be found in both skin and hair. Laser hair removal is most effective when a person’s hair contains more melanin, i.e., is darker than, the skin. The laser can then safely destroy the hair follicles without damaging the pigment in the skin. Conversely, the treatment does not work well for people with blond or gray hair because their skin is as dark as, or sometimes even darker than, the hair. Drs. Beth and Adam Goldstein wrote, “[P]atients with darkly pigmented hairs are the best candidates for this procedure. The treatment is poorly effective for white or [gray] hairs.”1
Potential risks of laser hair removal include temporary or permanent changes in skin pigmentation, blistering, and scarring. The risk of changes in skin pigmentation is higher for individuals with darker skin. To minimize the chances of this side effect, the clinician should perform a spot test on an area of the skin that is hardly visible, so that he or she can adjust the laser settings prior to treatment.
Topical treatments for ingrown hairs

The most common drugs used to treat ingrown hairs are:
- Benzoyl peroxide, especially when combined with alpha hydroxy acids. This is why so many men find that The Regimen eliminates ingrown hairs. Alpha hydroxy acids can help with persistent hyperpigmentation as well.
- Topical retinoids (tretinoin, adapalene, tazarotene, trifarotene)
- Low-potency topical corticosteroids
- Topical antimicrobials, such as erythromycin and clindamycin7
Information on the efficacy of these treatments is limited, and more research is needed to determine how helpful these and other drugs may be in treating ingrown hairs.
References
- Goldstein, B. & Goldstein, A. Pseudofolliculitis barbae. (2017). https://www.uptodate.com/contents/pseudofolliculitis-barbae
- Ogunbiyi, A. Pseudofolliculitis barbae; current treatment options. Clin. Cosmet. Investig. Dermatol. 12, 241 – 247 (2019). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6585396/
- Winter, H., Schissel, D., Parry, D. A. et al. An unusual Ala12Thr polymorphism in the 1A alpha-helical segment of the companion layer-specific keratin K6hf: evidence for a risk factor in the etiology of the common hair disorder pseudofolliculitis barbae. J. Invest. Dermatol. 122, 652 – 657 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15086549
- Oakley, A. Folliculitis barbae and pseudofolliculitis barbae, https://www.dermnetnz.org/topics/folliculitis-barbae/ (2016)
- Alexis, A., Heath, C. R. & Halder, R. M. Folliculitis keloidalis nuchae and pseudofolliculitis barbae: are prevention and effective treatment within reach? Dermatol. Clin. 32, 183-191 (2014). https://pubmed.ncbi.nlm.nih.gov/24680005/
- Mayo Clinic: Laser hair removal. Available at: https://www.mayoclinic.org/tests-procedures/laser-hair-removal/about/pac-20394555
- Ogunbiyi, A. Pseudofolliculitis barbae; current treatment options. Clin. Cosmet. Investig. Dermatol. 12, 241-247 (2019). https://pubmed.ncbi.nlm.nih.gov/31354326/
 Acne.org Products
Acne.org Products