Sulfur Smells Bad, but Is a Useful Aid in the Treatment of Acne, Especially When Combined With Other Medications

The Essential Info
Sulfur is a time-tested topical treatment for acne that people have been using since the 5th century BC for its ability to:
- Shed the outer layer of skin cells. This helps prevent pores from becoming clogged.
- Inhibiting the growth of acne bacteria.
However, due to the unpleasant odor of sulfur and the temporary skin discoloration that it can impart, topical treatments containing only sulfur are unpopular. This is why you’ll usually find it combined with benzoyl peroxide or sodium sulfacetamide (a prescription medication). Combining sulfur with these other medications cuts down on the unpleasant odor and also increases effectiveness. Caution: You should not use sulfur combined with sulfacetamide if you are allergic to sulfa drugs.
Side effects of topical sulfur include:
- Dryness
- Peeling of the skin
- Occasional cracking/splitting of the skin around the mouth
The higher the percentage of sulfur you use, the more side effects you can expect.

The Science
Topical application of sulfur has been used to treat various skin conditions since the time of Hippocrates (5th century BC). Since the 1960s, modern science has validated its effectiveness in treating acne, particularly when combined with other ingredients such as benzoyl peroxide.
Sulfur is used to treat a variety of conditions, including:
- Acne
- Seborrheic dermatitis (scaly patches and red skin, usually on the scalp)
- Rosacea
- Scabies
- Fungal infections
In nature, sulfur is a yellow, nonmetallic element found in the Earth’s crust. A particular type of sulfur called colloidal sulfur is the most commonly used and most potent form of sulfur due to the smaller size of its particles, which makes it work better when applied to the skin.
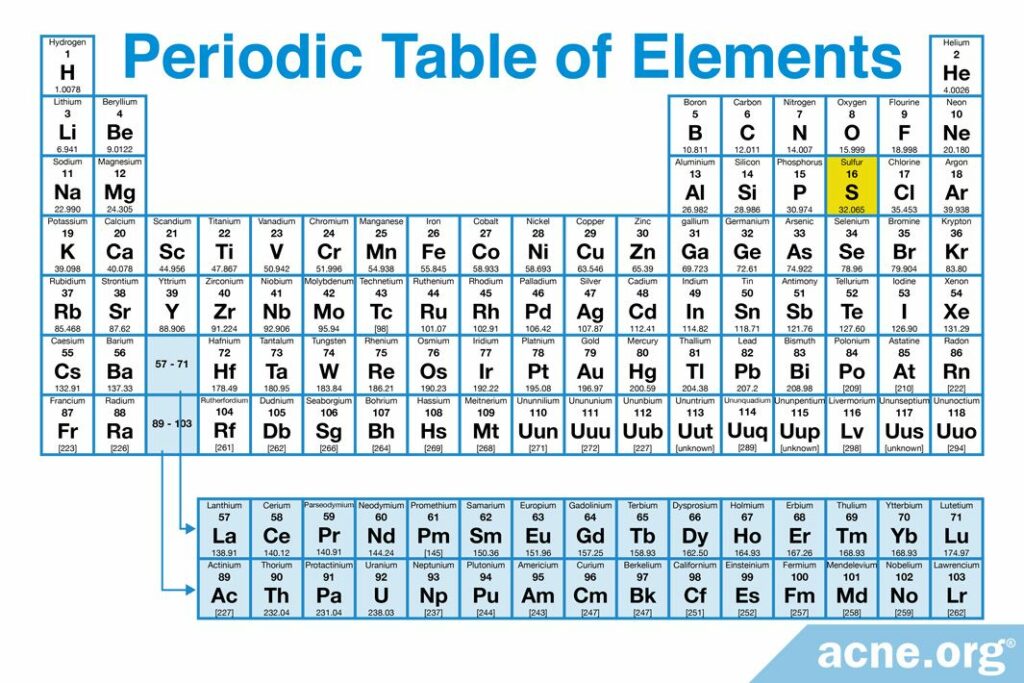
How Sulfur Works on Acne
Sulfur helps with acne in two ways:
- Promoting the shedding of the outer layer of skin cells, helping prevent pores from becoming clogged.
- Inhibiting the growth of acne bacteria.
Expand to read the deeper science of how sulfur works
Keratin is a sticky protein that clogs up skin pores. Sulfur is keratolytic, which means that it breaks down keratin. This helps prevent pores from clogging.
Combining sulfur with other medications makes it even more keratolytic and also alleviates some of the unpleasant effects of sulfur alone, such as temporary skin discoloration and its unpleasant smell.2
Scientists have yet to discover on a cellular level exactly how sulfur works, but research suggests that:
- It may work because a reaction between the sulfur and cysteine, an amino acid found in the skin, aids in the formation of hydrogen sulfide ions, which break down keratin in the skin cells.2
- Sulfur inhibits the growth of acne bacteria (Cutibacterium acnes or C. acnes for short).3
When combined with other medications, sulfur may work in these ways:
Combined with benzoyl peroxide:
- Benzoyl peroxide may increase the skin shedding effect of sulfur.
Combined with sodium sulfacetamide (a prescription medication):
- Sulfur combined with sodium sulfacetamide demonstrates anti-inflammatory properties.1 Since acne is at its root an inflammatory disease, anything that reduces inflammation may reduce acne.
How Well Sulfur Works – Study Results
Because sulfur alone isn’t as effective as it is when combined with other medications, and because sulfur alone can produce skin discoloration and has a bad odor, it is rarely used on its own.4 The few sulfur-only products that exist, like Vleminckx’s solution and Ress’ solution, are primarily used in countries where newer medications may be unavailable.5
There is more research on the efficacy of sulfur when combined with other ingredients, like benzoyl peroxide6 and sodium sulfacetamide7,8, in the form of lotions, creams, soaps, and ointments. These combination treatments usually contain sulfur in concentrations from 1 – 10%.
When it comes to using sulfur together with benzoyl peroxide, one study found that this combination treatment successfully controlled mild-to-moderate acne within three or four months, and very severe acne within six to nine months.6 Another study found that a 3-month course of treatment with sulfur together with sodium sulfacetamide reduced the number of acne lesions by 78%.9
Expand to read details of studies

A 1965 study published in the Canadian Medical Association Journal showed that sulfur combined with benzoyl peroxide is a potent agent against even severe body acne. In this study, sulfur was combined with benzoyl peroxide to treat 286 participants with acne, and the results showed that:
- Mild to moderate acne was suppressed within two weeks and controlled within three to four months.
- Moderately severe acne responded quickly to the treatment, and control over acne symptoms was achieved within four to six months.
- Cystic acne on the face and also on the chest and back was controlled within six months.
- Severe cystic acne was the most resistant, but control was achieved within six to nine months.6

In a 1993 study published in the International Journal of Dermatology, Breneman and Moira examined the effectiveness of a sodium sulfacetamide (10%) and sulfur (5%) lotion in 60 women aged between 22 – 45 years of age with mild to moderate acne.9
The study followed patients over a 12-week study period, and the results found that:
- Using sodium sulfacetamide (10%) and sulfur (5%) lotion for 12 weeks for mild to moderate acne effectively decreased total acne lesions by 78%.
- Physician Global Assessment (PGA) scores showed that 53 of 54 patients (98.2%) were “moderately better” and “much better” after 8 weeks of treatment, and by week 12 all 54 patients showed similar improvement.9

In a 2009 article in the Journal of Clinical and Aesthetic Dermatology, researchers described eight cases of acne treated with a topical foam containing 5% sulfur and 10% sodium sulfacetamide. They found that the sulfur-sodium sulfacetamide foam was effective against acne. However, it is important to note that some of the patients also received other topical acne treatments, such as retinoids (tretinoin, adapalene, or tazarotene). In other words, it is impossible to know how much sulfur contributed to the improvement.
The authors noted that the sulfur-sodium sulfacetamide foam decreased skin irritation caused by topical retinoids, suggesting that sulfur and topical retinoids might be a useful combination. They also commented that combining sulfur with sodium sulfacetamide reduced its unpleasant odor.10
Side Effects
While uncommon, adverse effects of topical sulfur products include:
- Unpleasant odor
- Temporary discoloration of skin
- Drying, peeling, and swelling of the skin2,6,7,10-12
Pregnancy: Sulfur is a category C drug, which means there are no adequate studies performed on humans but potential benefits may warrant its use in pregnant women despite the potential risks.7 It is always important to speak with your doctor before using any medications, topical or otherwise, during pregnancy.
While preparations containing sulfur alone normally are well tolerated, preparations combined with sodium sulfacetamide are not recommended for patients with a sulfa allergy.11 Sulfa allergies can cause a number of symptoms varying in severity. The most common symptoms are skin reactions such as:
- Redness
- Maculopapular rash (a rash that contains both a discolored area of skin and small, raised bumps)
- Morbilliform rash (small lesions that may combine to form larger lesions and hives and itching)13
These reactions occur generally within a few days of treatment and cease promptly after discontinuation. Although uncommon, patients with sulfa allergies can experience anaphylaxis (a life-threatening allergic reaction). Symptoms of anaphylaxis include hives, swelling of the lips and around the eyes, swelling of the windpipe, constriction of respiratory pathways, gastrointestinal disturbances, and low blood-pressure.13
References
- Keri, J. & Shiman, M. An update on the management of acne vulgaris. Clin Cosmet Investig Dermatol 2, 105 – 110 (2009). https://www.ncbi.nlm.nih.gov/pubmed/21436973
- Lin, A. N., Reimer, R. J. & Carter, D. M. Sulfur revisited. J Am Acad Dermatol 18, 553 – 558 (1988). https://www.ncbi.nlm.nih.gov/pubmed/2450900
- Abramovits, W. & Kennedy, A. J. Sulfur/sodium sulfacetamide preparations. Skinmed 3, 95 – 101 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15010636
- Liu, H., Yu, H., Xia, J., Liu, L., Liu, G. J., Sang, H. & Peinemann, F. Topical azelaic acid, salicylic acid, nicotinamide, sulphur, zinc and fruit acid (alpha-hydroxy acid) for acne. Cochrane Database Syst Rev 5, 1-263 (2020). https://pubmed.ncbi.nlm.nih.gov/32356369/
- Kaminsky, A. Less common methods to treat acne. Dermatology 206, 68 – 73 (2003). https://www.ncbi.nlm.nih.gov/pubmed/12566807
- Pace, W. E. A Benzoyl Peroxide-Sulfur Cream for Acne Vulgaris. Can Med Assoc J 93, 252 – 254 (1965). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1928665/
- Akhavan, A. & Bershad, S. Topical acne drugs: review of clinical properties, systemic exposure, and safety. Am J Clin Dermatol 4, 473 – 492 (2003). https://www.ncbi.nlm.nih.gov/pubmed/12814337
- Davis, S. Topical treatment of acne: skin care. SA Pharmacist’s Assistant 13, 42 – 44 (2013). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3997205/
- Breneman, D. L. & Ariano, M. C. Successful treatment of acne vulgaris in women with a new topical sodium sulfacetamide/sulfur lotion. Int J Dermatol 32, 365 – 367 (1993). https://www.ncbi.nlm.nih.gov/pubmed/8505165
- Del Rosso, J. Q. The use of sodium sulfacetamide 10%-sulfur 5% emollient foam in the treatment of acne vulgaris. J Clin Aesthet Dermatol 2, 26 – 29 (2009). https://pubmed.ncbi.nlm.nih.gov/20729951/
- Feldman, S., Careccia, R. E., Barham, K. L. & Hancox, J. Diagnosis and treatment of acne. Am Fam Physician 69, 2123 – 2130 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15152959
- Russell, J. J. Topical therapy for acne. Am Fam Physician 61, 357 – 366 (2000). https://www.ncbi.nlm.nih.gov/pubmed/10670502
- Kelly, T. E. & Hackett, P. H. Acetazolamide and sulfonamide allergy: a not so simple story. High Alt Med Biol 11, 319 – 323 (2010). https://www.ncbi.nlm.nih.gov/pubmed/21190500
 Acne.org Products
Acne.org Products