A Bit Helps But Too Much Hurts

The Essential Info
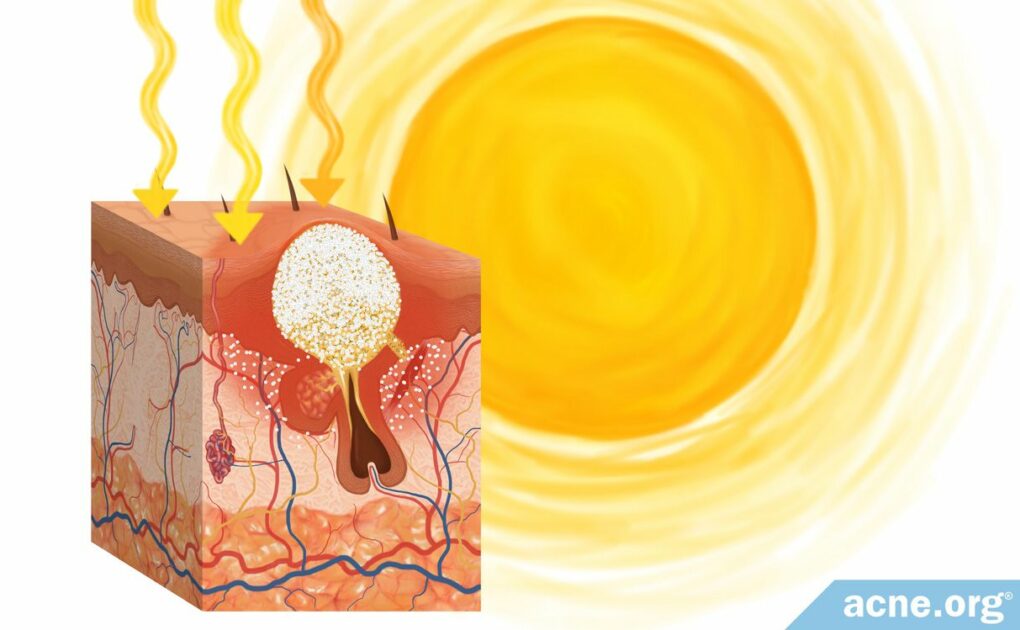
Moderate sun exposure may be helpful for achieving adequate vitamin D levels in the body, which may potentially help with acne to some degree. The sun’s UV rays may also help kill acne bacteria and lessen inflammation, both of which could also help with acne.
However, too much sun exposure causes sunburn, which is highly irritating to the skin. Anything that irritates the skin can lead to acne as the skin repairs itself. If you find that you are breaking out “for no apparent reason” consider if you got a sunburn in the week or two prior to the breakout.
The Research: Research looking at how sunlight directly affects acne is limited and contradictory, so we cannot definitively say whether getting some sun directly on acne-prone skin will help. But suffice it to say that getting too much sun is a bad idea.
The Bottom Line: For people with the lightest skin, getting up to 20 minutes of unprotected sun exposure will help you keep your vitamin D levels up, and might–we really don’t know, but it might–help alleviate acne to some degree. For people with the darkest skin, aim for 2 hours. The key is to not stay in the sun so long that you get burnt. Err on the side of caution.

The Science
- Sun’s Effect on Acne
- Studies Using Artificial Light
- Studies Looking at Seasonal Variations
- Vitamin D and Acne
- Light & Laser Treatment for Acne
- Potential Side Effects of Sun Exposure
- The Bottom Line
The Sun’s Effect on Acne Is Still an Open Question
There is limited and conflicting scientific evidence to support the use of sunlight in treating acne. In fact, partly due to the fact that it is difficult to perform studies on sun exposure, there are no reliable studies that look directly at the effect of sunlight on acne.
For this reason, to get an approximate answer to the question of whether the sun helps or hurts acne we need to look at two other types of studies that can potentially shine light (no pun intended) on this question:
- Studies using artificial light on acne: Because some days are cloudier while other days are sunnier, this makes it hard to control for sun exposure in studies. For this reason, scientists will often instead opt for artificial light sources like sun lamps which can be shone on the skin at exact wavelengths and for exact amounts of time. These studies indicate that some light wavelengths might have a beneficial effect on acne while other studies indicate the opposite. In other words, the evidence is conflicting.
- Studies looking at seasonal variations in acne: There are also several studies that examine seasonal variations in acne, which could show us whether acne tends to improve or worsen in the summer, when people get more sun exposure, but these studies also produce conflicting evidence.
As we can see, based on the evidence we have so far, we can’t say whether the sun’s rays will benefit acne. However, let’s look more closely at these two types of studies one by one, starting with studies using artificial light, and see what we can suss out.
Studies Using Artificial Light
Studying the effects of sunlight can be fraught with error because depending on cloud cover, latitude, season, and time of day, sun exposure can vary greatly.
Therefore, scientists have resorted to artificial light in their experiments, while fully admitting that artificial light may not be directly generalizable to natural sunlight.1 In other words, we cannot necessarily say that natural sunlight will have the same effects as artificial light, but at least it gives us a clue.
Several teams of scientists have taken a critical look at all the studies on artificial light and acne so far. Unfortunately, they came to the conclusion that the evidence is conflicting and weak. In other words, the jury is very much still out when it comes to the effects of artificial light on acne.1-3
Expand to read details of analysis

One systematic review looking at the effect of artificial light on acne was published in the journal Family Practice in 2005. This systematic review examined all the studies on this topic to date to draw overall conclusions.
According to several of the reviewed studies in the analysis, “Trials of artificial UV-B, UV-A and combined light sources, and phototherapy with artificial blue-red, blue, violet, green and full-spectrum light sources have been found to improve acne.” However, the authors noted that these studies had methodological problems that limit the ability to interpret their results.
In contrast to the other studies reviewed in the meta-analysis, a trial of UV (ultraviolet) light applied to rabbit ears resulted in an increased tendency for sebum (skin oil) to form acne comedones. Rabbit ears are the closest animal model to human skin. This result suggests that light might cause pores to become clogged and make acne worse.1

A more recent systematic review published in the Cochrane Database of Systematic Reviews in 2016 found no hard evidence that artificial light is effective in the treatment of acne. The authors concluded that the usefulness of blue and red light therapy for moderate-to-severe acne is questionable and highlighted the need for more carefully designed studies. They wrote, “High-quality evidence on the use of light therapies for people with acne is lacking.”2

Another systematic review published in the Annals of Family Medicine in 2019 reached the same conclusion. The researchers examined 14 studies that tested blue light on people with acne. They found that most of the studies were too small and too short to draw firm conclusions about the efficacy of blue light for acne.3
Studies Looking at Seasonal Variations
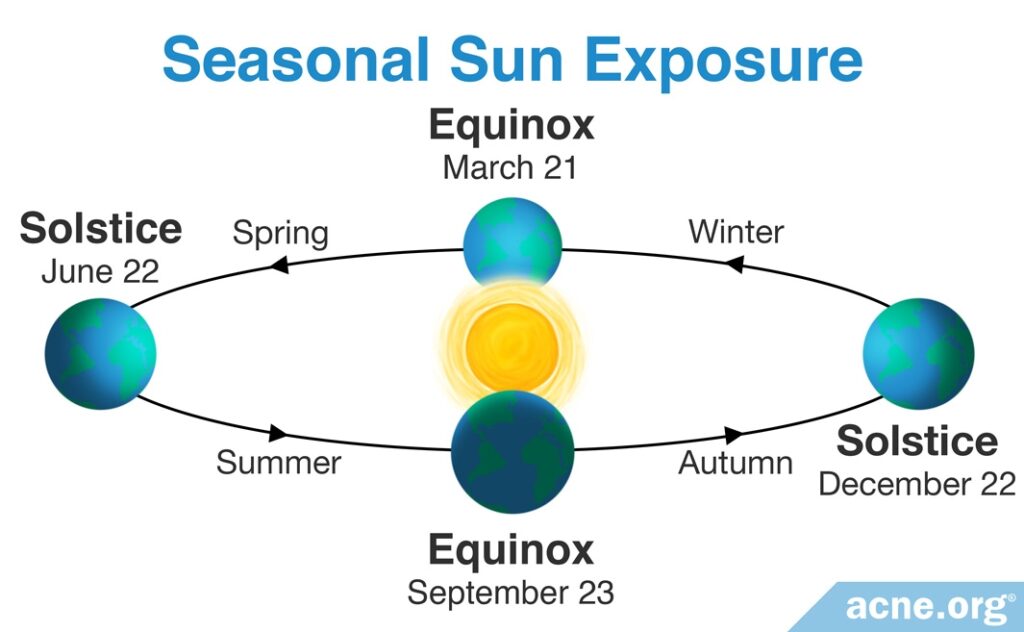
The sun is highest in the sky in the summer, so we can look to studies on seasonal variations to see if we can find some other evidence on sun exposure and acne.
But you guessed it, the studies that have been performed so far reach conflicting conclusions. The majority of studies show improvement of acne during summer months, but some others point toward a worsening of acne in the summer.4-8 Also, many of these studies use self-reported data, which is unreliable. Therefore, due to the conflicting results and less than ideal study methodology, we cannot draw conclusions from them.
Expand to read details of studies

According to a 1989 study in the journal Photodermatology, in which the authors examined and interviewed 809 randomly selected people from four different Swedish cities, “The majority of subjects with atopic eczema, acne vulgaris or seborrheic dermatitis experienced improvement after exposure to sunlight.”4

A 1996 study in the International Journal of Dermatology found no effect of season-dependent sun exposure on acne severity. The authors asked 139 patients whether their acne worsened during summer or during winter, whether their acne improved seasonally, and whether they noticed any change at all with different seasons. This study states, “About one-third of the patients reported an aggravation of their acne in winter, but also approximately one-third of the patients complained about an aggravation of their acne in summer. Another third did not notice any change.”5

A 2002 study in The Journal of Dermatology asked 452 patients about seasonal variations in their acne. This study found that about half of patients noticed seasonal variations: the majority of these (56.33%) noted that their acne was worse in summer; 16% improved in summer, and only 11.35% said their acne was worse in winter. The authors commented, “Significantly, a majority (80.62%) of patients noticed a summer aggravation due to sweating and increased humidity.”6 The authors noted that their results contradicted other studies that indicate improvement in the summer and worsening in the winter, and they proposed that the increased temperature, humidity, and sweating in their region might account for the majority of patients whose acne worsened in the summer in this study.

A more recent small study from 2015, in the Journal of Drugs in Dermatology, compared the facial skin of 17 adolescent males with and without acne over the course of one year. This study found that “[Skin oil] production was significantly greater in subjects with acne than in those without for each season examined…and was lowest in the winter and highest in the fall.”7

Another 2015 study in the Journal of the American Academy of Dermatology collected data for 9301 acne patients, 73% of whom were female. This study found that acne cleared in the fall and worsened in the winter. In addition, analysis of 6101 patients who were seen multiple times indicated a “significant trend of summer clearing…and winter worsening.” The authors suggested that summer improvement may be attributed to the known immune-regulating and antibacterial effects of the sun. Ultraviolet light, which suppresses the immune system and decreases inflammation, may be the cause of the summer/fall improvement in acne.8

A study published in the journal Experimental Dermatology in 2018 looked at seasonal changes in skin function. The researchers found that people with acne had lower levels of substances called ceramides in their skin in the winter months (measured in November and February) compared to the summer (measured in August). Ceramides are specialized fats that help form the skin barrier. The skin barrier is the outermost layer of skin, and a strong and healthy skin barrier is important for staying acne-free. Therefore, the researchers concluded that lack of ceramides in the skin in winter may contribute to acne flare-ups.9
Since we will need more research before we can say for sure how the sun affects acne, the next thing we can take a look at is vitamin D and how it might affect acne.
Vitamin D and Acne

Vitamin D is an extremely important vitamin for the health of the skin. People with acne tend to have lower levels of vitamin D in the blood, and there is some evidence that vitamin D can help in the treatment of acne. Since exposure to sunlight is the only way that the body produces vitamin D, it is reasonable to question whether sun exposure might help improve acne for this reason.
Preliminary studies done so far show us that severe acne might go along with vitamin D deficiency and that administering vitamin D might potentially help improve acne.10-13 In other words, getting some sun exposure might indirectly be beneficial for acne if it increases our vitamin D levels. But we should interpret the conclusions from these preliminary studies with caution because they are just that–preliminary.
Expand to read details of studies

A 2011 article in Dermato-Endocrinology notes that vitamin D has antimicrobial (anti-bacterial) effects, and that vitamin D deficiency has negative effects on general well-being. The authors state, “Vitamin D and its analogues…are playing an increasing role in the management of [skin conditions such as] atopic dermatitis, psoriasis, vitiligo, acne and rosacea.” The article states also, “Vitamin D constitutes an inexpensive [preventive] option and possibly therapeutic product either by itself or as a synergistic agent to traditional antimicrobial agents.”10

According to a 2013 study in the Indian Journal of Dermatology, sebocytes (skin oil cells) treated in vitro (in the lab) with vitamin D caused these cells to decrease their production of proteins that contribute to inflammation.11

A small 2014 study in Dermato-Endocrinology compared blood levels of vitamin D in patients with nodulocystic (severe) acne with those of healthy controls. This study declares, “The patients with nodulocystic acne had relatively low serum vitamin D levels compared with the subjects in the control group. The findings from this study suggest that there is a connection between low vitamin D levels and acne.”12

Another study published in the journal PloS One in 2016 compared vitamin D levels in the blood of 80 people with acne and 80 people without acne. The authors found that Vitamin D deficiency was more frequent in people with acne. Specifically, 48.8% of people with acne were deficient in vitamin D, compared to 22.5% of people without acne.
In the second part of the study, the researchers looked only at the 39 people with acne who were vitamin D-deficient. The scientists randomly split these people into two groups:
- Group 1 consisted of 20 people who received an oral vitamin D supplement every day for two months
- Group 2 consisted of 19 people who received an oral placebo (similar-looking supplement without vitamin D) every day for two months
After 2 months, the researchers looked for acne improvements in Group 1 and Group 2. They found that the number of inflammatory acne lesions decreased in Group 1 more than in Group 2.
This study provides some evidence that a vitamin D deficiency may predispose people to developing acne, and that correcting a vitamin D deficiency might help with acne.13

Lastly, a study published in the Journal of Cosmetic Dermatology in 2019 also evaluated vitamin D levels in 90 people with acne. The scientists concluded that the people with the lowest vitamin D levels tended to have the most severe acne. However, the researchers could not determine whether low vitamin D levels make acne worse, or whether having severe acne somehow causes vitamin D deficiency.14
How to Get the Right Amount of Vitamin D
Regardless of whether getting sun exposure will allow you to improve your acne, it is important to get the vitamin D you need for your overall health. Vitamin D deficiency is pervasive in modern society due to restricted time in the sun and the use of sunscreens. Therefore, if blood vitamin D levels are low, doctors recommend spending time in the sun. However, the amount of sun required varies according to several factors, including:
- Skin pigmentation (light or dark)
- Age
- The amount of exposed skin
- Latitude
- Season
Because of these variations, the amount of sun exposure a given individual might need varies. For instance, closer to the equator, people need less sun exposure than they would the further they get from the equator. Also, people need far more sun exposure during winter months to achieve the same amount of vitamin D they would get during summer months. Using common sense is often best. Get a little sun when you can, but limit your sun exposure so that you do not get burnt.15,16
Light & Laser Treatment for Acne – Does This Give Us Any Clues?
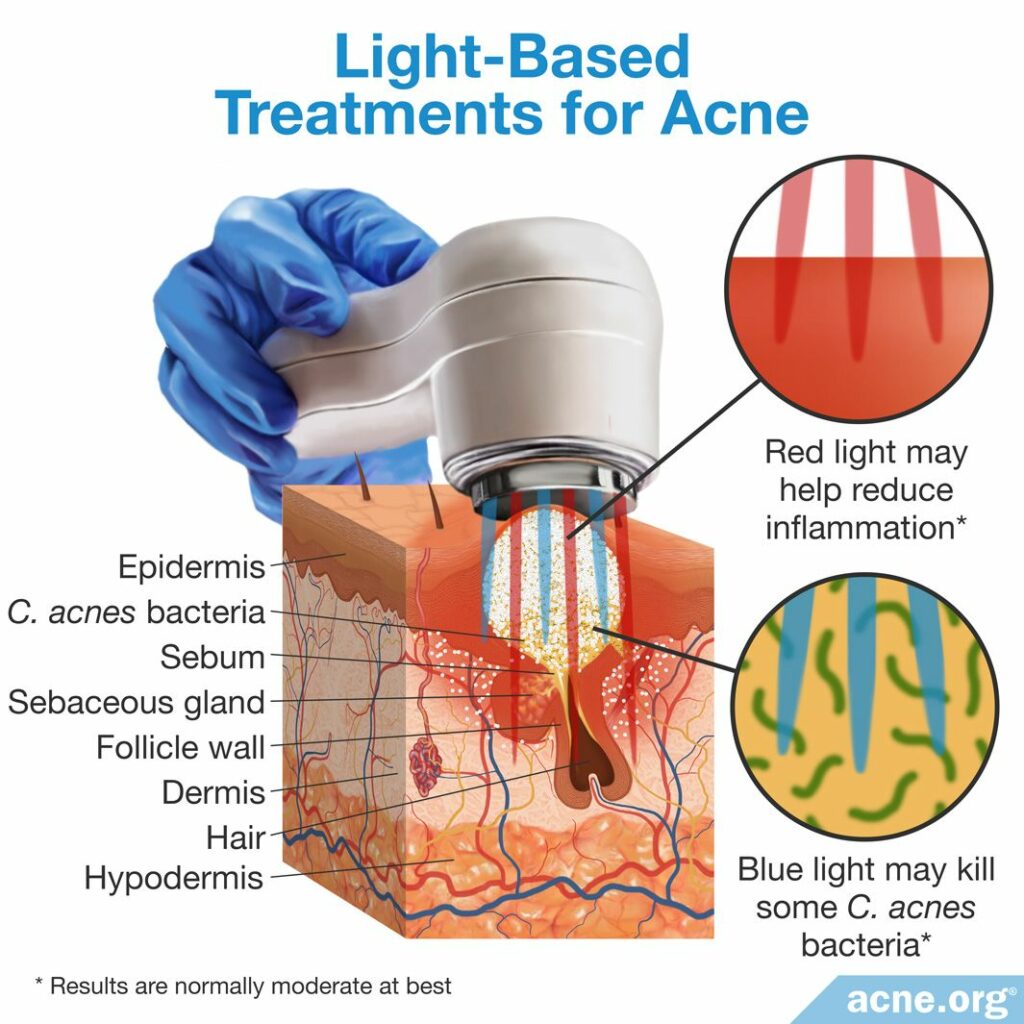
Light and laser-based treatments for acne use various forms of light to reduce acne symptoms. These treatments, which rely on the antibacterial and anti-inflammatory properties of several wavelengths of light, usually are somewhat effective.
Whether the sun would offer similar benefits is unknown, but because light and laser therapy do help reduce acne to some degree, it is possible that the sun’s rays could do the same.
Three recent studies suggest that light and laser therapy may help with acne by lowering skin oil production, killing acne bacteria, and reducing inflammation.17-19
Expand to read details of studies

A 2013 study in the Indian Journal of Dermatology, Venereology, and Leprology notes, “A variety of light and laser devices has been used for the treatment of acne,” and that these devices appear to work by targeting underlying mechanisms that contribute to acne, such as by eliminating bacteria, reducing skin oil (sebum) production, and reducing inflammation.17

According to a 2013 article in Drug Resistance Updates, blue light has antimicrobial effects that can kill C. acnes (acne bacteria) with fewer side effects than those of ultraviolet light. The authors noted, “Blue light therapy is a clinically accepted approach for Cutibacterium acnes infections.”18

A 2011 study in the Annals of Dermatology demonstrated that photodynamic therapy, a common treatment for acne that involves putting a substance on the skin that increases photosensitivity and then exposing the skin to light, is effective in reducing acne lesions. This study used photodynamic therapy on 12 patients with mild to moderate acne. The authors found a “significant reduction in the number of inflammatory acne lesions after [photodynamic therapy].” They also found a significant decrease in sebum production after 2 weeks and a reduction in the expression of receptors that contribute to inflammation in skin oil glands.19
Potential Side Effects of Sun Exposure
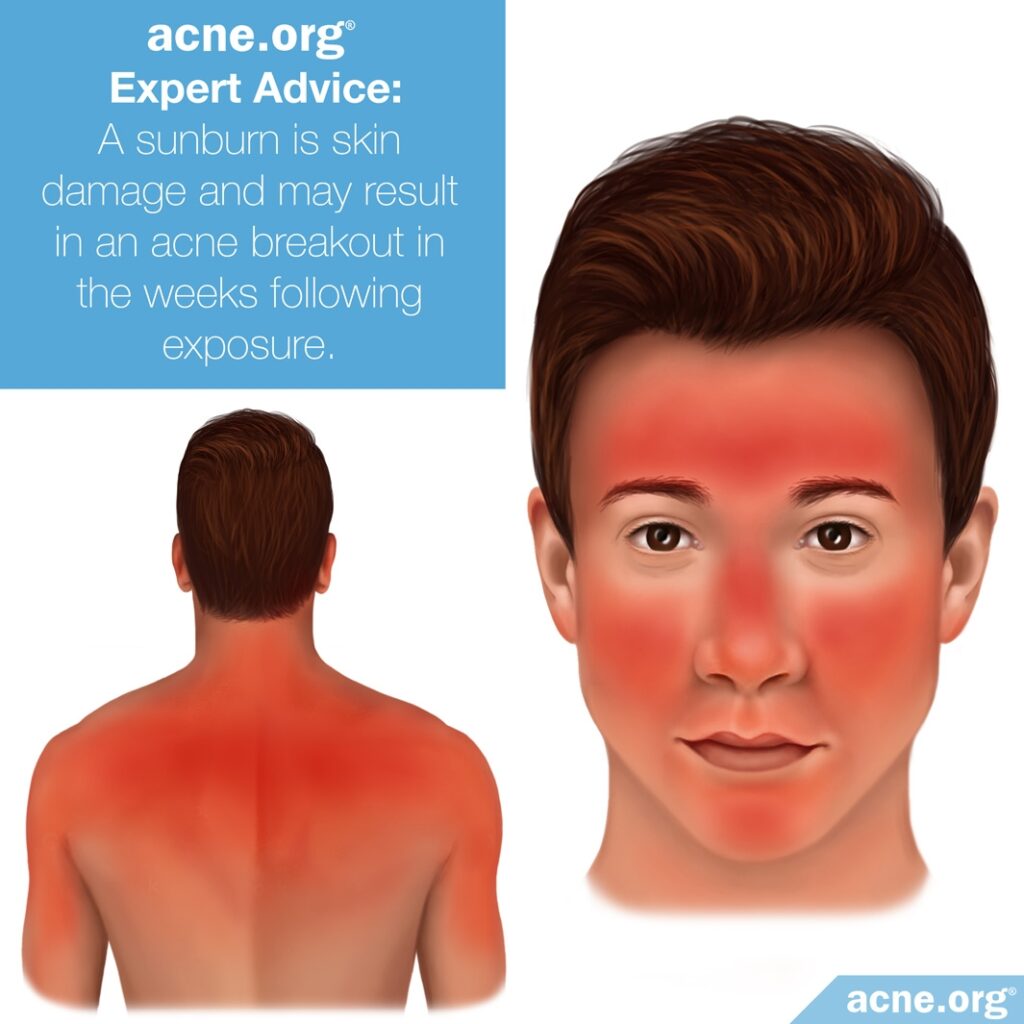
A moderate amount of sun exposure may or may not help reduce acne. A sunburn, on the other hand, is skin damage and will very likely result in a breakout a week or two following the sunburn. To decrease the chance of developing acne, avoid sunburn.
Long-term overexposure to sunlight also results in serious side effects such as increased risk of skin cancers. In addition, commonly used acne medications, such as tetracycline antibiotics and isotretinoin (Accutane), can cause the skin to become more sensitive to the sun: this increases the risk of sunburn and, subsequently, cancer development.1
The Bottom Line
Thus far, research has been unable to positively prove or disprove that sun exposure is effective as an acne treatment.
However, there is evidence of a correlation between low levels of vitamin D and acne, suggesting that sun exposure could help acne for this reason.
Light and laser therapy have also been shown to be at least somewhat effective in reducing acne lesions, so this gives us hope that the sun might provide some benefit.
However, if you choose to get regular sun exposure, be cautious. Too much sun will cause sunburn, which will bite back with acne in the weeks following the sunburn. And too much sun can also cause skin cancer over the long haul.
References
- Magin, P., Pond, D., Smith, W. & Watson, A. A systematic review of the evidence for ‘myths and misconceptions’ in acne management: diet, face-washing and sunlight. Fam. Pract. 22, 62 – 70 (2005). https://www.ncbi.nlm.nih.gov/pubmed/15644386
- Barbaric, J., Abbott, R., Posadzki, P., Car, M., Gunn, L.H., Layton, A.M., Majeed, A. & Car, J. Light therapies for acne. Cochrane Database Syst. Rev. 9, CD007917 (2016). https://www.ncbi.nlm.nih.gov/pubmed/27670126
- Scott, A. M., Stehlik, P., Clark, J., Zhang, D., Yang, Z., Hoffmann, T., Mar, C. D. & Glasziou, P. Blue-light therapy for acne vulgaris: A systematic review and meta-analysis. Ann. Fam. Med. 17, 545-553 (2019). https://www.ncbi.nlm.nih.gov/pubmed/31712293
- Berg, M. Epidemiological studies of the influence of sunlight on the skin. Photodermatol. 6, 80 – 84 (1989). https://www.ncbi.nlm.nih.gov/pubmed/2748434
- Gfesser, M. & Worret, W. I. Seasonal variations in the severity of acne vulgaris. Int. J. Dermatol. 35, 116 – 117 (1996). https://www.ncbi.nlm.nih.gov/pubmed/8850040
- Sardana, K., Sharma, R. C. & Sarkar, R. Seasonal variation in acne vulgaris–myth or reality. J. Dermatol. 29, 484 – 488 (2002). https://www.ncbi.nlm.nih.gov/pubmed/12227481
- Meyer, K. et al. Evaluation of Seasonal Changes in Facial Skin With and Without Acne. J. Drugs. Dermatol. 14, 593 – 601 (2015). https://www.ncbi.nlm.nih.gov/pubmed/26091385
- Pascoe, V. L. & Kimball, A. B. Seasonal variation of acne and psoriasis: A 3-year study using the Physician Global Assessment severity scale. J. Am. Acad. Dermatol. 73, 523 – 525 (2015). https://www.jaad.org/article/S0190-9622(15)01740-5/fulltext
- Pappas, A. et al. Seasonal changes in epidermal ceramides are linked to impaired barrier function in acne patients. Experimental Dermatology 27, 833-836(2018). https://pubmed.ncbi.nlm.nih.gov/29356138/
- Youssef, D. A. et al. Antimicrobial implications of vitamin D. Dermatoendocrinol. 3, 220 – 229 (2011). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3256336/
- Lee, W. J., Choi, Y. H., Sohn, M. Y., Lee, S. J. & Kim, D. W. Expression of Inflammatory Biomarkers from Cultured Sebocytes was Influenced by Treatment with Vitamin D. Indian J. Dermatol. 58, 327 (2013). https://www.ncbi.nlm.nih.gov/pubmed/23919024
- Yildizgoren, M. T. & Togral, A. K. Preliminary evidence for vitamin D deficiency in nodulocystic acne. Dermatoendocrinol. 6, e983687 (2014). https://www.ncbi.nlm.nih.gov/pubmed/26413187
- Lim, S. K., Ha, J. M., Lee, Y. H., Lee, Y., Seo, Y. J., Kim, C. D., Lee, J. H. & Im, M. Comparison of vitamin D levels in patients with and without acne: A case-control study combined with a randomized controlled trial. PLoS One. 11, e0161162 (2016). https://www.ncbi.nlm.nih.gov/pubmed/27560161
- El-Hamd, M. A., El Taieb, M. A., Ibrahim, H. M. & Aly, S. S. Vitamin D levels in acne vulgaris patients treated with oral isotretinoin. J. Cosmet. Dermatol. 18, 16-20 (2019). https://www.ncbi.nlm.nih.gov/pubmed/29460332
- Lucas, R. M., Repacholi, M. H. & McMichael, A. J. Is the current public health message on UV exposure correct? Bull. World Health Organ. 84, 485 – 491 (2006). https://www.ncbi.nlm.nih.gov/pubmed/16799733
- Cancer Council Australia. Risks and benefits of sun exposure: Summary statement. 1 – 7 (2007). https://www.cancer.org.au/policy-and-advocacy/position-statements/sun-smart/
- Rai, R. & Natarajan, K. Laser and light based treatments of acne. Indian J. Dermatol. Venereol. Leprol. 79, 300 – 309 (2013). http://www.ijdvl.com/article.asp?issn=0378-6323;year=2013;volume=79;issue=3;spage=300;epage=309;aulast=Rai
- Dai, T. et al. Blue light for infectious diseases: Propionibacterium acnes, Helicobacter pylori, and beyond? Drug Resist. Updat. 15, 223 – 236 (2012). https://www.ncbi.nlm.nih.gov/pubmed/22846406
- Jeong, E. et al. Topical ALA-Photodynamic Therapy for Acne Can Induce Apoptosis of Sebocytes and Down-regulate Their TLR-2 and TLR-4 Expression. Ann. Dermatol. 23, 23 – 32 (2011). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3119995/
 Acne.org Products
Acne.org Products