Looking at the Research and Possible Links Between Drugs and Acne

The Essential Info
Due to ethical and legal restrictions, researchers have not directly studied the effects of most drugs on acne. This leaves us without the necessary data to draw any firm conclusions on how drugs might affect acne.
However, we do know that most drugs:
- Increase the stress hormone cortisol in the body. Cortisol is the main stress hormone in the body. Since stress can make acne worse, can drugs do the same thing? It’s an interesting question.
And we also know that some drugs (particularly cocaine):
- Increase inflammation in the body. Acne is at its core an inflammatory disease, so it is possible that drugs, especially cocaine, may prove detrimental for acne.
Lastly, one drug in particular, methamphetamines, can lead to:
- Uncontrollable skin picking. This can wreak havoc on the skin, leaving open sores and leading to scarring.
The Bottom Line: Until we have more evidence, no one can say for sure whether various drugs will worsen acne. But suffice it to say that it is extremely unlikely that any drug will improve acne. The safest bet would be not to do drugs.

The Science
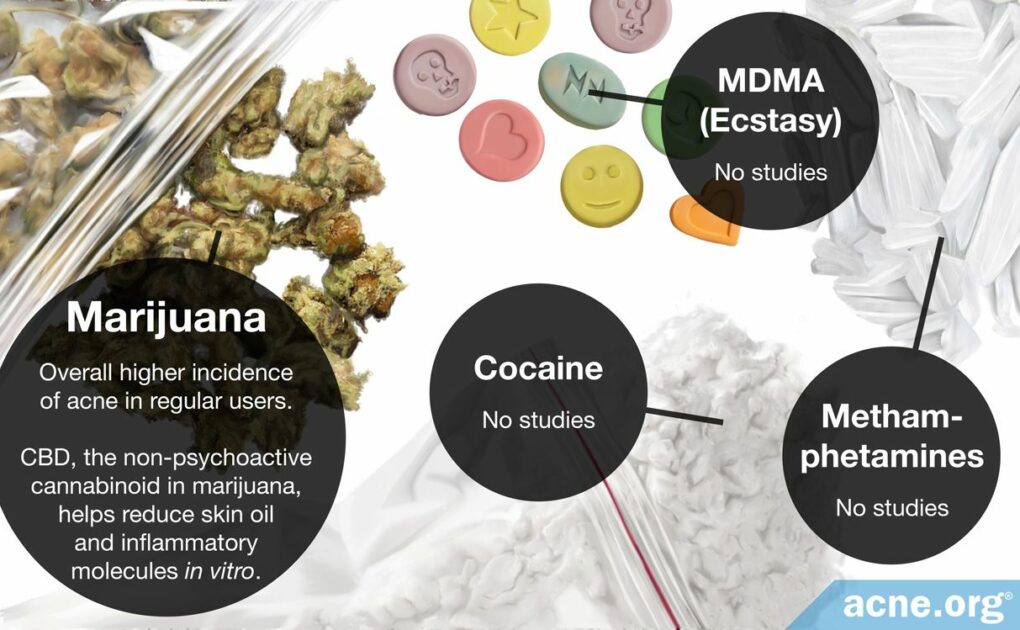
Scientists have performed two recent studies on marijuana and acne, but no research specific to other drugs and their effects on acne exists in any peer-reviewed medical journals.
However, we do have research on how drugs affect some other factors that might give us some clues to how they might affect acne:
- Hormones: Studies attempting to relate cocaine, MDMA (ecstasy), and marijuana with hormone production have come to conflicting conclusions. Acne is a hormonal disease, so if any drug does increase hormones associated with acne, this would be important to note. Research is trickling in on this, but we don’t have enough evidence to draw conclusions yet.
- Cortisol: Marijuana, cocaine, MDMA, and methamphetamines have all been shown to increase cortisol levels. Cortisol is the main stress hormone in the body and has been linked with acne.
- Inflammation: Some drugs, particularly cocaine, stimulate inflammation in the body. Acne is at its core an inflammatory disease, so anything that increases inflammation could theoretically worsen acne.
Let’s look at various drugs one-by-one and see what the research tells us so far.
Marijuana (mixed results from studies – can’t say for sure how it might affect acne)

Studies that have tried to find a link between marijuana use and acne have obtained mixed results. One recent study found that people who regularly use marijuana are more likely to suffer from acne than non-users.1
On the other hand, three lab studies found that one of the components of marijuana suppresses inflammation, which should theoretically reduce acne in marijuana users.2-4 Two of these three studies also found that marijuana may reduce the production of skin oil (sebum), which would also help with acne.2,4 However, it’s important to note that these lab studies are just that–in a lab. They are performed in petri dishes and not on human skin. So, while this is interesting, we should not take this as any sort of concrete evidence that marijuana can reduce acne.
Expand to read details of studies

A study published in the journal Dermatology in 2015 analyzed 10,084 people and concluded that regular marijuana users were more likely to have acne than non-users. On the other hand, participants who used marijuana only occasionally were not more likely than non-users to have acne. The authors concluded: “The regular use of cannabis was associated with acne.”1 Although this study shows that there may be a correlation between regular marijuana use and acne, more research is needed to support this conclusion.

Excess sebum (skin oil) is also associated with acne. Another study, published in 2014 in the Journal of Clinical Investigation showed that CBD, the non-psychoactive cannabinoid in marijuana, may actually help prevent acne through its effects on sebum suppression and reduced inflammation. When researchers exposed skin cells to a CBD solution in a laboratory setting, it slowed down the growth of cells that produce sebum, decreased sebum production, and suppressed the production of inflammatory molecules of these cells.2 It remains to be determined whether using marijuana, which contains many other compounds aside from CBD, would have the same effect on skin cells.

Another laboratory study, published in the journal Phytotherapy Research in 2019, also found that some compounds in marijuana might help with acne. In this study, researchers applied a marijuana extract to human skin cells in the lab. They found that the extract had an anti-inflammatory effect on the skin cells. Since acne is an inflammatory disease, this suggests that marijuana might potentially help reduce acne. The researchers speculated that CBD and possibly other substances in the marijuana may have been responsible for the anti-inflammatory effect. However, it is important to keep in mind that this was a lab study performed on skin cells grown in a petri dish, not on the skin of a person.3

Lastly, a study published in the journal PLOS ONE in 2018 tested the anti-acne potential of marijuana seeds on human skin cells in a petri dish. The researchers reported that marijuana might reduce acne in several ways:
- By exerting an anti-microbial effect on C. acnes, the type of bacteria found in acne lesions
- By reducing inflammation
- By reducing skin oil production4
Marijuana and its psychoactive cannabinoid THC affect multiple hormone (endocrine) systems. Changes in hormone levels, particularly increased male hormone (androgen) levels, can increase acne.
However, human studies investigating the effects of cannabinoids on hormones have been conflicting, with some studies showing lowered levels of androgens, some showing no change, and still others showing increased levels.5,6
Expand to read details of studies

A review study published in 2002 in the Journal of Clinical Pharmacology said: Lower testosterone levels have been reported in chronic marijuana users compared to nonusers and acute decreases in both LH (luteinizing hormone) and testosterone have been observed after marijuana smoking, but multiple subsequent studies have not confirmed these findings. In one study, heavy chronic users were found to have similar testosterone levels compared to casual users at baseline and did not experience any significant alterations in testosterone after a 21-day period of intense marijuana smoking in a controlled research setting. A subsequent study of similar design by the same investigators showed no significant changes in integrated LH levels over the study period. These inconsistent observations may be due to differences in study design but also may reflect the development of tolerance.”5

A more recent study published in 2015 in the American Journal of Epidemiology collected data from 1215 men and found that testosterone levels were slightly higher in marijuana users than non-users. “Serum testosterone, free testosterone, and sex hormone-binding globulin were higher among marijuana users than nonusers…with a level of 7%.”6
In summary, more research is needed before we draw any conclusions on how marijuana affects hormone levels, skin oil (sebum) production, or acne incidence or severity.
Cocaine (might increase inflammation, which could hypothetically worsen acne)

There are no studies that have looked at the direct link between cocaine and acne. However, cocaine can change hormone levels and increase inflammation, which could theoretically result in worsening of acne.
Studies on cocaine show changes in testosterone and estrogen levels in humans and animals during and after administration.6 Whenever we see changes in hormone levels, this is cause for concern when it comes to acne.
More specifically, and more concerningly, human trials have shown increases in a hormone called luteinizing hormone (LH) in both male and female human subjects during cocaine administration.8,9 Luteinizing hormone is a type of hormone called an androgen, which are male hormones present in both males and females. Increased levels of androgens tend to lead to more acne, so this is potential cause for concern when it comes to cocaine’s potential to increase acne.
Animal trials have shown conflicting results. Chronic cocaine use was shown to disrupt the menstrual cycle in female primates.7 How this would potentially affect acne is unknown. In one study on rats, testosterone levels and testes size was markedly lower after four weeks of cocaine use.10 Lower testosterone normally means lower acne symptoms, but this is just one study performed on rats so we cannot draw any conclusions.
Three additional studies in humans have found that cocaine might indirectly increase the amount of the stress hormone cortisol in the body and can also increase inflammation.11-13 Both of these effects of cocaine could theoretically contribute to making acne worse.
Expand to read details of these 3 studies

Cocaine could also hypothetically worsen acne by increasing the amount of ACTH, a hormone that stimulates cortisol release. A 2014 study published in the Journal of Endocrinological Investigation showed an increase in ACTH immediately following intravenous cocaine administration in humans.11

Cocaine use also increases systemic inflammation. A study published in Human Psychopharmacology in 2012 reported, “Current findings show that cocaine dependent individuals demonstrate increased immune system inflammation both at the baseline and in response to stress.”12

In 2022, researchers published a study in the journal Oxford Academic showing elevated levels of human stress hormones in chronic cocaine users. The scientists measured the amounts of stress hormones in human hair and found that chronic cocaine users had significantly higher levels of cortisone and cortisol than recreational users and non-users.13
MDMA “Ecstasy” (might dramatically increase cortisol levels, which could hypothetically worsen acne)

There are no studies that have looked at the direct link between MDMA (ecstasy) and acne. However, some evidence points toward possible changes in male hormone (androgen) and stress hormone levels following MDMA administration in animals and humans. The studies are small and results conflict.
In one study on rats, scientists found lowered amounts of testosterone and also lowered amounts of another reproductive hormone GnRH in rats seven days after administration of ecstasy (MDMA).14 One small human study showed a huge spike in cortisol (800%) during MDMA usage with testosterone also increasing by 75%.15 Another study published in 2014 measured hormone levels in sixteen healthy men and women after administration of MDMA and found that while cortisol levels increased by 166% twenty-four hours after taking MDMA, testosterone levels did not change.16
Since the evidence thus far on MDMA and hormones is mixed, and we cannot extrapolate results from animal studies to humans, we do not know at this point whether MDMA negatively or positively affects androgen production. However, considering that ecstasy may dramatically raise cortisol levels, this could possibly be a concern when it comes to acne development.
Methamphetamines (leads to uncontrollable skin picking, which can worsen acne and cause scarring)

Although anecdotal evidence suggests that methamphetamine users tend to develop acne, no research has been done on this topic. Methamphetamine users are also known to pick at their skin uncontrollably. Picking can cause physical irritation, which can lead to acne development. Picking is also a major contributor to scarring.
A study published in 2010 found that methamphetamines also increase stress in the body, which is linked to acne.17
Expand to read details of study

A study published in the Journal of Neuroimmune Pharmacology in 2010 investigated cortisol levels in adolescents who used methamphetamine. Although the levels of cortisol were the same in users and non-users under normal conditions, when methamphetamine users were exposed to a stressful situation, their cortisol levels rose much higher than in non-users. This study shows that methamphetamine exaggerates the response to stress.17
Another study found that methamphetamine slows down wound healing. Since acne lesions are small wounds, this suggests that acne lesions might take longer to heal in methamphetamine users.
In addition, this study found that methamphetamine reduces the ability of the immune system to fight certain bacteria. Since bacteria can also worsen acne, this might mean that people who use methamphetamine are more likely to develop acne.18 However, these are only speculations at this point.
Expand to read details of study

The study was published in the microbiology journal mBio in 2015. The researchers tested methamphetamine on mice with skin wounds, and found that the methamphetamine slowed down wound healing.18
In addition, the scientists tested how methamphetamine affected the ability of immune cells from both mice and humans to fight bacteria in the lab. They looked specifically at a type of bacteria called Staphylococcus aureus because this type of bacteria frequently causes an infection in methamphetamine users. The researchers found that methamphetamine decreased the ability of immune cells to fight this type of bacteria.18 This suggests that methamphetamine might also decrease the body’s ability to fight other types of bacteria, such as C. acnes, which can worsen acne. However, we do not have any direct evidence for this idea.
Other Considerations Regarding Drugs and Acne

Stress: Drug use can cause both mental and physical stress, and stress is intimately connected with acne symptoms in many people.19 Overuse of drugs can lead to paranoia, anxiety, and depression. Drug use can also put stress on the body. Bodily stress is an often overlooked factor in acne formation.
Missing Your Daily Regimen: Drug binges can sometimes lead to missing one’s daily skin care regimen. Consistent application of a properly applied regimen is required to completely clear acne.
Irritation: Some drugs, especially methamphetamines, can lead to the uncontrollable need to pick at one’s skin. Picking, or any irritation for that matter, is one of the biggest factors in acne development, and should not be underestimated.
References
- Wolkenstein, P. et al. Smoking and dietary factors associated with moderate-to-severe acne in French adolescents and young adults: results of a survey using a representative sample. Dermatology 230, 34 – 39 (2015). https://www.ncbi.nlm.nih.gov/pubmed/25413494
- Olah, A. et al. Cannabidiol exerts sebostatic and antiinflammatory effects on human sebocytes. J. Clin. Invest. 124, 3713 – 3724 (2014). https://www.ncbi.nlm.nih.gov/pubmed/25061872
- Sangiovanni, E., Fumagalli, M., Pacchetti, B., Piazza, S., Magnavacca, A., Khalilpour, S., Melzi, G., Martinelli, G. & Dell’Agli, M. Cannabis sativa L. extract and cannabidiol inhibit in vitro mediators of skin inflammation and wound injury. Phytother. Res. 33, 2083-2093 (2019). https://www.ncbi.nlm.nih.gov/pubmed/31250491
- Jin, S. & Lee, M.-Y.. The ameliorative effect of hemp seed hexane extracts on the Propionibacterium acnes-induced inflammation and lipogenesis in sebocytes. PLOS ONE 13, 1-19 (2018). https://pubmed.ncbi.nlm.nih.gov/30148860/
- Brown, T. T. & Dobs, A. S. Endocrine effects of marijuana. J. Clin. Pharmacol. 42, 90S – 96S (2002). https://www.ncbi.nlm.nih.gov/pubmed/12412841
- Gundersen, T. D. et al. Association Between Use of Marijuana and Male Reproductive Hormones and Semen Quality: A Study Among 1,215 Healthy Young Men. Am. J. Epidemiol. 182, 473 – 481 (2015). https://www.ncbi.nlm.nih.gov/pubmed/26283092
- Mello, N. K. et al. The effects of cocaine on gonadal steroid hormones and LH in male and female rhesus monkeys. Neuropsychopharmacology 29, 2024 – 2034 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15199372
- Mendelson, J. H. et al. Effects of intravenous cocaine and cigarette smoking on luteinizing hormone, testosterone, and prolactin in men. J. Pharmacol. Exp. Ther. 307, 339 – 348 (2003). https://www.ncbi.nlm.nih.gov/pubmed/12893845
- Mendelson, J. H., Sholar, M. B., Siegel, A. J. & Mello, N. K. Effects of cocaine on luteinizing hormone in women during the follicular and luteal phases of the menstrual cycle and in men. J. Pharmacol. Exp. Ther. 296, 972 – 979 (2001). https://www.ncbi.nlm.nih.gov/pubmed/11181931
- Jia, X. D., Zhou, D. X. & Song, T. B. [The reproductive system impairment of adult male rats induced by cocaine]. Fa Yi Xue Za Zhi 24, 411 – 413 (2008). https://ijpsr.com/bft-article/male-infertility-causes-and-contributors/?view=fulltext
- Manetti, L., Cavagnini, F., Martino, E. & Ambrogio, A. Effects of cocaine on the hypothalamic-pituitary-adrenal axis. J. Endocrinol. Invest. 37, 701 – 708 (2014). https://www.ncbi.nlm.nih.gov/pubmed/24852417
- Fox, H. C. et al. Immune system inflammation in cocaine dependent individuals: implications for medications development. Hum. Psychopharmacol. 27, 156-166 (2012). https://www.ncbi.nlm.nih.gov/pubmed/22389080
- Voegel, C.D. et al. Alterations of stress-related glucocorticoids and endocannabinoids in hair of chronic cocaine users. The International Journal of Neuropsychopharmacology 25, 226-237 (2022). https://pubmed.ncbi.nlm.nih.gov/34676867/
- Dickerson, S. M., Walker, D. M., Reveron, M. E., Duvauchelle, C. L. & Gore, A. C. The recreational drug ecstasy disrupts the hypothalamic-pituitary-gonadal reproductive axis in adult male rats. Neuroendocrinology 88, 95 – 102 (2008). https://www.ncbi.nlm.nih.gov/pubmed/18309234/
- Parrott, A. C., Lock, J., Conner, A. C., Kissling, C. & Thome, J. Dance clubbing on MDMA and during abstinence from Ecstasy/MDMA: prospective neuroendocrine and psychobiological changes. Neuropsychobiology 57, 165 – 180 (2008). https://www.ncbi.nlm.nih.gov/pubmed/18654086
- Seibert, J. et al. Acute effects of 3,4-methylenedioxymethamphetamine and methylphenidate on circulating steroid levels in healthy subjects. Neuroendocrinology 100, 17 – 25 (2014). https://www.ncbi.nlm.nih.gov/pubmed/24903002
- King, G., Alicata, D., Cloak, C. & Chang, L. Psychiatric symptoms and HPA axis function in adolescent methamphetamine users. J. Neuroimmune Pharmacol. 5, 582 – 591 (2010). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2974768/
- Mihu, M. R., Roman-Sosa, J., Varshney, A. K., Eugenin, E. A., Shah, B. P., Ham Lee, H., Nguyen, L. N., Guimaraes, A. J., Fries, B. C., Nosanchuk, J. D. & Martinez, L. R. Methamphetamine alters the antimicrobial efficacy of phagocytic cells during methicillin-resistant Staphylococcus aureus skin infection. mBio. 6, e01622-15 (2015). https://mbio.asm.org/content/6/6/e01622-15
- Alexopoulos, A. & Chrousos, G. P. Stress-related skin disorders. Rev. Endocr. Metab. Disord. 17, 295-304 (2016). https://www.ncbi.nlm.nih.gov/pubmed/27368716
 Acne.org Products
Acne.org Products