Yes, and It Is Such a Well-Known Problem that It Has Its Own Medical Term: Acne Mechanica

The Essential Info
Physical irritation of the skin refers to anything that repeatedly touches or rubs against the skin. This physical irritation can lead to acne. In fact, it is such a common phenomenon that dermatologists refer to it with the term acne mechanica.
If the irritation goes on for a longer time or if the irritation is more intense, more severe acne can result.
Physical irritation mixed with sweat can make matters even worse.
Some common examples of physical irritation:
- COVID-19 masks
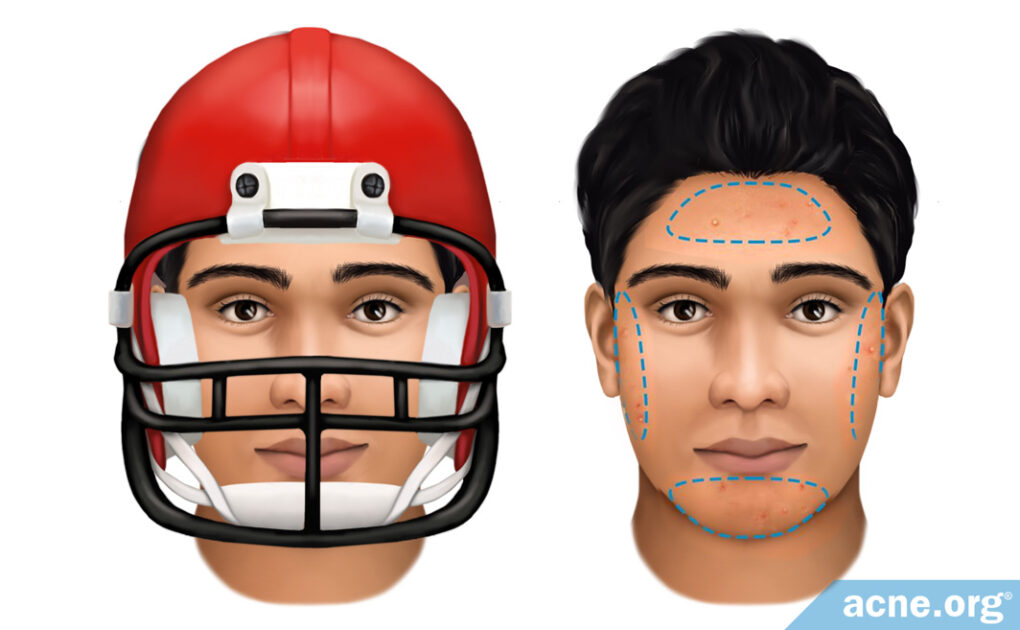
- Face masks for sports
- Tight hats
- Constantly touching/picking the skin
- Washcloths
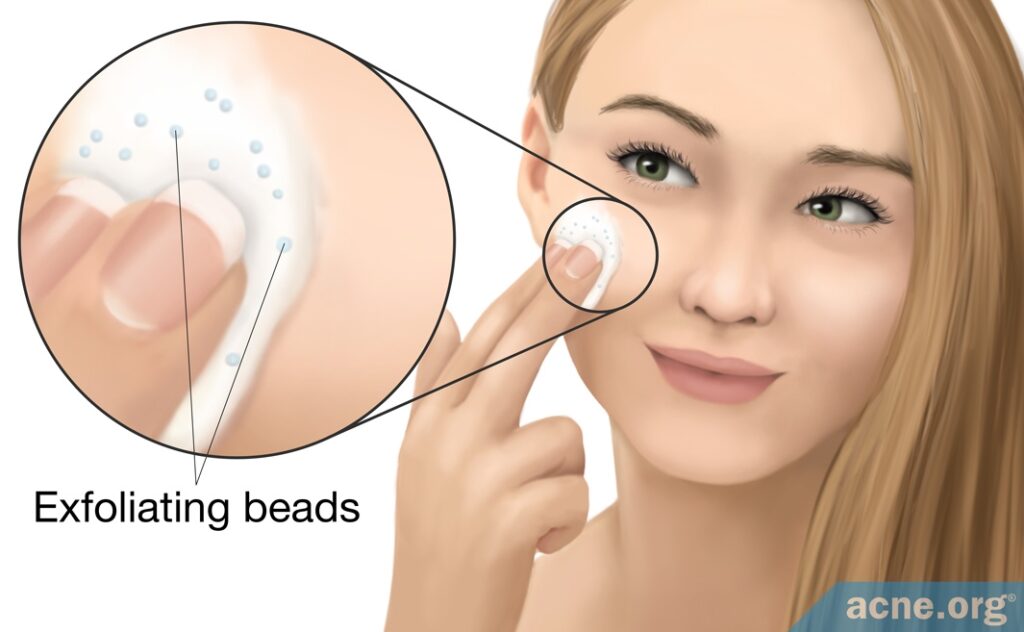
- Exfoliating cleansers
- Backpack/Purse straps
What can be done about it:
- Don’t stress out about it too much, but try to leave acne-prone skin relatively untouched when you can.
- Wash your face gently. That means using only your bare hands and washing for 10 seconds or less using a featherlight touch.
- Treat acne-prone areas with a proper daily regimen to keep acne at bay, and if you happen to overly irritate any area, be sure to apply 10% glycolic acid to that area as insurance against a breakout.

The Science
- How Acne Mechanica Was Discovered
- Occupational Acne – Another Term for Acne Mechanica
- What Can Be Done About It?
Since the 1970s, researchers have published studies showing that acne can be aggravated by physical irritation. These researchers introduced the concept of acne mechanica to describe this phenomenon.
Today, dermatologists accept the reality of acne mechanica and recognize that friction, tension, rubbing, and persistent pressure can aggravate existing acne and can also induce acne on healthy skin.
Some common things that can cause acne mechanica include:
- Wearing a COVID-19 mask
- Wearing a facemask for a sport
- Wearing tight hats that rub against the forehead
- Constantly touching the face or resting your chin in your hands
- Picking at acne lesions
- Scrubbing with a washcloth or cleansing brush instead of gently washing with bare hands
- Getting a close “buzz” haircut with clippers when the hairdresser is not gentle
- Using “exfoliating” skin care products that contain irritating beads or seeds
- Backpack straps / purse straps
So, as you can see, any repetitive physical irritation of the skin can potentially make acne worse. This is true on the skin of the face and the body.
Since it is impossible to completely avoid any irritation, don’t stress out about this too much. Instead, just become aware of obvious and avoidable sources of irritation, and eliminate them when you can.
How Acne Mechanica Was Discovered

The researchers, Mills and Klingman, introduced acne mechanica in a study they published in the journal Archives of Dermatology in 1975. They wanted to emphasize that any type of mechanical stress of the skin can intensify the symptoms of acne, so they devised a method to demonstrate that physical pressure can aggravate acne. These researchers simulated the effect of physical pressure by placing cloth-backed adhesive tape on the skin of ten teenage volunteers with moderately severe facial and back acne. They placed the tape on the skin over the shoulder blade in areas where the acne was less severe so they could see how mild acne symptoms were affected by the physical irritation of the tape. They removed the tape after a week to evaluate skin changes and then applied an identical piece of tape for another week. After one week the number of inflamed lesions increased in five of the subjects. After two weeks the number of inflamed lesions increased in seven of the subjects, with new pimples appearing on the skin where the irritating tape had been placed. The researchers also took biopsy samples that showed typical features of acne, such as inflammation of pores and the surrounding skin, after two weeks. This proved their point that acne can be aggravated by physical irritation. Clogged pores that had not been inflamed became inflamed after taping, indicating that the mechanical action of the tape on the skin worsened the acne.1
Since acne mechanica was first introduced in 1975, other researchers reported on more examples of acne mechanica in case studies. A case study is published when doctors notice something in just one or a few people and report it. It is interesting to see how real people experience acne mechanica as the result of such varied physical irritants.
One case study reported on three females who developed acne mechanica after rubbing their skin with cosmetic agents.2
Expand to read details of case study

A 2012 case study reported in the journal Dermatology described three cases of acne induced by friction when the patients rubbed their skin with cosmetic agents. In one of these cases, a girl (age 19) had numerous pustules on her left cheek that merged into large plaques (scaly, red, bumpy areas). The disease developed after she rubbed a prescription skin-repair cream on her cheek twice a day to treat damage from surgery. The symptoms in the other two study-cases were similar to those in the first one. One girl (age 17) rubbed her skin once a day with an exfoliative cream containing nutshell seeds, and the other girl (age 15) “rubbed vigorously” once a day with a product to reduce pain in her jaw. None of the three girls had a previous history of severe acne, and the substances they used did not have a history of inducing acne. These factors led the researchers to classify these cases as acne mechanica since there seemed to be no other cause.2
Another case study described three female dental patients and nine male orthopedic patients. These patients developed acne mechanica in locations where their skin was in constant contact with a dental splint or bed during their treatment.3
Expand to read details of case study

Another case study, published in 1976 in the British Medical Journal, described three dental patients (all female, ages 17, 19, and 24) and nine orthopedic patients (all male, ages 18 – 39) who developed acne as a side effect of their treatments. The dental patients developed acne around the mouth three to six weeks after surgeons placed corrective splints on their jaws. The orthopedic patients were confined to bed rest, on their backs for most of the time, for three to six months while waiting for surgery and developed acne on their backs. All 12 patients had minimal or no acne anywhere else on their bodies. One of the factors for this is that sebum (skin oil) was trapped in the skin pores because of the contact with the dental splint or bed. The extra sebum could have increased the onset of clogged pores and acne. The other factor is increased sweating on the back. While sweat normally is not a factor in acne development, it may add water to the keratin (a protein) in the skin when trapped inside clothing for extended periods, making it more likely to block skin pores. Once the pore is clogged with keratin, sebum cannot escape onto the skin surface; the pore becomes enlarged, and the oxygen level inside the pore decreases. This creates ideal conditions for bacteria inside the pore to proliferate, causing irritation, inflammation, and ultimately, acne.3
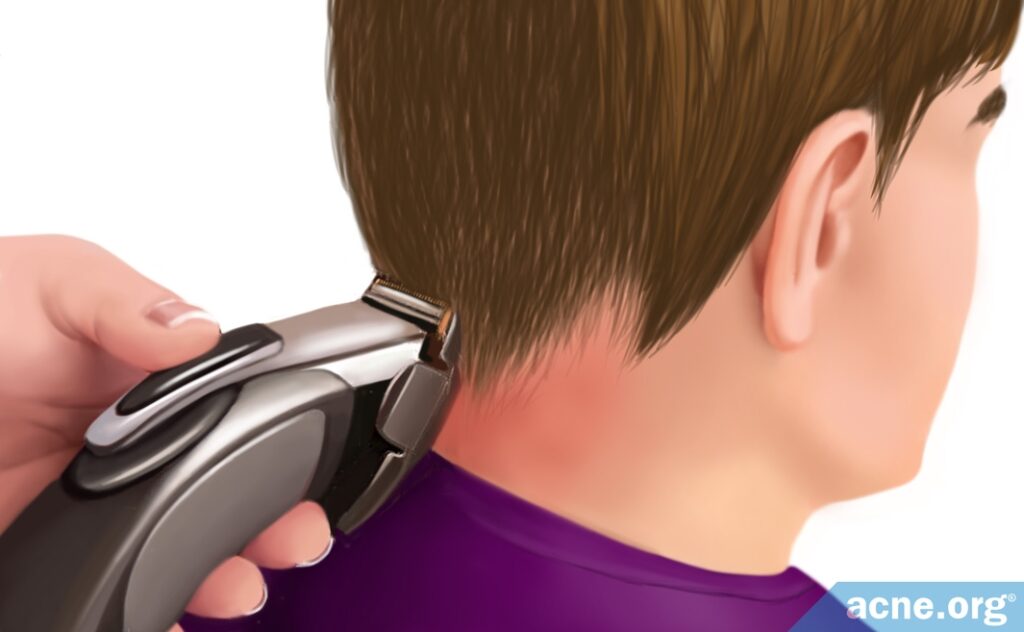
A third case study described 27 patients who believed their severe acne began due to trauma of the skin by a razor during a haircut.4
Expand to read details of case study

Another 2007 case study published in the International Journal of Dermatology reported on 27 patients who had believed that their acne began with a haircut. These patients had a severe form of acne called acne keloidalis nuchae (AKN), which is chronic inflammation of hair follicles on the back of the neck with fibrous plaques and papules (small raised solid pimples). AKN occurs mostly in young African-American males. Trauma of the skin by a razor appears to be a common factor in AKN. As the razor is used, the cutting edge becomes dull, and more force must be used to give a close shave, damaging the skin. The resulting physical irritation appears to cause this particular form of acne to develop.4
Occupational Acne – Another Term for Acne Mechanica

Occupational acne is acne mechanica that is caused by a person’s job or some other activity they regularly participate in. Since acne mechanica is associated with repetitive physical contact, it is common in athletes, especially in football players. In addition to the heat and friction caused by contact sports, heavy protective equipment, such as that worn by football players, can cause eruptions of acne on the shoulders, upper back, back of the head, and chin. All of these areas receive high levels of pressure from the protective pads, helmets, and facemasks.5
Acne mechanica in football players: Researchers made the connection between football equipment and acne mechanica in a 1997 study published in the Journal of the American Academy of Dermatology, in which they examined 453 football players for acne.6
Expand to read details of study

The researchers examined football players with a type of acne called nuchal acne, which is acne that occurs on the nape (back) of the neck, and AKN. They examined 453 football players ranging from high school age to professional, adult age and found 64 of them (14.1%) had one or the other of these forms of acne. Nuchal acne without AKN was considerably higher in the high school age players: 15.5% compared to 1.2%. This was attributed to the younger age of the high school players, their poorer personal hygiene, and a greater tendency to share equipment among players. On the other hand, AKN was markedly higher among the college and pro-level players when compared to the high school players: 9.4% of the college and pro-level players had AKN, while only 5.2% of the younger players had AKN. Researchers hypothesized that older players had a longer lifetime exposure to the irritating effects of protective helmets. There was other evidence to back up this idea that football equipment causes acne. Acne on the back of the neck was not seen in preseason practice, when protective equipment was not yet worn, but was seen soon after they began to use the equipment. The acne improved once the season had ended, when the players stopped wearing the equipment.6

Acne mechanica in violin and viola players: Another example of occupational acne is fiddler’s neck, which is seen in a quite different group of people: violin and viola players. These musicians play their instrument while holding it under the left side of their chin. A study published in 1978 described fiddler’s neck in 23 violin and viola players and concluded that this condition was an example of acne mechanica.7
Expand to read details of study

Researchers published a study in 1978 in the British Journal of Dermatology, describing their findings on 23 subjects (14 male, 9 female) with fiddler’s neck. The most common symptoms were thickened skin with exaggerated skin markings (in 82% of subjects) and inflammatory pimples (in 91%) on the left side of the neck. Other symptoms included redness, pustules, and hardening of the skin. The researchers highlighted several factors that contribute to the condition:
- Long duration of play with many hours of daily practice
- Increased pressure of the instrument on the neck due to tiredness or poor grip
- Greater friction between the instrument and the skin due to poor technique
- Poor hygiene
The researchers decided that fiddler’s neck is an example of acne mechanica because it was caused by the physical irritation of the violin or viola on the skin.7 It is an example of occupational acne, specifically, because some of the musicians were professionals and played their instruments frequently.
Acne mechanica in medical professionals: During the COVID-19 pandemic, a new form of occupational acne mechanica emerged, nicknamed “maskne.” Maskne results from wearing a face mask regularly for an extended period of time, so it typically occurs in medical professionals. The mask causes physical irritation by pressing on and rubbing against the skin of the face.8
Acne Mechanica Due to Friction Between Skin Surfaces
It turns out that acne mechanica can even result from two different skin surfaces rubbing against each other. For example, one case report described a teen girl who developed acne on her inner thighs in the summer when the skin of her thighs rubbed together.
Expand to read details of case report

This case study was published in the journal Pediatric Dermatology in 2019. A 17-year-old African American female who was obese visited a dermatologist for her facial acne. During the visit, she also complained of blackheads on her inner thighs. She explained that these acne lesions appeared during the summer when she wore shorts or dresses that allowed her legs to rub against each other. The researchers wrote, “Previous reported causes of acne mechanica have all been external factors such as clothing. This patient’s presentation is unique because the lesions are caused by friction between [skin] surfaces.”9
What Can Be Done About It?
As we can see, life can present us with physical irritation of the skin in many ways. While it is impossible to completely avoid physical irritation, it is nevertheless a good idea to pay attention to anything that might be repeatedly irritating your skin. If you can reduce the irritation, do so. For instance, stop using exfoliating scrubs, wash your face with only your bare hands and not with a washcloth or cleansing brush, and whatever you do, DO NOT PICK at your skin. If you cannot reduce the irritation – for instance, if you have to continue wearing a facemask for a sport – make sure to perform your daily anti-acne regimen carefully in that area to combat the irritation.
Tip: While the best defense against physical irritation is an effective daily anti-acne regimen, additional application of glycolic acid to physically-irritated areas of your skin can provide even more insurance against breakouts when that area has been irritated.
References
- Mills, O. & Kligman, A. Acne mechanica. Arch. Dermatol. 111, 481 – 483 (1975). https://www.ncbi.nlm.nih.gov/pubmed/123732
- Seneschal, E. et al. Exogenous inflammatory acne due to combined application of cosmetic and facial rubbing. Dermatology 224, 221 – 223 (2012). https://www.ncbi.nlm.nih.gov/pubmed/22653048
- Tan, S. et al. Acne mechanica. Brit. Med. J. 1, 130 (1976). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5986265/
- Salami, T., Omeife, H. & Samuel, S. Prevalence of acne keloidalis nuchae in Nigerians. Int. J. Dermatol. 46, 482 – 484 (2007). https://www.ncbi.nlm.nih.gov/pubmed/17472675
- Basler, R. S., Hunzeker, C. M. & Garcia, M. A. Athletic skin injuries: combating pressure and friction. Phys. Sportsmed. 32, 33 – 40 (2004). https://www.ncbi.nlm.nih.gov/pubmed/20086411
- Knable, A. L. Jr., Hanke, C. W. & Gonin, R. Prevalence of acne keloidalis nuchae infootball players. J. Am. Acad. Dermatol. 37, 570 – 574 (1997). https://www.ncbi.nlm.nih.gov/pubmed/9344195
- Peachey, R. D. & Matthews, C. N. Fiddler’s neck. Brit. J. Dermatol. 98, 669-674 (1978). https://www.ncbi.nlm.nih.gov/pubmed/150281
- Teo, W. L. The “Maskne” microbiome – pathophysiology and therapeutics. Int. J. Dermatol. 60, 799-809 (2021). https://pubmed.ncbi.nlm.nih.gov/33576511/
- Mazhar, M., Simpson, M. & Marathe, K. Inner thigh friction as a cause of acne mechanica. Pediatr. Dermatol. 36, 546-547 (2019). https://www.ncbi.nlm.nih.gov/pubmed/30883890
 Acne.org Products
Acne.org Products