Overweight or Obese Females May Be More Likely to Develop Acne, but the Evidence for Males Remains Contradictory

The Essential Info
Females: Studies are contradictory on whether overweight or obese females are more likely to develop acne, and more studies must be performed before we reach a scientific consensus. In other words, we really don’t know yet. However, being overweight may cause a hormonal imbalance, and hormonal imbalances can lead to acne. It’s also important to note that acne in overweight females may also be a symptom of a hormonal disease, such as polycystic ovary syndrome (PCOS). If you are an overweight female with acne, particularly if you have noticed excess hair growth or irregular periods, be sure to speak with your doctor about the possibility of PCOS.
Males: When it comes to males, most of the evidence so far points toward weight not being a factor in acne, but some evidence is contradictory, so we also can’t say for sure.

The Science
- How Do You Know Whether You Are Overweight or Obese?
- Is There a Link Between Being Overweight or Obese and Having Acne?
- Why Might Overweight or Obese People Have More Acne?
- Conclusion
How Do You Know Whether You Are Overweight or Obese?
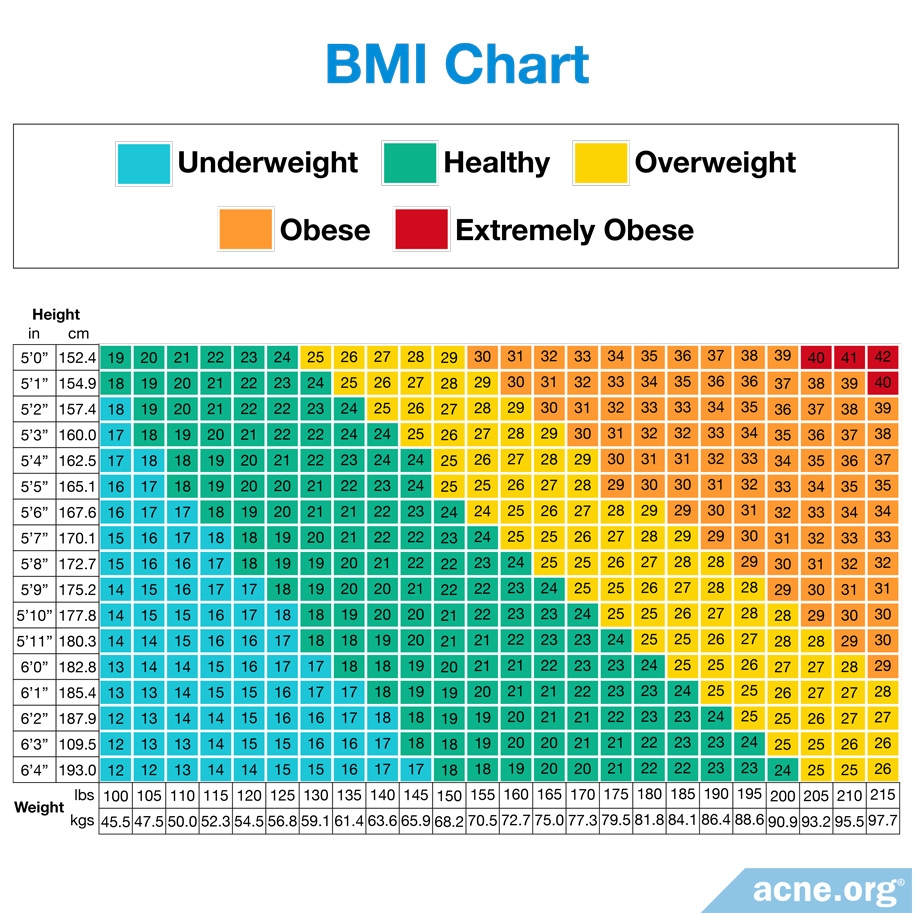
To determine whether a person is underweight, at a healthy weight, overweight, or obese, health professionals use a measure called the body mass index (BMI). BMI is calculated the same way for all ages and genders. To calculate your BMI, follow these steps:
- Determine your height in inches. For example, if your height is 5’6″, then you are 66 inches tall
- Multiply this number by itself. For example, 66*66 = 4356
- Take your weight in pounds and divide by the number you calculated in step two. For example, if you weigh 170 lb, you would divide 170 by 4356, which equals 0.039
- Finally, multiply the number you got in step three by 703. For example, 0.039*703 = 27.4
The final number in step four is your BMI. According to the World Health Organization, if you are at least 20 years old, you are:
- Underweight if your BMI is 18.49 or lower
- At a healthy weight if your BMI is between 18.5 and 24.99
- Overweight if your BMI is 25 or higher
- Obese if your BMI is 30 or higher1
People younger than 20 years should look up healthy BMIs with respect to their age in the charts on the World Health Organization website to determine whether they are underweight, at a healthy weight, overweight, or obese.1
Is There a Link Between Being Overweight or Obese and Having Acne?
Eleven studies have directly investigated whether being overweight or obese increases a person’s likelihood of developing acne and/or of his acne worsening.2-12 The studies, performed around the world, have come to contradictory findings.
Males
On the whole, for males, the preponderance of the evidence seems to point to no connection between excess weight and acne. Here are the conclusions reached by the 10 studies that looked at males:
- 2 studies found that being overweight or obese might lead to acne in males.3,12
- 1 study concluded that while being overweight or obese may not lead to acne in males, if a male already has acne, being overweight or obese might increase the chances that his acne will be more severe.6
- 6 studies found that being overweight or obese has no impact on acne in males.2,4,7,8,10,11
- 1 study concluded that being overweight or obese might actually protect young men from developing acne. However, the researchers did not recommend gaining weight to improve acne.9
Females
For females, most of the findings suggest there may be a connection between excess weight and acne. In other words, for females, being overweight or obese may make acne more likely to develop and/or more severe. Here are the conclusions reached by the 9 studies that looked at females:
- 4 studies found that being overweight or obese might lead to acne in females.3-5,12 However, 1 of these 4 studies found that the connection between excess weight and acne in females was relatively weak.3
- 2 studies concluded that if a female already has acne, being overweight or obese might increase the chances that her acne will be more severe.5,6
- 3 studies found that being overweight or obese has no impact on acne in females.7,10,11
- 1 study concluded that being overweight or obese might protect young women from developing acne. Again, the researchers did not suggest putting on extra weight in hopes of improving acne.9
Expand the section below if you are curious to get all the details of these studies.
Expand to read details of studies

The first study which tried to find a link between weight and acne was published in 1956 in the British Medical Journal. The study examined 2720 male soldiers between the ages of 15 and 45 years. The researchers did not find a clear link between weight and acne in the soldiers and wrote, “We find no simple relation between any grade of acne and weight at any age…”2

A more recent study, which was published in 2012 in the Journal of the American Academy of Dermatology, also looked at BMI and several other risk factors for acne. The study was conducted at a skin disease clinic in Southern Italy and examined 205 people with acne and 358 people without acne, all of whom were 12 – 24 years old. The researchers found that people with a higher BMI were more likely to have acne. They noted that the link between BMI and acne was stronger in males than in females. This means that knowing a girl’s or woman’s BMI would only be slightly helpful in predicting whether she would develop acne, but knowing a boy’s or man’s BMI would be more helpful in predicting whether he would develop it.3

Another study, published in 2012 in the journal Archives of Dermatology, was carried out in Norway and examined 4744 teens between the ages of 18 and 19 years. The researchers found a link between BMI and acne in girls, but not in boys. However, despite this link in teen girls, the researchers were not comfortable with concluding that being overweight causes acne. One reason for this was that the study was based on questionnaires which the teens filled out themselves, so the researchers did not check whether the information they gave was correct. Additionally, the study only looked at the teens at one specific point in time. In order to show that being overweight causes acne, the researchers would ideally study teens who were of healthy weight, observe them over time, and determine whether those who gained weight ended up developing acne. Because of these limitations, the authors of the study wrote, “Despite the findings demonstrating a relationship between acne and overweight and obesity in girls aged 18 and 19 years, the study limitations do not allow the straightforward interpretation that obesity causes acne.”4

Another study, which was published in 2014 in the Saudi Medical Journal, studied Turkish females between the ages of 13 and 42 years. Of these females, 141 had acne and were assigned to group 1, while 73 females did not have acne and were assigned to group 2. The researchers then calculated each girl’s or woman’s BMI and determined whether she was of healthy weight, overweight, or obese. They found that group 1, the group with acne, comprised more overweight and obese females than group 2. They concluded that the higher a girl’s or woman’s BMI is, the more likely she is to develop acne. The researchers further divided just the females with acne into 2 subgroups: subgroup 1 contained females with mild acne, and subgroup 2 contained females with severe acne. They compared the BMI of the females in the 2 subgroups and found that the severe acne group possessed a higher average BMI than the mild acne group. The authors therefore added to their conclusion that not only is a female with a higher BMI more likely to develop acne, but also more likely to suffer from severe acne with a higher BMI. They wrote, “There was a positive correlation between body mass index (BMI) value and the severity of acne.”5

A more recent study, published in 2019 in the journal Acta Dermatovenerologica Croatica, looked at Polish adolescents between the ages of 12 and 18. The researchers examined 85 males and 58 females from a school in Poland. The scientists found no connection between BMI and the likelihood of having acne. In other words, teens of different BMI were equally likely to suffer from acne.
However, the researchers did find a correlation between BMI and the severity of acne for both males and females. Overweight or obese teenagers were more likely to suffer from inflammatory acne compared to underweight teenagers or those of healthy weight. In addition, the presence of shoulder or back acne tended to go hand-in-hand with higher BMI. In other words, this study suggests that being overweight or obese will not give you acne, but if you already have acne, being overweight or obese might make your acne more severe.
The researchers concluded that BMI may be linked to acne severity, but since this was a relatively small study, they noted that further studies are needed to confirm these results. They wrote, “Due to the rather small number of analyzed teenagers, our observations must be taken with caution.”6

Another study, published in 2018 in the Nepal Journal of Dermatology, Venereology & Leprology, looked at 249 acne patients who visited a clinic in Nepal to see whether there was a connection between BMI and acne severity. Most of the patients were between the ages of 11 and 20 and included 145 males and 104 females. The researchers found no link between the patients’ BMI and the severity of their acne.7

Yet another study, published in 2018 in the West Indian Medical Journal, examined 105 male university students in Nigeria. The average age of the students was 22 years. The researchers found no relationship between BMI and acne.8

The next study, published in 2019 in the Journal of the American Academy of Dermatology, looked at 600,404 young people completing their military service in Israel. Half of the study participants were male and half were female, with an average age of 19 years. Surprisingly, the researchers found an inverse relationship between BMI and acne. In other words, young people who were overweight or obese were less likely to have acne than people of healthy weight.
The researchers speculated that excess body fat might protect people from developing acne by converting some male hormones (androgens) into female hormones (estrogens). Androgens, which are found in both males and females, tend to make acne worse, while estrogens tend to improve acne. However, like the previous studies, this study could not prove that a particular BMI causes acne, nor did the researchers recommend gaining weight in order to reduce acne. The study authors wrote, “Further studies including important variables in the obesity-acne relationship are needed to validate our findings.”9
Study #9

A study published in 2021 in the Journal of the Pakistan Medical Association also investigated the impact of BMI on acne severity. The researchers examined 98 acne patients, 27 males and 71 females, at Mayo Hospital in Pakistan. The average age of the patients was 22 years. No link was found between the patients’ BMI and the severity of their acne.10
Study #10

Similarly, a study published in 2022 in the journal Cureus looked for a link between BMI and acne in 596 participants. Approximately half of the participants were male and approximately half were female, and the majority of the participants were 18 to 23 years old. The researchers divided participants into 2 nearly equal groups: those with acne and those without acne, and calculated their BMI. They found that there was no significant difference in BMI between the 2 groups.11
Study #11

Finally, a study published in 2023 in the journal Pediatric Dermatology looked for a possible connection between BMI and acne in 643 acne patients between the ages of 7 and 12 years old. The scientists found that children and pre-teens who had a higher BMI were more likely to have a prescription for an acne medication, suggesting that excess weight might be linked to having acne in this age group. The researchers wrote, “Preadolescents with acne are more likely to be obese than those without acne.”12

It is important to note that even in females, the 5 studies that found a connection between high BMI and acne did not show that being overweight causes acne. They instead showed a correlation: in other words, they showed that females who are overweight tend to suffer from acne. Another example of a correlation would be noticing that on the days when people carry umbrellas, there are usually puddles on the ground. Of course, the umbrellas didn’t cause the puddles. Instead, both the umbrellas and the puddles are due to another factor – rain. In the same way, it is possible that another factor causes some people both to develop acne and to be overweight.
To show that excess weight actually causes acne, researchers would have to take people of healthy weight and without acne and randomly subdivide them into 2 groups: an experimental group and a control group. The people in the experimental group would need to gain weight, while the people in the control group would need to stay at the same weight. The researchers would then compare the number of people with acne in the 2 groups. If the people in the experimental group had more acne than those in the control group, then being overweight most likely causes acne. Until a study like this is performed, we cannot be confident that weight is the cause of acne in overweight or obese people. Rather, another factor may cause both excessive weight and acne.
Why Might Overweight or Obese People Have More Acne?

Hormonal Imbalances
An overproduction of male hormones, called androgens, which are present in both males and females), are one of the top causes of acne in both males and females.
Being overweight or obese can cause an increase in androgens. Here’s how:
- In some people, excess weight causes insulin resistance. Insulin is a hormone which is necessary for our body’s cells to obtain energy from the food we eat. When excess weight causes a person to become insulin resistant, the cells of the body stop responding normally to insulin.
- The body reacts by producing more insulin, which, in turn, can cause the person to gain even more weight.13
- Because insulin is a “master hormone,” which controls other hormones, when more insulin is produced, more androgens are produced.
- Androgens directly control sebum (skin oil) production, so more androgens means more skin oil is produced.
- More skin oil normally leads to more acne.14
In other words, being overweight or obese may start a chain reaction, causing an increase in insulin and leading to even more weight gain and acne.
Polycystic Ovary Syndrome – A Special Case
Some teen girls and women suffer from a hormonal disease known as polycystic ovary syndrome (PCOS). The name of the disease comes from the fact that females with PCOS often have small cysts on the ovaries. Although it is normal for women to produce small amounts of androgens, women with PCOS produce too much. This leads to other symptoms of PCOS, such as acne, weight gain and obesity, hirsutism (unusual hairiness), excess sebum, and irregular periods.5,14
For instance, in one of the studies we looked at above, in which researchers looked at Turkish females with acne, the researchers noticed that many more females with acne were unusually hairy, experienced irregular periods, and had cysts on their ovaries when compared to females without acne. The researchers also measured the amounts of androgens in each girl’s or woman’s blood and found that the higher the levels of androgens a girl or woman possessed, the higher her BMI and the more severe her acne was.5
Put simply, some females develop acne and also become overweight or obese because they suffer from PCOS, which causes their bodies to produce excess androgens.
However, the case regarding the connection between PCOS, BMI, and acne is not so cut-and-dried. A recent study conducted in Korea found that while PCOS seems to frequently go hand-in-hand with higher BMI, women with PCOS who are obese may actually be less likely to suffer from facial acne compared to women with PCOS who are at a healthy weight.15 Further research is necessary to clarify the relationship between BMI and facial as well as body acne in women with PCOS.
Diet

A Western-style diet, filled with high-glycemic (high sugar) and processed foods, and an imbalanced ratio of omega-3 to omega-6 fats, may lead to weight gain and may therefore contribute to acne.
Some scientists have found that acne, like obesity, is a disease of Western civilization and is absent in regions where people’s diets are more “natural” or similar to those of the Stone Age.16 The Stone Age, or Paleolithic Period, which represents the vast majority of human evolution, was a time when humans lived as hunters and gatherers, and their diet consisted of meats, fruits, nuts, and vegetables, with few grains, processed foods, sugar, or dairy products. In contrast, a Western diet today, which is sometimes called the Neolithic diet, typically includes high levels of processed grains, cereals, and dairy products.
Many food products which are part of the modern Western diet have a high glycemic load, which means that they are high in sugar. Consuming these foods will cause the amount of glucose in a person’s blood to increase quickly, which can lead to insulin resistance as we mentioned previously, and an ensuing hormonal chain reaction that potentially leads to weight gain and acne.16
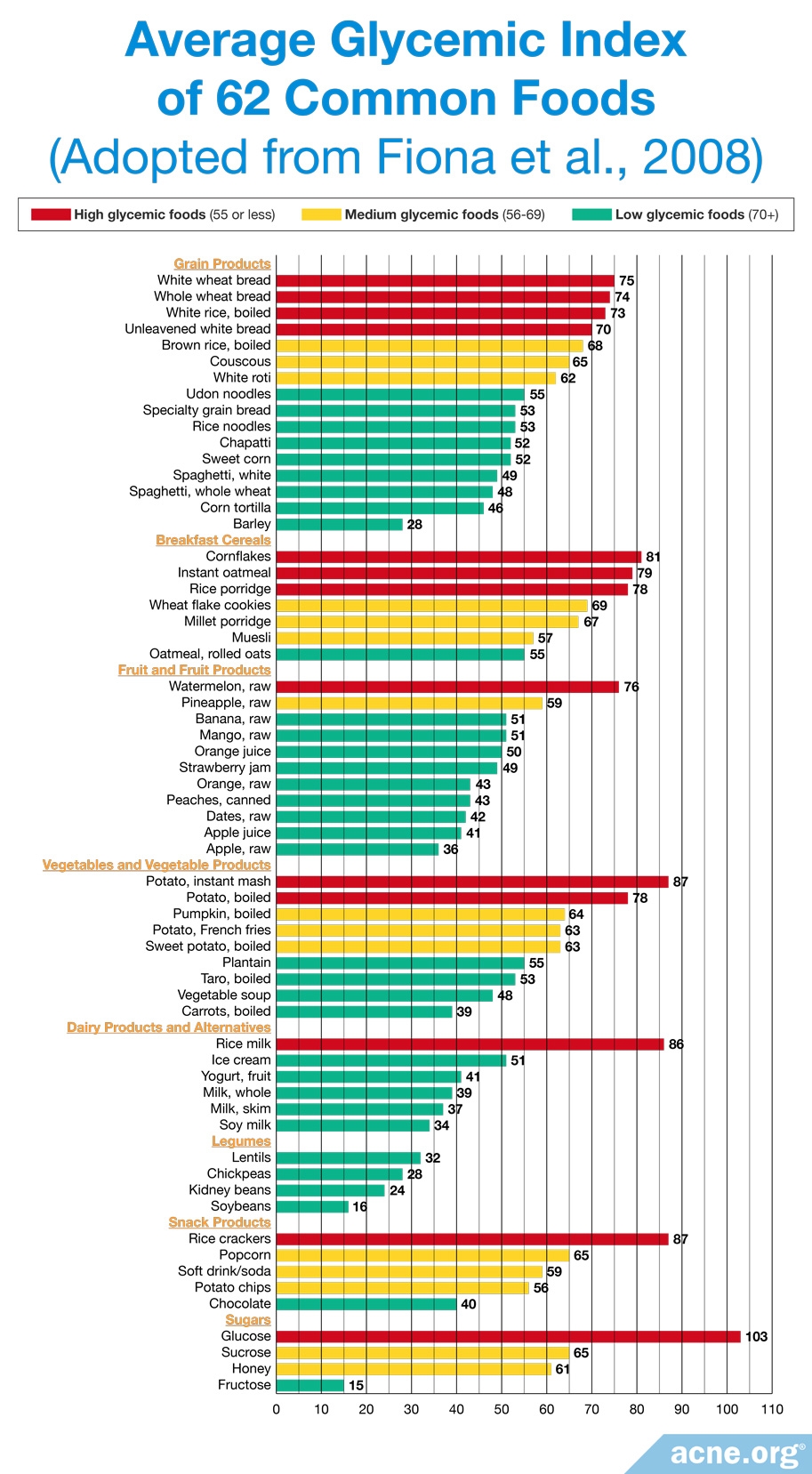
One method of determining how eating a particular food will affect your blood sugar is to view its glycemic index, which is measured in low, medium, and high categories.17
- Low (55 or less): The food is low in sugar and will not significantly increase your blood sugar
- Medium (56 – 69): The food will moderately increase your blood sugar
- High (70 or more): The food is high in sugar and will quickly increase your blood sugar
Let’s look a bit more deeply into how eating high glycemic load foods might lead to weight gain and acne. Research suggests that eating foods with a high glycemic load increases the levels of two hormones:
- Insulin
- Insulin-like growth factor 1 (IGF-1)
As we have seen, insulin can set off a chain reaction leading to both weight gain and acne.
IGF-1 is a hormone that has many effects on the body, one of which is to increase the production of androgens. As we have discussed, an increase in androgens can lead to more sebum production and more acne. In addition, IGF-1 can also directly increase the production of sebum even further.18
Let’s dive even deeper now. A diet with a high glycemic load may cause the body to produce certain substances called binding proteins. These substances play a part in synthesizing unsaturated (normally liquid at room temperature) fatty acids. Why does this matter? Because skin oil (sebum) that is abundant in unsaturated fatty acid is more likely to cause acne.16

One study tried to answer the question of whether a diet with a low glycemic load can solve the problems of both obesity and acne by putting acne patients on a 12-week low glycemic load diet. The results were promising: the patients on the low glycemic load diet lost more weight, produced less sebum, and experienced less acne overall at the end of the 12 weeks compared to patients who stayed on a high glycemic load diet.19
Expand to read details of study

The study, published in 2008 in the Journal of Dermatological Science, put acne patients on a 12-week LGL diet and compared them to acne patients who remained on a HGL diet. The researchers found that after 12 weeks, the patients had significantly less acne than patients who stayed on a HGL diet. The patients on the LGL diet also produced less sebum and lost more weight. In fact, the researchers found that the higher the patients’ BMI at the beginning of the diet, the more weight they lost over the 12 weeks.19
The results of this study suggest that a low glycemic load diet may help reduce both excess weight and acne, but more research is needed to confirm this result. It is important to note that since the patients lost weight, we cannot be sure that the weight loss is not the reason for their improved acne. That is to say, any diet or exercise regimen that caused weight loss could have been just as effective as the low glycemic load diet in reducing the patients’ acne.
“Yo-yo dieting”: Recently, some scientists have speculated that weight cycling or yo-yo dieting, in which an overweight or obese person repeatedly loses weight and then gains it back, may also contribute to acne development.20 Weight cycling appears to cause an increase in the number of fat cells, and this sets off a chain reaction in the body. One possible result is that the body begins to produce more unsaturated fatty acid. As mentioned before, sebum that contains more unsaturated fatty acid is more likely to cause acne.21,22 However, so far, no one has conducted a properly controlled study to test this idea.
In Conclusion
Overweight and obese women may suffer from more acne, while men may not. Acne in overweight or obese females may be due to increased insulin, a high-sugar diet, or a hormonal disease like PCOS. In addition, weight cycling may play a role, but there is currently no evidence to confirm this suspicion.
References
- Obesity and overweight, http://www.who.int/en/news-room/fact-sheets/detail/obesity-and-overweight
- Bourne, S. & Jacobs, A. Observations on acne, seborrhoea, and obesity. Br. Med. J. 1, 1268 – 1270 (1956). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1979692/
- Di Landro, A. et al. Family history, body mass index, selected dietary factors, menstrual history, and risk of moderate to severe acne in adolescents and young adults. J. Am. Acad. Dermatol. 67, 1129 – 1135 (2012). https://www.ncbi.nlm.nih.gov/pubmed/22386050
- Halvorsen, J. A. et al. A population-based study of acne and body mass index in adolescents. Arch. Dermatol. 148, 131 – 132 (2012). https://jamanetwork.com/journals/jamadermatology/fullarticle/1105449
- Alan, S. & Cansizoglu, E. Effects of hyperandrogenism and high body mass index on acne severity in women. Saudi. Med. J. 35, 886 – 889 (2014). https://www.ncbi.nlm.nih.gov/pubmed/25129194
- Sas, K. & Reich, A. High body mass index is a risk factor for acne severity in adolescents: A preliminary report. Acta Dermatovenerol. Croat. 27, 81-85 (2019). https://www.ncbi.nlm.nih.gov/pubmed/31351501
- Neupane, S., Basnet, B., & Sharma, T. Association between acne and body mass index: A hospital based cross sectional study. Nepal Journal of Dermatology, Venereology & Leprology, 16, 53-56 (2018). https://doi.org/10.3126/njdvl.v16i1.19408
- Anyachukwu, C., Onyeso, O. & Ezema, C. Age, body mass and physical activity determinants of facial acne severity among Southern Nigerian adolescents and young adults. The West Indian Medical Journal. (2018) https://www.mona.uwi.edu/fms/wimj/article/3682
- Snast, I., Dalal, A., Twig, G., Astman, N., Kedem, R., Levin, D., Erlich, Y., Leshem, Y.A., Lapidoth, M., Hodak, E. & Levi, A. Acne and obesity: A nationwide study of 600,404 adolescents. J. Am. Acad. Dermatol. 81, 723-729 (2019). https://www.ncbi.nlm.nih.gov/pubmed/30978426
- Chaudhary, S., Ameer, A., Sarwar, M. Z., Naqi, S. A. & Butt, A. I. A cross-sectional study of body mass index and sleep quality as risk factors to severity of acne. J. Pak. Med. Assoc. 71, 2148-2150 (2021). https://pubmed.ncbi.nlm.nih.gov/34580504/
- Alowairdhi, Y., Alrasheed, F., Alghubaywi, F., Alqirnas, M. Q. & Alajroush, W. A. Association between acne vulgaris and body mass index in adult population: A tertiary hospital-based retrospective study in Riyadh, Saudi Arabia. Cureus. 14, e32867 (2022). https://pubmed.ncbi.nlm.nih.gov/36699779/
- Rodriguez Baisi, K. E., Weaver, A. L., Shakshouk, H. & Tollefson, M. M. Acne incidence in preadolescents and association with increased body mass index: A population-based retrospective cohort study of 643 cases with age- and sex-matched community controls. Pediatr. Dermatol.40, 428-433 (2023). https://pubmed.ncbi.nlm.nih.gov/36597586/
- Kumari, R. & Thappa, D. M. Role of insulin resistance and diet in acne. Indian J. Dermatol. Venereol. Leprol. 79, 291 – 299 (2013). https://www.ncbi.nlm.nih.gov/pubmed/23619434
- Halvorsen, J. A. et al. A population-based study of acne and body mass index in adolescents. Arch. Dermatol. 148, 131 – 132 (2012). https://jamanetwork.com/journals/jamadermatology/fullarticle/1105449
- Kim, J. H., Kim, O., Jung, H., Pang, Y. & Dan, H. Body mass index, menstruation, acne, and hirsutism of polycystic ovary syndrome in women: A cross-sectional study. Health Care Women Int. 43, 85-97 (2022). https://pubmed.ncbi.nlm.nih.gov/34292855/
- Melnik, B. C. Linking diet to acne metabolomics, inflammation, and comedogenesis: an update. Clin. Cosmet. Investig. Dermatol. 8, 371 – 388 (2015). https://www.ncbi.nlm.nih.gov/pubmed/26203267
- Fiona, S. A., Kaye, F. & Jennie, C. B. International tables of glycemic index and glycemic load values: 2008. Diabetes Care 31, 2281 – 2283 (2008). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2584181/
- Melnik, B. C. & Schmitz, G. Role of insulin, insulin-like growth factor-1, hyperglycaemic food and milk consumption in the pathogenesis of acne vulgaris. Exp. Dermatol. 18, 833 – 841 (2009). https://www.ncbi.nlm.nih.gov/pubmed/19709092
- Smith, R. N. et al. The effect of a low glycemic load diet on Acne vulgaris and the fatty acid composition of skin surface triglycerides. J. Dermatol. Sci. 50, 41 – 52 (2008). https://www.ncbi.nlm.nih.gov/pubmed/18178063
- Strohacker, K., Carpenter, K. C. & McFarlin, B. K. Consequences of Weight Cycling: An increase in disease risk? Int. J. Exerc. Sci. 2, 191 – 201 (2009). https://www.ncbi.nlm.nih.gov/pubmed/25429313
- Kim, J. et al. Activation of Toll-Like receptor 2 in acne triggers inflammatory cytokine responses. J. Immunol. 169, 1535 – 1541 (2002). https://www.ncbi.nlm.nih.gov/pubmed/12133981
- Farah, D. M. & Ingham, E. Acne: Inflammation. Clin Dermatol 22, 380 – 384 (2004). https://www.ncbi.nlm.nih.gov/pubmed/15556722
 Acne.org Products
Acne.org Products