Wound Healing Is a Complex Process, but Basically Follows Four Steps: Clotting, Inflammation, Healing, and Remodeling

The Essential Info
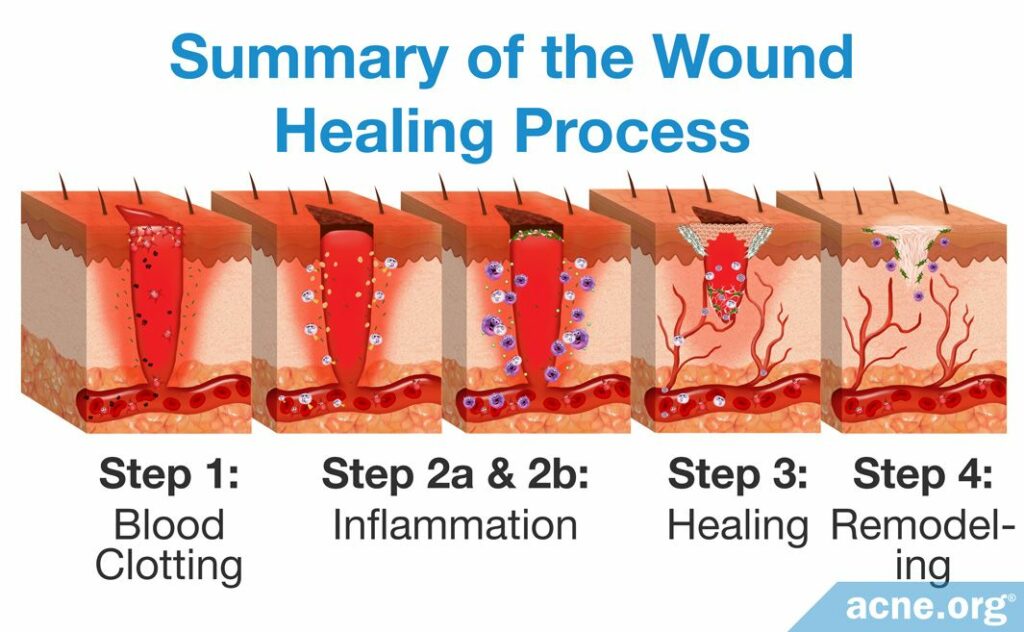
Wound healing is a complex process that involves several steps. We can simplify the process into four stages:
- Stage 1: Blood clotting: Cells stick together to form a blood clot to stop the bleeding.
- Stage 2: Inflammation: Several types of molecules, like immune molecules and inflammatory molecules, cleanse the wound and start the process of rebuilding blood vessels and skin.
- Stage 3: Healing: New skin, blood vessels, and connective tissue develop, and the wound edges begin to close.
- Stage 4: Remodeling: Scar tissue develops and becomes strong enough to allow for complete healing. This stage can last for many months or even for years and is responsible for the fading of scars over time.
Acne lesions are a form of skin wound and heal using the same process as other wounds, excluding Stage 1: Blood Clotting, because acne lesions are not bleeding cuts, so there is no need for blood clotting. The duration and severity of inflammation in an acne lesion can influence whether the lesion leaves a scar and what type of scars it causes.

The Science
The skin is a complex organ that serves as the body’s first protective barrier against the environment. Because the skin is such an important barrier, it must be able to heal itself quickly after an injury, whether the injury is a cut or an acne lesion.
The wound healing process is quite complicated. To understand how it works, we can simplify the process into four stages, which occur in this order:
- Stage 1: Blood clotting (occurs in any bleeding injury, so this stage is not part of the healing of most acne lesions)
- Stage 2: Inflammation
- Stage 3: Healing
- Stage 4: Remodeling
In reality, the process is much more complex than described here, and the various stages of wound healing often overlap. Let’s have a close look at all 4 stages of wound healing, and then we will look at how these stages are involved in the healing of acne lesions in particular.
Stage 1: Blood Clotting
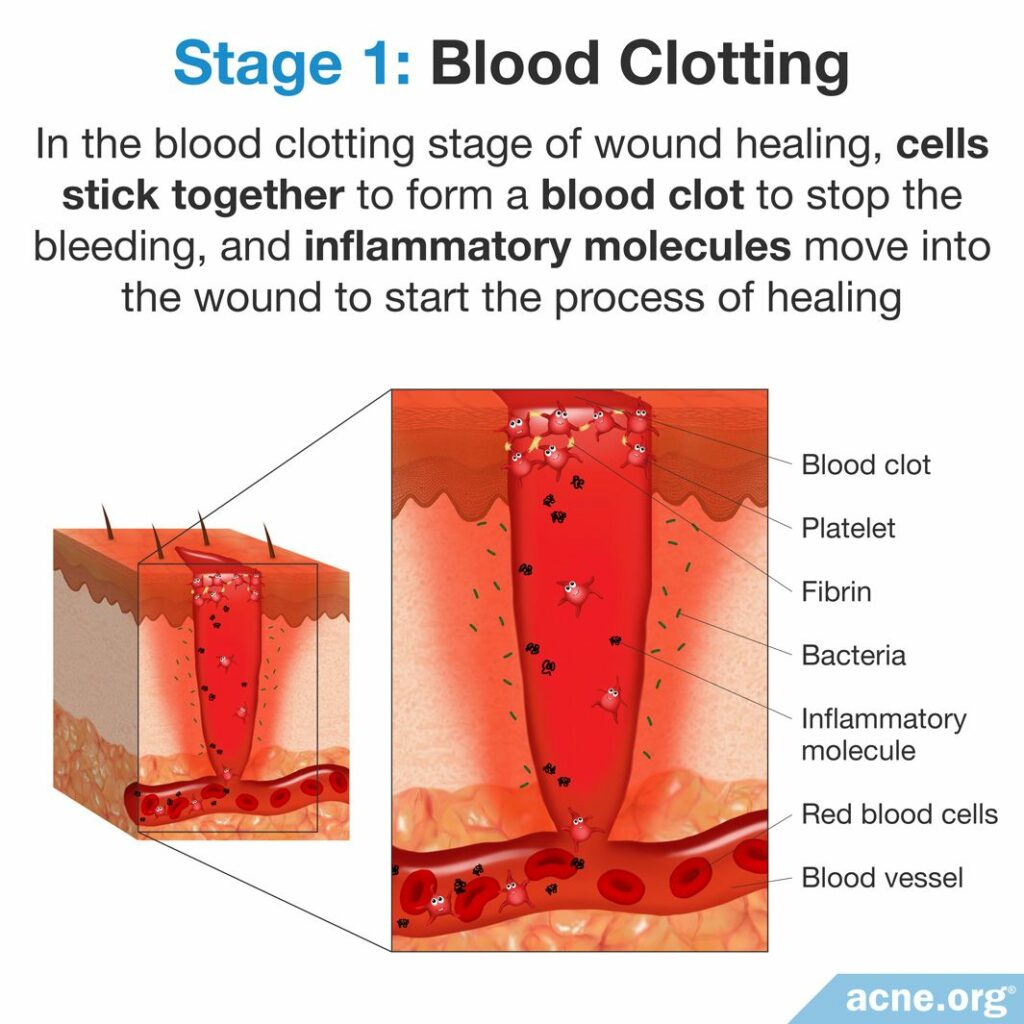
In the blood clotting stage of wound healing, cells stick together to form a blood clot to stop the bleeding, and inflammatory molecules move into the wound to start the process of healing.
Blot clot
When the skin is injured, such as in a cut, blood leaks from damaged blood vessels. Within minutes of the injury, cells called platelets move into the wound and use chemical signals to activate a protein called fibrin. Fibrin acts as a glue that sticks platelets together, forming a blood clot. The blood clot acts as a shield that protects the wound and slows or stops the bleeding.1-3
Inflammatory Molecules
At the same time, damaged cells release inflammatory molecules that cause the damaged blood vessels to narrow in order to prevent blood loss. This vasoconstriction (narrowing of the blood vessels) lasts for approximately 5-15 minutes and is then followed by a period of vasodilation (widening of the blood vessels). Vasodilation brings a variety of inflammatory, immune, and other types of molecules to the wound area to begin the healing process.1,3
Stage 2: Inflammation
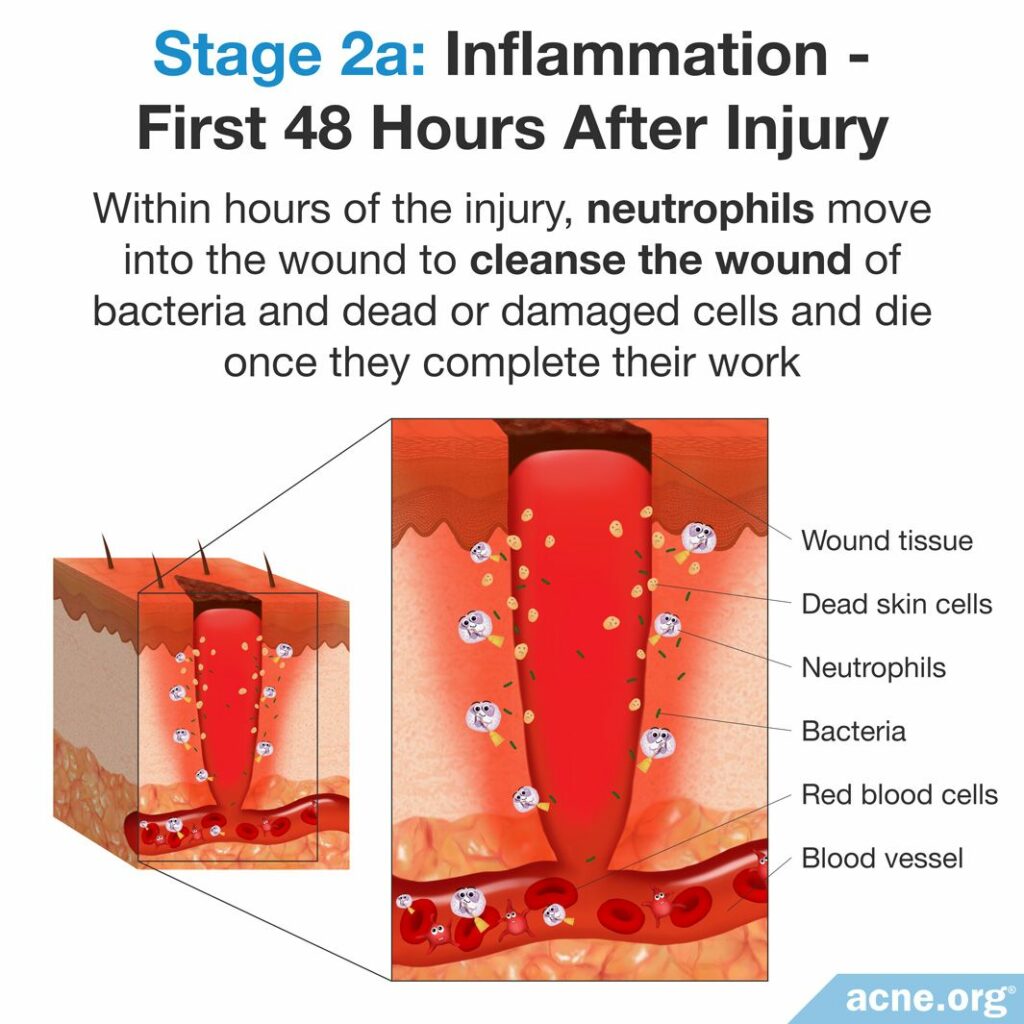
In the inflammatory stage of wound healing, immune and inflammatory cells clean up the wound and begin the process of rebuilding the blood vessels and skin.
Wound clean-up
Within hours of the injury, cells called neutrophils, which carry out both immune and inflammatory functions, move into the wound. They are the primary cells in the wound for the first 48 hours. Neutrophils cleanse the wound of bacteria and dead or damaged cells and die once they complete their work.1,3,4
Next, approximately 48 – 72 hours after the injury, other cells that carry out both immune and inflammatory functions called macrophages move into the wound. Macrophages are essential to wound healing; in fact, they are some of the most important cells during the early stages of the healing process. The macrophages finish cleansing the wound by “eating” the dead neutrophils and any remaining bacteria and dead skin cells.3,4
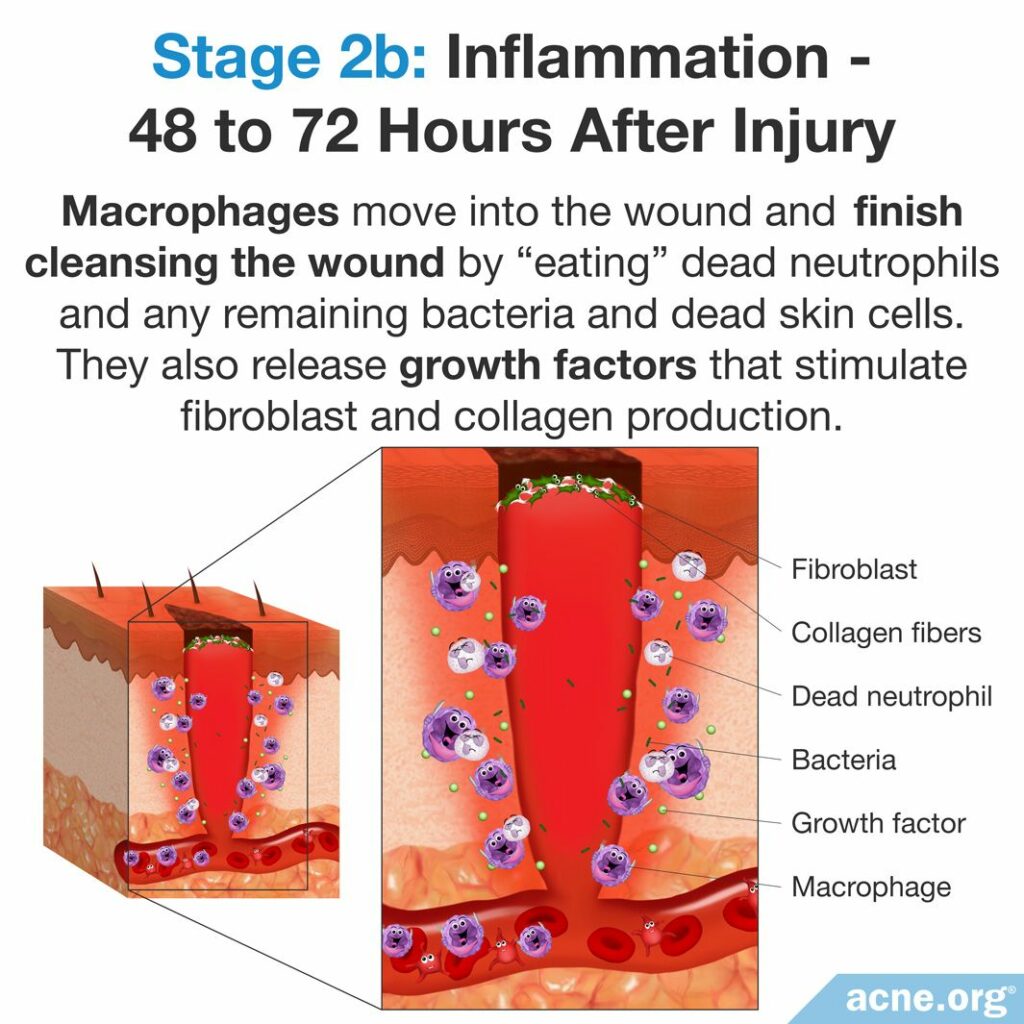
Skin regeneration
In addition to cleaning up the wound, macrophages also help with skin regeneration. They release growth factors (molecules that promote cell growth). The growth factor molecules then stimulate the production of cells called fibroblasts, which produce a protein called collagen that is essential to rebuilding both blood vessels and skin.1,3,4
Stage 3: Healing
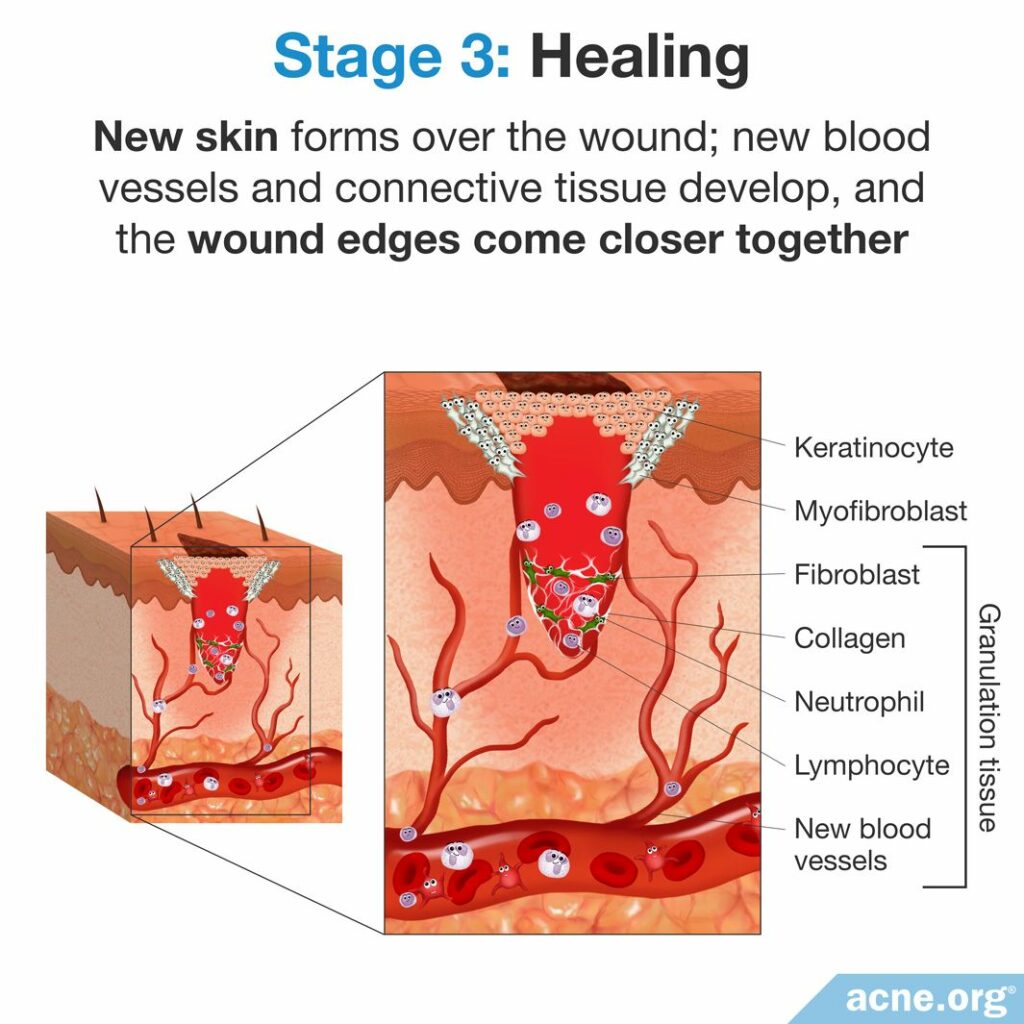
In the healing stage of wound recovery, new skin forms over the wound; new blood vessels and connective tissue develop, and the wound edges come closer together.
New skin
Beginning 24-48 hours after the injury, skin cells called keratinocytes start to close the wound. They do this by migrating slowly from the edges of the wound toward the center, making copies of themselves along the way. They continue this process until the cells from opposite sides of the wound meet in the middle. This new layer of cells is the beginning of the new skin that grows over the wound, and it provides a barrier between the wound and the environment. However, it is delicate and easily can be damaged until healing progresses further.3,4
New blood vessels and connective tissue
Within 2 – 5 days of the injury, connective tissue called granulation tissue also forms on the surface of the wound and keeps growing until it fills the entire wound. Granulation tissue consists of a combination of fibroblasts, inflammatory cells, new blood vessels, and collagen. As it grows across the wound, granulation tissue replaces the blood clot.3,4
Contraction of wound edges
During this stage, the wound contracts as its edges move toward each other. This facilitates the granulation tissue’s filling the wound. Wound contraction occurs because cells called myofibroblasts contract in the same manner as smooth muscles (muscles that we cannot control, such as those of blood vessels), drawing the edges of the wound toward each other.3,4
Stage 4: Remodeling
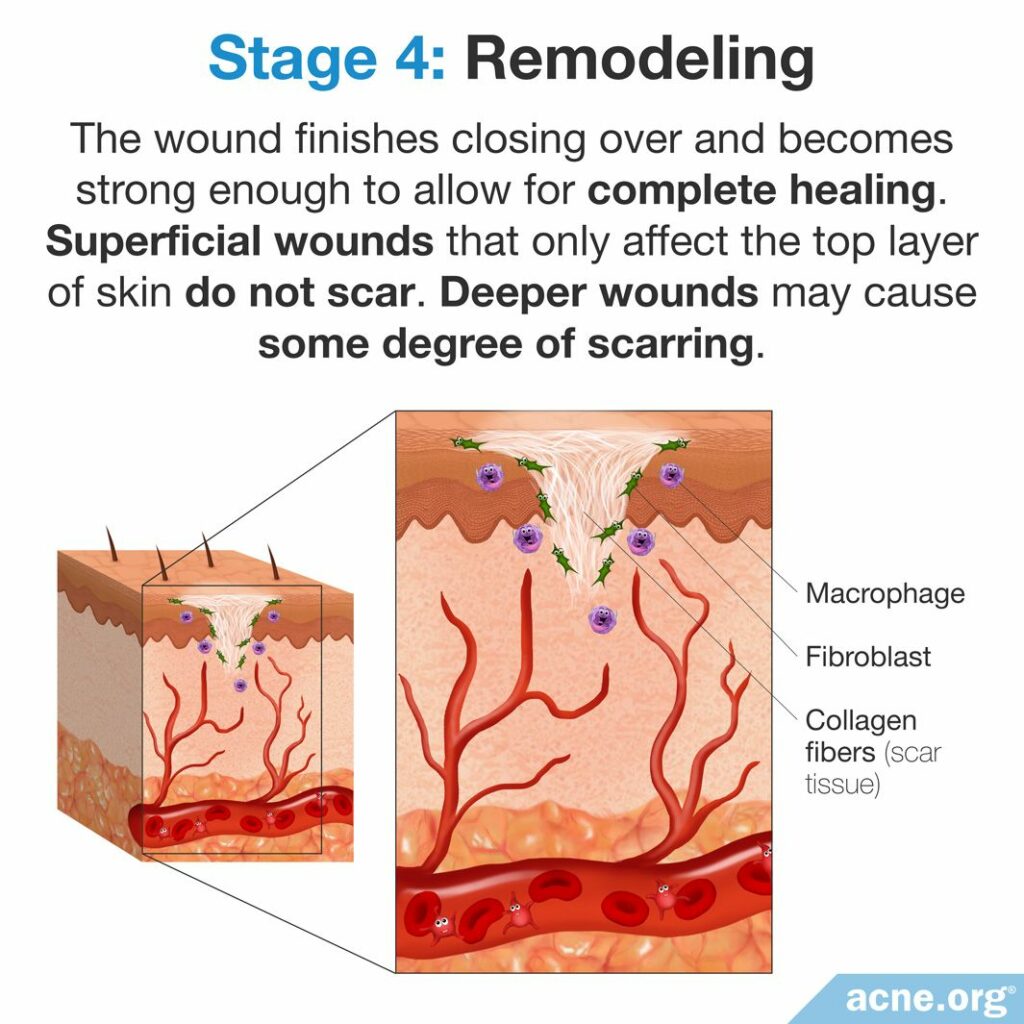
In the remodeling stage of wound healing, the wound finishes closing over and becomes strong enough to allow for complete healing. For superficial wounds, which only affect the top layer of skin, no scar is formed. However, deeper wounds may cause some degree of scarring.
Scar tissue
Approximately 21 days after the injury, more collagen moves into the wound; the water content of the wound decreases, and the collagen fibers in the wound start rearranging themselves to create a scar. In normal tissue, collagen fibers are aligned somewhat randomly in multiple directions. In contrast, in scar tissue, the collagen fibers are mostly aligned in one direction.3,5
Scar strength
During the same time, the tensile strength (ability to withstand stretching) of the scar gradually increases, meaning that the scar tissue becomes stronger and less prone to reinjury. Even with this increase in tensile strength, scar tissue is not as strong as unwounded skin. The scar reaches its peak strength approximately 60 days after the injury, and at its peak it is only about 80% as strong as normal tissue.3,5
The remodeling stage of wound healing can last for many months or even for years. This stage is responsible for the scars becoming less noticeable over time.3,5
Acne Healing
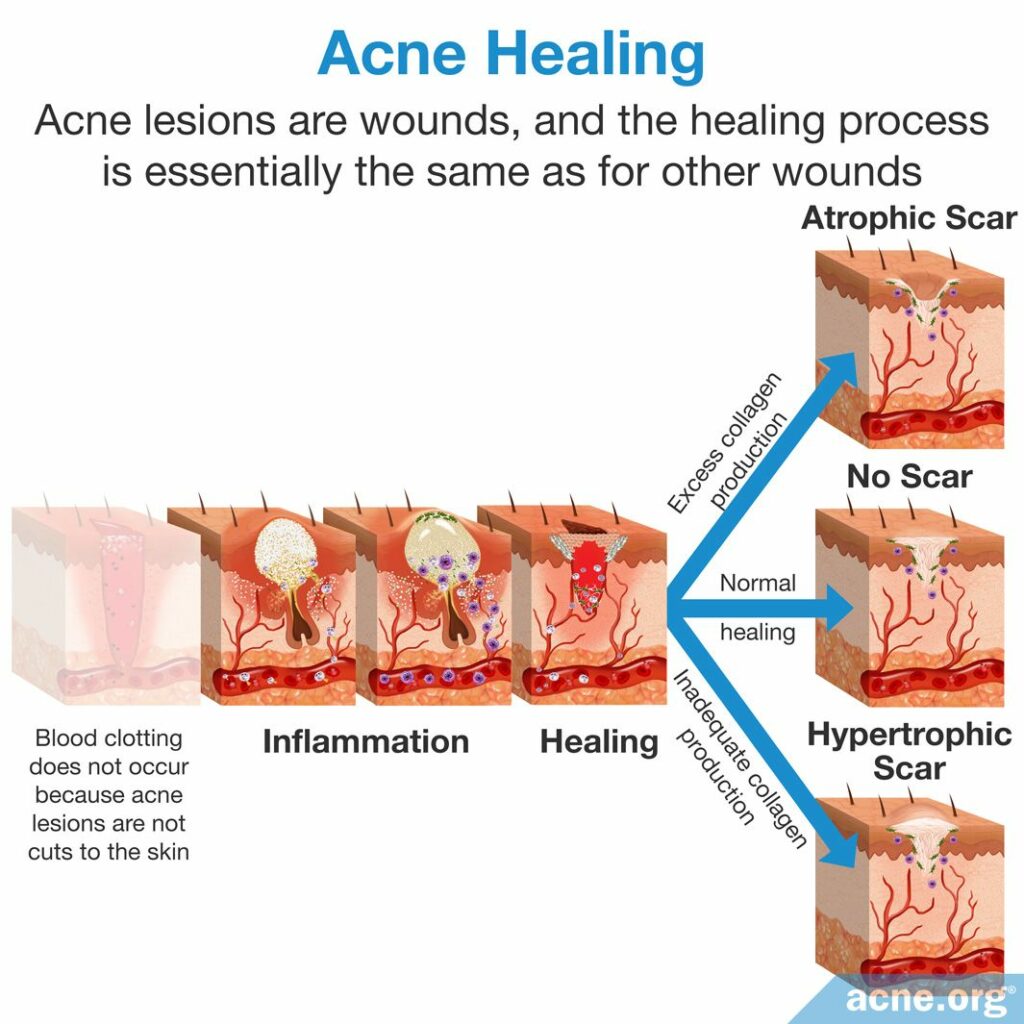
Acne lesions are wounds, and the healing process is essentially the same as for other wounds. The exception is that there are only three stages because acne lesions are not cuts to the skin, so blood clotting does not occur.
- Stage 1: Inflammation
Inflammatory molecules, such as neutrophils and macrophages, move into the lesion, and the same process of cleaning the wound occurs as for other types of wounds. - Stage 2: Healing
The healing stage of an acne lesion follows the same basic steps as other types of wounds, and includes the growth of new skin and connective tissue. - Stage 3: Remodeling
The remodeling phase is also essentially the same as for other wounds, and includes collagen realignment. If the body produces more collagen than needed during the remodeling stage, a raised scar called a hypertrophic scar forms. If the body produces less collagen than is needed, an indented scar called an atrophic scar forms. Both hypertrophic and atrophic scars often accompany a severe form of acne called nodulocystic acne, especially if it is not treated. Milder acne lesions, such as comedones, papules, and pustules, usually heal without leaving a visible scar.6
Interestingly, research has found that inflammation that is more severe or lasts for a longer period of time increases the risk of developing scars when acne lesions heal. This risk is largely due to genetics.

As a 2010 article in Dermatology Research and Practice noted, “[This research] showed a strong relationship between severity and duration of inflammation and the development of scarring, suggesting that treating early inflammation in acne lesions may be the best approach to prevent acne scarring.”6
References
- Wound healing, https://en.wikipedia.org/wiki/Wound_healing
- Martin, P. Wound Healing–Aiming for Perfect Skin Regeneration. Science 276, 75 – 81 (1997). https://www.ncbi.nlm.nih.gov/pubmed/9082989
- Simon, P. Skin Wound Healing. (2016). https://emedicine.medscape.com/article/884594-overview#a1
- Velnar, T., Bailey, T. & Smrkolj, V. The Wound Healing Process: An Overview of the Cellular and Molecular Mechanisms. J Int Med Res 37, 1528 – 1542 (2009). https://www.ncbi.nlm.nih.gov/pubmed/19930861
- Scar, https://en.wikipedia.org/wiki/Scar
- Fabbrocini, G. et al. Acne Scars: Pathogenesis, Classification and Treatment. Dermatol Res Pract 2010, 1 – 13 (2010). https://www.ncbi.nlm.nih.gov/pubmed/20981308
 Acne.org Products
Acne.org Products