No One Knows, but Scientists Speculate That Humidity Might Play a Role in Acne Development or the Appearance of Acne

The Essential Info
Researchers have not yet identified whether humidity increases acne symptoms, but some researchers hypothesize that humidity might worsen acne by:
- Disrupting the microbial balance in the skin – in other words, allowing for the growth of more acne bacteria
- Decreasing the function of the skin barrier – in other words, making the skin more vulnerable to disease
- Clogging sweat glands – in other words, creating bumps on the skin that look like acne but are actually clogged sweat glands
More research is needed to evaluate each of these possible issues in order to draw any conclusions on whether or how humidity affects acne.
My Experience and Thoughts: I’m only one person, so it’s purely anecdotal, but I grew up in Pennsylvania, where it’s very humid during the summer, and my acne was usually worse in the summer months. My own personal hypothesis on humidity is that it “plumps” the skin. Follow along with me here…when humidity and heat plumps up your skin, it expands. Now imagine going inside your skin, into a pore. When the skin around the pore plumps up, the pore walls are forced together. And anything that forces pore walls to touch might lead to them sticking together. Clogged pores are the first step in acne development, so perhaps it’s this expansion of the skin that leads to more acne. However, even if I’m right, there’s not much that anyone can do about humidity, so there’s no point in obsessing about it. After I found The Regimen, I was able to keep my skin clear even in the summer months.

The Science
- Seasons & Acne
- Altitude & Acne
- Geographical Location & Acne
- How Humidity Might Make Acne Worse
- The Bottom Line
Scientists have not performed any research that directly investigates the effect of humidity on acne severity. Therefore, to determine whether it may play a role, we must rely on studies that investigate the effect of:
- Seasons & acne: Summer is the most humid season
- Altitude & acne: Lower altitudes tend to be more humid
- Geography & acne: Certain places in the world are more humid than others
However, even when we look at these studies, due to a variety of conflicting conclusions, we can’t definitively say whether humidity affects acne. This is the case sometimes in science. We must simply say “we don’t know” until we get more data. Still, let’s have a closer look at the studies we do have and see what we can discover.
Seasons & Acne (summer is the most humid season)
Scientists have performed several studies that investigated the relationship between seasons and acne severity. Since summer is normally the most humid season, this could potentially give us a clue into how humidity might factor into acne.
However, many of these studies simply involved asking young people to answer surveys. This is called participant self-reporting and is known to be an unreliable scientific method.
Some studies have found a link between humid seasons and increased acne, others have found the opposite or observed no seasonal pattern at all. Therefore, if there is a link between humid times of the year and acne, it is likely to be fairly weak. In other words, based on the evidence we have thus far, the jury is still out on whether acne is worse in particular seasons.1-5
Expand to read details from studies

For example, a 2002 study published in The Journal of Dermatology interviewed 452 Indian participants about seasonal changes and acne worsening. The researchers found that the majority of participants reported acne worsening during the summer season. Further, many of the participants believed that the acne exacerbation was due to increased sweating and humidity. However, this study relied solely on participant self-reporting, which is unreliable.3

A 2009 study published in the International Journal of Dermatology interviewed Nigerian high school students regarding their beliefs about what causes acne. Five percent of the participants believed that humidity could exacerbate acne. Although this study shows that some people believe humidity can cause acne, it once again relies on self-reporting and does not provide reliable scientific evidence on how humidity could influence acne.4

A 2019 study published in the Journal of Cosmetic Dermatology tracked seasonal variation in acne in 171 Indian patients. The researchers graded the patients’ acne over the course of a year and also questioned the patients about changes they had noticed in their acne. Among patients who noticed changes in their acne with the season, 40.4% reported worsening in summer. The researchers attributed this increase in acne to heat and humidity.5 However, we should note that according to their findings, the humidity in India is almost the same year-round, while the temperature increases significantly in the summer.
Another group of researchers looked at data collected between 2002 and 2016 that analyzed hospital records in Saudi Arabia, Turkey, and Yemen. They found that many patients reported acne during the winter season, when humidity normally decreases.6-8
Similarly, another team of researchers examined data from 10,999 patients in Spain who saw a doctor for their skin conditions in 2016. The researchers found that a diagnosis of acne was more common during the cold period of the year.9 However, in Spain, the coldest months actually tend to be the most humid. In other words, this finding supports the idea that more humidity might mean more acne.
Finally, another set of researchers looked at the data from Iranian acne patients and found no correlation between seasons and acne severity.10-12
Altitude & Acne (lower altitudes tend to be more humid)
As altitude increases, humidity tends to decrease.
Scientists have performed only two studies, both in 2013, investigating the effect of altitudes on acne.
Again we see conflicting results, with one study finding that high altitudes might lead to more acne and the other study finding the opposite, that high altitudes might lead to less acne.13,14
Expand to read details of studies

A 2013 study published in the Indian Journal of Dermatology investigated the incidence of skin diseases in high altitudes. The researchers found that “low humidity, high velocity wind, UV exposure, and cold temperatures” are the main causes of skin diseases, including acne, in higher altitudes. They therefore predicted that lower humidity probably increases acne and other skin diseases in higher altitudes.13

A separate 2013 study published in the European Journal of Pediatrics examined the effect of altitude on acne in 6200 boys. They found that boys living in higher altitudes had less acne when compared to boys living in lower altitudes. However, the researchers did not identify if humidity or other factors–including temperature, UV exposure, or wind–contributed to less acne in the boys who lived in higher altitudes.14
Geographical Location & Acne (certain places in the world are more humid than others)
Researchers have performed several studies to identify if acne prevalence changes depending on where people live. They have also performed studies to see if acne symptoms change during temporary travel to a new area.
Overall, researchers have not yet identified if living in certain climates may cause people to be more or less prone to acne. However, some evidence suggests that short-term travel does not affect acne severity.
Expand to read details from studies
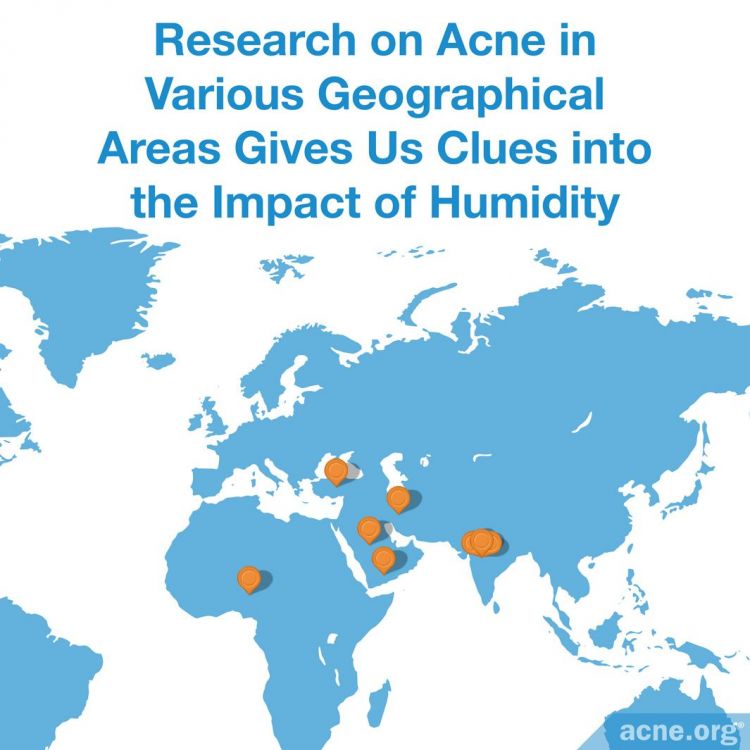
Living in Certain Geographical Locations

A 2012 study published in the International Journal of Dermatology investigated a skin condition called pityrosporum folliculitis, which causes acne-like eruptions on the skin. This study found that pityrosporum folliculitis occurred more often in men but not in women who lived in hot and humid climates. However, it is unclear if the results from studying this condition directly correlate with acne.15

A 2016 study published in the Indian Journal of Dermatology investigated the prevalence of skin diseases in people from a variety of ethnic groups living on a small group of islands east of the Indian mainland. The researchers found that the prevalence of acne and other skin diseases on these islands was similar to that of other hot, humid areas of India.16

A 1983 study published in the Indian Journal of Dermatology investigated whether military personnel were more likely to develop acne when traveling in hot and humid areas. The researchers found that only one soldier developed acne after traveling to the new, more humid area. As this is only one case, no conclusions can be drawn regarding traveling and acne.17

A 1997 study published in the Indian Journal of Dermatology, Venereology, and Leprology found that short-term travel to more humid areas did not affect the acne severity of Iranian high school students.11

A 2013 study published in The Nigerian Postgraduate Medical Journal examined the incidence of skin diseases in prison inmates living in a tropical part of Southwest Nigeria that is high in humidity. The researchers found that the tropical environment, stress, and overcrowding of the prison all contributed to the development of skin diseases, including acne. However, the study failed to note if humidity was an important factor in acne development.18
How Humidity Might Make Acne Worse
Although scientists have not yet determined whether humidity levels affect acne severity, they have proposed four mechanisms that could hypothetically connect humidity with worsening of acne.
1. Microbial Imbalance
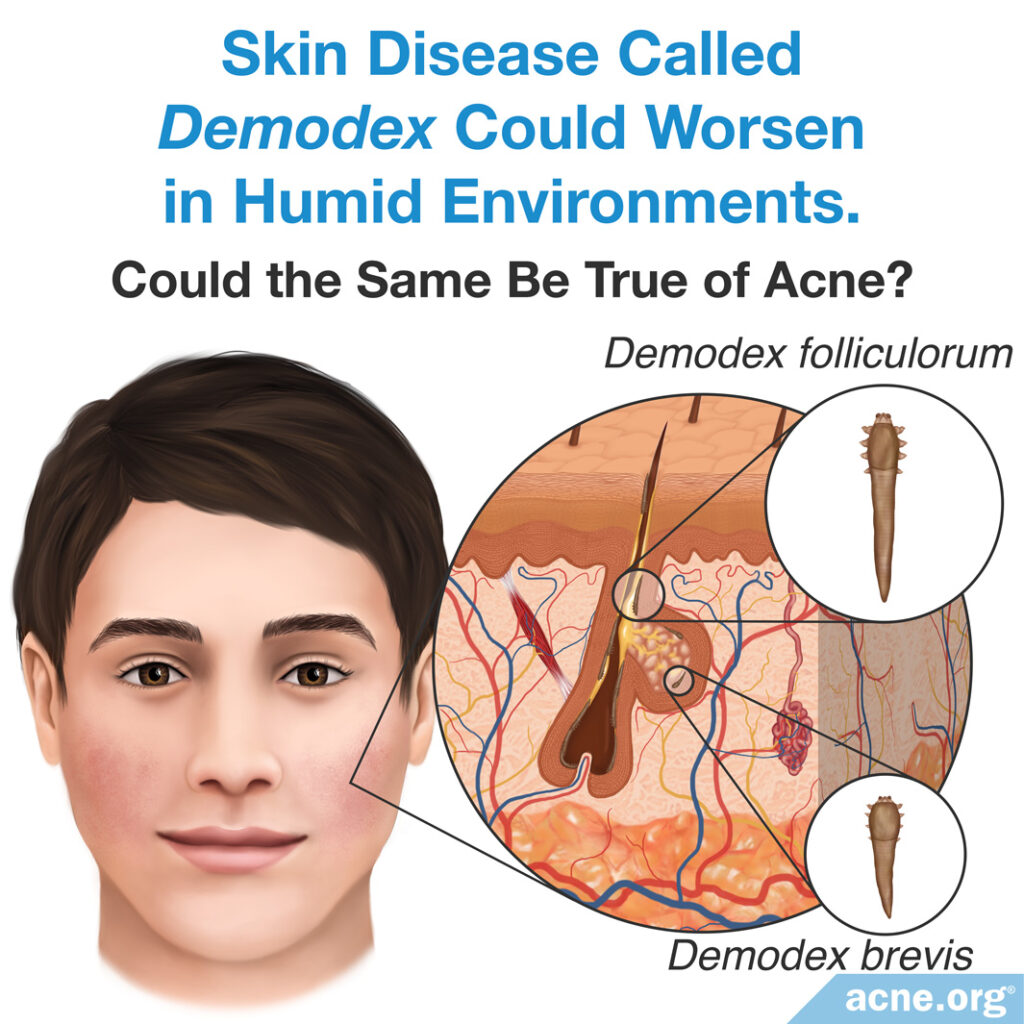
Skin health depends on microbes (micro-organisms) and bacteria that support the skin barrier and immune system. These microbes and bacteria also help prevent diseases like acne. When humidity increases, the excess moisture can promote microbial growth and cause an unhealthy imbalance of microbes in the skin, which may exacerbate acne. One 2009 study found that a skin disease called Demodex could worsen in humid environments, so it is hypothesized that the same might be true of acne.19,20
2. Oily Skin

When the body temperature rises, the skin secretes more skin oil onto the surface of the skin.
While this has not been shown to cause acne, a 2012 study discovered that skin oiliness increases in hot and humid environments. However, the observed increase in skin oiliness was not due to a larger amount of skin oil, but instead a thinning of the oil’s consistency. This lends credibility to an argument that heat and humidity would result in less acne since acne occurs when sebum becomes trapped inside the pore. However, this is hypothetical, and there is no evidence that the resulting increased skin oil excretion from hot and humid weather helps reduce acne.21
3. Impaired Skin Barrier
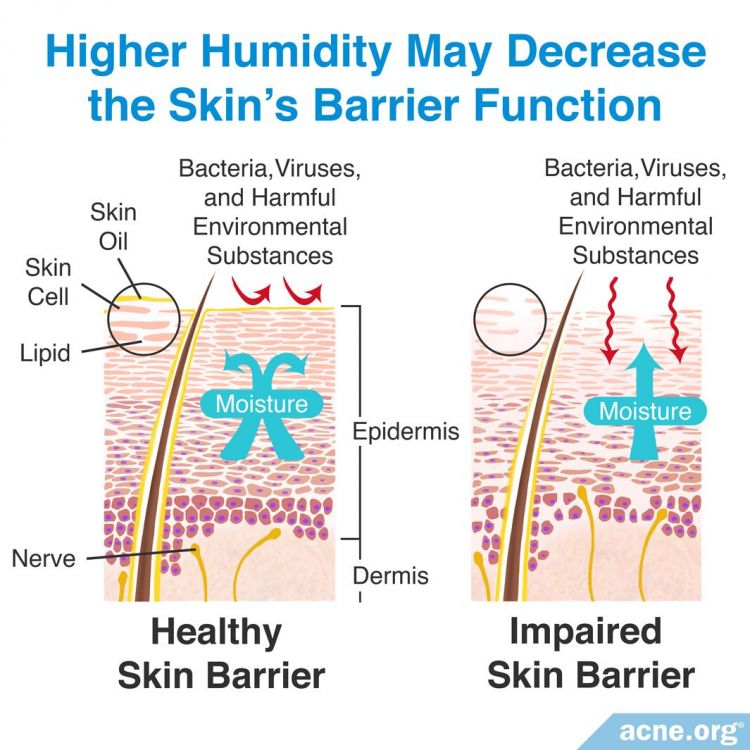
The skin acts as an important barrier protecting the body from harm.
Many skin diseases, including acne, often come with a disrupted barrier. Researchers have proposed that higher humidity may decrease the skin’s barrier function, particularly in acne-prone skin, which seems to be more vulnerable to seasonal changes.22 This could increase the severity of acne, but it may also increase the level of permeation of skin medications that can be used to treat acne. Either way, many researchers believe that higher humidity may make the skin more permeable.23,24
4. Sweat Gland Interactions

Research has shown that sweat remains on the skin longer in a humid environment than a less humid one. This lingering sweat can cause sweat ducts to clog and produce a small red bump on the skin. Although clogging of sweat ducts is not acne, it appears similar to acne.
The Bottom Line
Although scientists have performed numerous studies investigating the effects of seasons, altitude, and geography on humidity and acne, they have not yet identified whether humidity increases acne symptoms. Researchers must perform more reliable, carefully controlled studies investigating this association.
References
- Adityan, B. & Thappa, D. M. Profile of acne vulgaris–a hospital-based study from South India. Indian J Dermatol Venereol Leprol 75, 272 – 8 (2009). https://www.ncbi.nlm.nih.gov/pubmed/19439880
- Ghosh, S. K. et al. The ‘holi’ dermatoses: annual spate of skin diseases following the spring festival in India. Indian J Dermatol54, 240 – 2 (2009). https://www.ncbi.nlm.nih.gov/pubmed/20161854
- Sardana, K., Sharma, R. C. & Sarkar, R. Seasonal variation in acne vulgaris–myth or reality. J Dermatol 29, 484 – 8 (2002). https://www.ncbi.nlm.nih.gov/pubmed/12227481
- Yahya, H. Acne vulgaris in Nigerian adolescents–prevalence, severity, beliefs, perceptions, and practices. Int J Dermatol 48, 498 – 505 (2009). https://www.ncbi.nlm.nih.gov/pubmed/19416381
- Narang, I., Sardana, K., Bajpai, R. & Garg, V. K. Seasonal aggravation of acne in summers and the effect of temperature and humidity in a study in a tropical setting. J Cosmet Dermatol 18, 1098-1104 (2019). https://www.ncbi.nlm.nih.gov/pubmed/30238598
- Al-Ameer, A. M. & Al-Akloby, O. M. Demographic features and seasonal variations in patients with acne vulgaris in Saudi Arabia: a hospital-based study. Int J Dermatol 41, 870 – 1 (2002). https://www.ncbi.nlm.nih.gov/pubmed/12492972
- Tamer, E. et al. Prevalence of skin diseases among pediatric patients in Turkey. J Dermatol 35, 413 – 8 (2008). https://www.ncbi.nlm.nih.gov/pubmed/18705828
- Al-Kamel, M. A. Spectrum of winter dermatoses in rural Yemen. Int J Dermatol 55, 512 – 7 (2016). https://www.ncbi.nlm.nih.gov/pubmed/26341716
- Gonzalez-Cantero, A., Arias-Santiago, S., Buendía-Eisman, A., Molina-Leyva, A., Gilaberte, Y., Fernández-Crehuet, P., Husein-ElAhmed, H., Viera-Ramírez, A., Fernández-Peñas, P., Taberner, R., Descalzo, M.A. & García-Doval, I. Do dermatologic diagnosis change in hot vs. cold periods of the year? A sub-analysis of the DIADERM national sample (Spain 2016). Actas Dermosifiliogr 110, 734-743 (2019). https://www.ncbi.nlm.nih.gov/pubmed/30982569
- Gfesser, M. & Worret, W. I. Seasonal variations in the severity of acne vulgaris. Int J Dermatol 35, 116 – 7 (1996). https://www.ncbi.nlm.nih.gov/pubmed/8850040
- Ghodsi, S. Z., Orawa, H. & Zouboulis, C. C. Prevalence, severity, and severity risk factors of acne in high school pupils: a community-based study. J Investig Dermatol 129, 2136 – 41 (2009). https://www.ncbi.nlm.nih.gov/pubmed/19282841
- Weiss, S. C., Rowell, R. & Krochmal, L. Impact of seasonality on conducting clinical studies in dermatology. Clin Dermatol 26, 565 – 9 (2008). https://www.ncbi.nlm.nih.gov/pubmed/18755376
- Robeva, R. et al. Acne vulgaris is associated with intensive pubertal development and altitude of residence–a cross-sectional population-based study on 6,200 boys. Eur J Pediatr 172, 465 – 71 (2013). https://www.ncbi.nlm.nih.gov/pubmed/23247617
- Singh, G. et al. Incidence and care of environmental dermatoses in the high-altitude region of ladakh, India. Indian J Dermatol58, 107 – 12 (2013). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3657208/
- Poli, F. Differential diagnosis of facial acne on black skin. Int J Dermatol 51 Suppl 1, 24 – 6, 7 – 9 (2012). https://www.ncbi.nlm.nih.gov/pubmed/23210948
- Subramaniyan, R. Pattern of Dermatoses Among Nicobarese in a Community Health Camp at Nancowry, Andaman and Nicobar Islands. Indian J Dermatol 61, 187 – 9 (2016). https://www.ncbi.nlm.nih.gov/pubmed/27057019
- Tucker, S. B. Occupational tropical acne. Cutis 31, 79 – 81 (1983). https://www.ncbi.nlm.nih.gov/pubmed/6218968
- Oninla, O. A. et al. Pattern of dermatoses among inmates of Ilesha Prison, Nigeria. Niger Postgrad Med J 20, 174 – 80 (2013). https://www.ncbi.nlm.nih.gov/pubmed/24287746
- Grice, E. A. & Segre, J. A. The skin microbiome. Nature Rev Microbiol 9, 244 – 53 (2011). https://www.nature.com/articles/nrmicro2537?draft=collection
- Cao, Y. S. et al. [Facial Demodex infection among college students in Tangshan]. Zhongguo Ji Sheng Chong Xue Yu Ji Sheng Chong Bing Za Zhi 27, 271 – 3 (2009). https://www.ncbi.nlm.nih.gov/pubmed/19852374
- Sakuma, T. H. & Maibach, H. I. Oily skin: an overview. Skin Pharmacol Physiol 25, 227 – 35 (2012). https://www.ncbi.nlm.nih.gov/pubmed/22722766
- Pappas, A., Kendall, A. C., Brownbridge, L. C., Batchvarova, N. & Nicolaou, A. Seasonal changes in epidermal ceramides are linked to impaired barrier function in acne patients. Exp Dermatol 27, 833-836 (2018). https://pubmed.ncbi.nlm.nih.gov/29356138/
- Suskind, R. R. Environment and the skin. Environ Health Perspect 20, 27 – 37 (1977). https://www.ncbi.nlm.nih.gov/pubmed/413711
- Wiechers, J. W. The barrier function of the skin in relation to percutaneous absorption of drugs. Pharm Weekbl Sci 11, 185 – 98 (1989). https://www.ncbi.nlm.nih.gov/pubmed/2694089
 Acne.org Products
Acne.org Products